Pain Fundamentals - Know Thy Foe
- Pain Types:
- Nociceptive: Due to actual or threatened tissue damage.
- Somatic: Sharp, dull, aching, well-localized (skin, muscle, bone).
- Visceral: Deep, cramping, poorly localized (internal organs).
- Neuropathic: Caused by a lesion or disease of somatosensory nervous system. Burning, shooting, tingling.
- Nociceptive: Due to actual or threatened tissue damage.
- Pain Pathway (Simplified): Transduction → Transmission (Aδ & C fibers) → Perception (CNS) → Modulation (descending inhibition).
- Assessment: Visual Analog Scale (VAS), Numeric Rating Scale (NRS 0-10), Wong-Baker FACES.
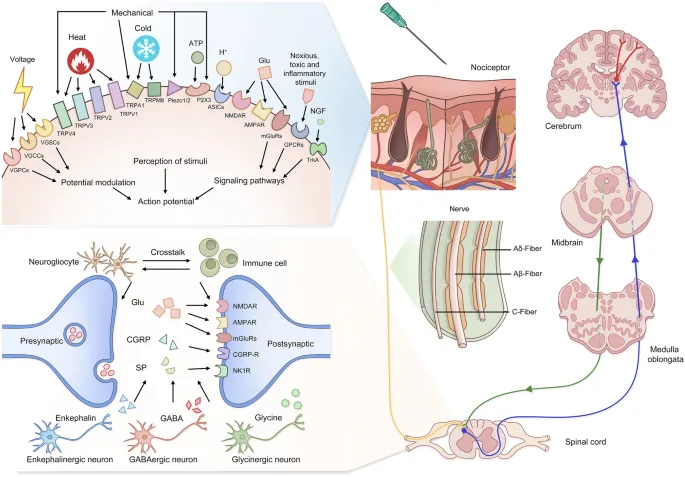
⭐ Allodynia (pain from non-painful stimuli) is a hallmark of neuropathic pain.
Multimodal Analgesia - Pain's Kryptonite
- Strategic use of ≥2 analgesic drugs/techniques targeting diverse pain mechanisms.
- Goal: Achieve superior analgesia, significantly ↓ opioid consumption (opioid-sparing) and related side effects.
- Core Elements (📌 PLAN):
- Paracetamol: Central action.
- Local/Regional Anesthesia: Nerve blocks, epidurals.
- Anti-inflammatory drugs: NSAIDs.
- Narcotics (opioids, judicious use) & Adjuvant Meds: Ketamine, gabapentinoids, lidocaine.
- Benefits: Better pain control, earlier recovery, reduced complications.
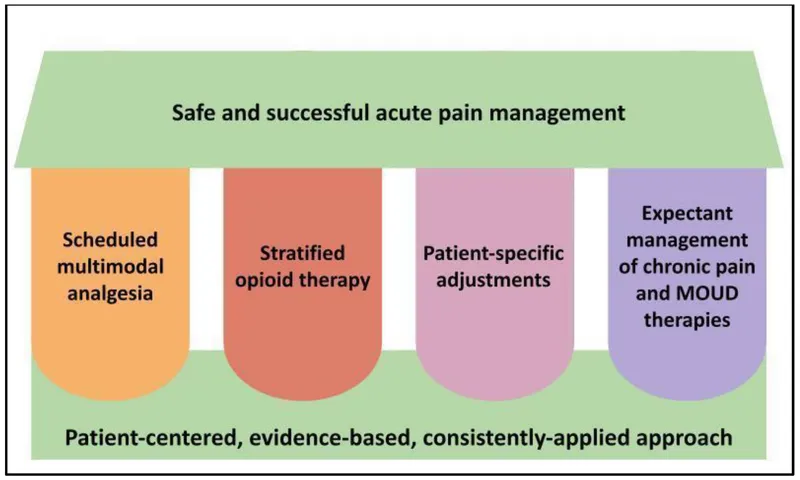
⭐ A cornerstone of ERAS (Enhanced Recovery After Surgery) protocols, significantly improving postoperative outcomes.
Non-Opioid Analgesics - Gentle Giants
- Paracetamol (Acetaminophen):
- Central analgesic, weak COX inhibitor; also antipyretic.
- Dose: 1g QID (Max 4g/day). IV/PO. Safe therapeutically.
- Minimal anti-inflammatory. Risk: Hepatotoxicity (overdose, alcohol).
⭐ Antidote for paracetamol overdose: N-acetylcysteine (NAC), most effective within 8-10h.
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs):
- COX inhibitors (↓ prostaglandins). Analgesic, anti-inflammatory, antipyretic; opioid-sparing.
- Types: Non-selective (Ibuprofen); COX-2 selective (Etoricoxib - ↓GI toxicity, CV risk persists).
- Risks: GI ulcers/bleed, renal injury (AKI), ↑CV events, platelet dysfunction.
- Ketorolac: Potent injectable, max 5 days (GI/renal toxicity).
- Avoid: PUD, renal/heart failure, AERD, pregnancy (3rd trimester).
Opioid Analgesics - Potent Power
- Mechanism: Act on μ, κ, δ opioid receptors (CNS, periphery).
- Strong Agonists:
- Morphine: Gold standard.
- Fentanyl: Potent (80-100x morphine), rapid, short-acting.
- Pethidine: Shorter acting; risk of seizures (norpethidine).
- Methadone: Long half-life; for opioid dependence.
- Atypical: Tramadol (weak μ-agonist, SNRI).
- Antagonist: Naloxone (reverses opioid overdose).
- Side Effects: Respiratory depression (⚠️), sedation, miosis (📌 except Pethidine), constipation, N/V, dependence.

⭐ Fentanyl patches: for chronic pain in opioid-tolerant patients; high risk of fatal hypoventilation if misused.
Regional & PCA - Precision Pain Punishers
- Regional Anesthesia: Targeted pain relief.
- Types: Epidural, spinal, peripheral nerve blocks (e.g., brachial plexus, femoral).
- Pros: Superior analgesia, opioid-sparing, ↓ PONV, ↓ ileus, early mobilization.
- Cons: Hypotension (esp. neuraxial), PDPH, nerve injury, hematoma, infection.
- Patient-Controlled Analgesia (PCA): Empowers patients.
- Mechanism: Patient self-administers small, preset opioid doses (IV, epidural).
- Settings: Bolus dose, lockout interval (e.g., 5-10 min), +/- basal rate (caution!).
- Drugs: Morphine, Fentanyl, Hydromorphone.
- Monitor: RR, SpO2, sedation.
⭐ PCA is contraindicated in patients unable to understand or operate the device (e.g., very young, cognitively impaired).
High‑Yield Points - ⚡ Biggest Takeaways
- Multimodal analgesia is standard: combine opioids, NSAIDs, paracetamol, and regional blocks.
- Adhere to the WHO analgesic ladder for a structured approach to pain relief.
- PCA (Patient-Controlled Analgesia) with opioids like morphine enhances patient comfort.
- Epidural analgesia provides superior pain control post major abdominal/thoracic surgery.
- NSAIDs are potent analgesics; monitor for renal, GI, and bleeding risks.
- Paracetamol is a fundamental, safe analgesic; maximum daily dose is 4g.
- Consider gabapentinoids for neuropathic pain and as opioid-sparing agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

