NSTIs: The Basics - Flesh-Eater Files
- Rapidly progressive infections; extensive necrosis of skin, subcutaneous tissue, fascia; systemic toxicity.
- Classification & Key Organisms:
- Type I (Polymicrobial): Most common (~70-80%). Mixed aerobes & anaerobes (e.g., E. coli, Bacteroides). Often post-surgery, diabetics.
- Type II (Monomicrobial): Group A Streptococcus (GAS) ± Staph. aureus. "Flesh-eating bacteria"; severe pain out of proportion.
- Type III (Gas Gangrene): Clostridium spp. (esp. C. perfringens). Myonecrosis, crepitus.
- Type IV (Fungal): Rare. Candida, Zygomycetes. Severe immunocompromise.

⭐ Fournier's gangrene is a Type I NSTI of the perineal/genital regions, often polymicrobial.
NSTIs: Pathogenesis & Risks - Vulnerability Scan
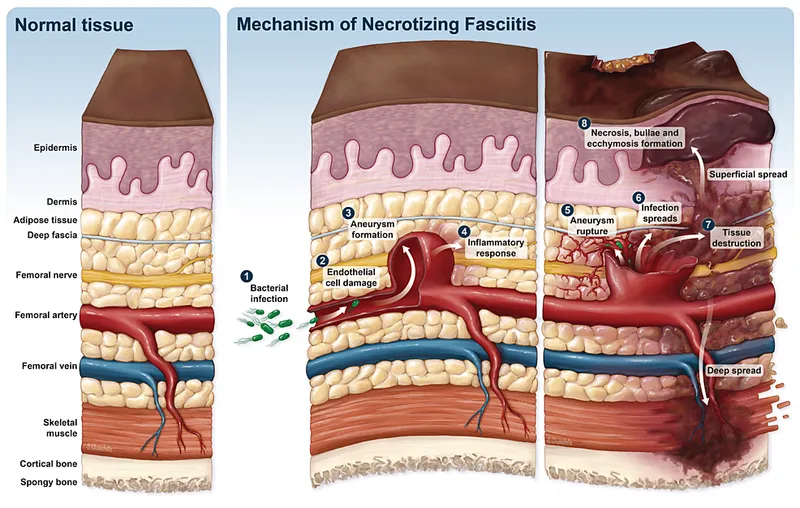
- Pathogenesis:
- Bacterial invasion (often polymicrobial - Type I; or monomicrobial e.g., Group A Strep - Type II, Vibrio vulnificus - Type III).
- Synergistic release of toxins & enzymes (hyaluronidase, collagenase).
- Leads to: Microvascular thrombosis → tissue ischemia & liquefactive necrosis. Gas (crepitus) may be present.
- Major Risk Factors:
- Diabetes Mellitus (most common, ↑↑ risk)
- Peripheral Vascular Disease (PVD)
- Immunosuppression (steroids, HIV, chemotherapy)
- Recent surgery or trauma (even minor)
- IV drug use
- Obesity, Chronic Kidney/Liver Disease
⭐ Fournier's gangrene is a specific NSTI of the perineum, genitals, or perianal area; often polymicrobial and carries high mortality.
NSTIs: Clinical Clues & Diagnosis - Code Red Alert
- Clinical Clues (Red Flags):
- Excruciating pain, disproportionate to signs (POOP) - earliest clue.
- Tense edema, extending beyond erythema.
- Skin: dusky hue, violaceous bullae, necrosis.
- Systemic toxicity: fever (>38°C), tachycardia (>100 bpm), hypotension, delirium.
- Rapid deterioration despite antibiotics.
- 📌 Mnemonic "CREEP": Crepitus, Rapid progression, Edema beyond erythema, Ecchymosis/Bullae, Pain out of proportion.
- Diagnosis:
- Urgent clinical diagnosis is key; don't delay surgery for imaging if high suspicion.
- LRINEC Score: (Lab Risk Indicator for Necrotizing Fasciitis)
- Aids risk stratification (Parameters: CRP, WBC, Hb, Na, Creatinine, Glucose).
- Score ≥6 indicates high risk; ≥8 strongly predictive.
- Imaging (if diagnosis uncertain & patient stable):
- X-ray: subcutaneous gas (late sign).
- CT/MRI: fascial thickening, fluid collections, gas (more sensitive).
- Definitive: Surgical exploration, debridement, & tissue biopsy (culture, histopathology).

⭐ Pain out of proportion to clinical findings is the earliest and most classic symptom of NSTI, often preceding cutaneous signs.
NSTIs: Management Strategy - Surgical & Medical Assault
Core Principle: Rapid, aggressive, combined approach.
Surgical Assault:
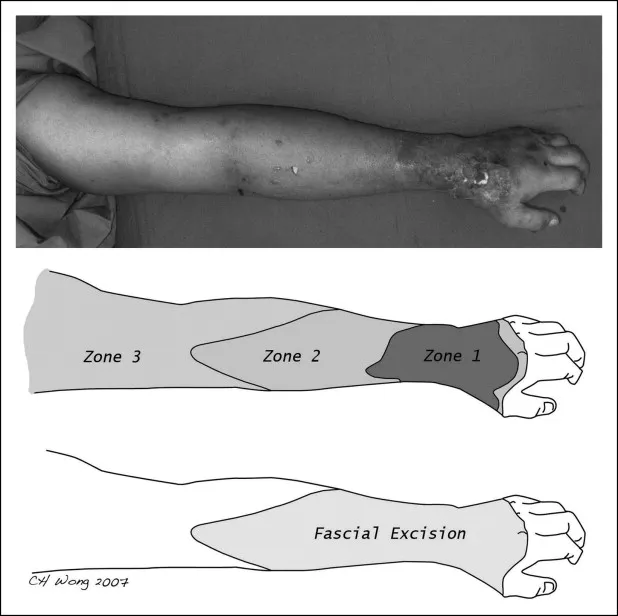
- Immediate, radical debridement: Cornerstone! Excise ALL necrotic tissue to healthy, bleeding margins.
- Second-look surgery within 12-24 hrs.
- Fasciotomy: If compartment syndrome.
- Amputation: For extensive necrosis or non-viable limb.
- Wound care post-op: e.g., Negative Pressure Wound Therapy (NPWT).
Medical Assault:
- Hemodynamic stabilization: Aggressive IV fluids, vasopressors.
- Empiric Broad-Spectrum Antibiotics (IV):
- Vancomycin/Linezolid (MRSA) +
- Piperacillin-Tazobactam/Carbapenem (Gram-neg, anaerobes) +
- Clindamycin (↓ toxin production).
- Tailor antibiotics to culture results.
- Supportive care: Nutrition, tetanus prophylaxis, manage comorbidities.
- Consider: IVIG (Strep TSS), Hyperbaric Oxygen (HBO).
⭐ Clindamycin is vital for its anti-toxin effect, especially in Group A Strep infections, reducing mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- NSTIs are life-threatening, rapidly spreading infections with extensive soft tissue necrosis.
- Severe pain out of proportion to clinical findings is a key indicator.
- Type I is polymicrobial; Type II is monomicrobial (e.g., Streptococcus pyogenes).
- Fournier's gangrene involves the perineum; gas gangrene (clostridial) presents with crepitus.
- Early diagnosis is clinical; LRINEC score can be a useful adjunct.
- Treatment pillars: Urgent, wide surgical debridement, broad-spectrum IV antibiotics, and intensive supportive care.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

