Indications & Timing - Recon Roadmap
- Indications:
- Post-mastectomy (cancer, prophylactic)
- Congenital (e.g., Poland syndrome)
- Severe trauma/burns
- Timing Options:
- Immediate: With mastectomy.
- Pros: Single surgery, ↑psychological well-being.
- Cons: Longer operation, potential delay to adjuvant therapy.
- Delayed: After mastectomy & adjuvant therapy.
- Pros: Oncologically safer (high-risk), patient choice.
- Cons: Multiple stages, tissue changes (fibrosis).
- Delayed-Immediate: Expander at mastectomy; final recon later.
- Balances benefits of immediate/delayed; staged approach.
- Immediate: With mastectomy.
⭐ Immediate reconstruction is generally preferred for eligible patients due to superior aesthetic and psychological outcomes, provided oncologic safety is not compromised.
Autologous Flaps - Flap Fantasia
- Uses patient's own tissue (skin, fat, +/- muscle).
- Types:
- Pedicled: Blood supply remains attached.
- Free: Blood supply detached & re-anastomosed (microsurgery).

| Flap | Pedicle(s) | Type (P/F) | Key Pro(s) | Key Con(s) |
|---|---|---|---|---|
| TRAM | Sup/Deep Inf. Epigastric | P/F | Good volume, robust | Abd. wall weakness, muscle sacrifice |
| DIEP | DIEA Perforators | F | Muscle-sparing, ↓ abd. morbidity | Technically demanding, longer OR |
| LD | Thoracodorsal A. | P/F | Reliable, salvage, good for thin pts | Back scar/seroma, often needs implant for vol. |
| SIEA | Superficial Inf. Epigastric A. | F | Muscle-sparing, ↓ donor pain | Vessel often small/absent, less reliable |
| SGAP | Sup. Gluteal A. Perf. | F | Alternative donor, good projection | Buttock contour issues, difficult positioning |
| IGAP | Inf. Gluteal A. Perf. | F | Hidden scar (IMF), good for thin pts | Sciatic nerve risk, shorter pedicle |
Implant-Based Methods - Silicone & Saline Stories

- Overview: Uses silicone or saline implants. Shorter surgery, faster recovery vs. autologous.
- Implant Types:
- Silicone Gel: Cohesive gel, natural feel. MRI for rupture detection.
- Saline: Sterile saltwater-filled. Rupture causes visible deflation. Firmer.
- Placement:
- Subglandular (prepectoral).
- Submuscular (retropectoral, often dual-plane for better coverage).
- Procedure:
- Two-Stage (Common): Tissue expander placed, gradually inflated, then exchanged for permanent implant.
- Direct-to-Implant (DTI): Single stage; requires good skin/soft tissue.
- Complications:
- Capsular Contracture (Baker I-IV).
- Implant Rupture/Deflation, Infection, Seroma.
- ⚠️ BIA-ALCL (Breast Implant-Associated Anaplastic Large Cell Lymphoma) - higher with textured surfaces.
⭐ Capsular contracture is the most frequent complication; Baker grades III and IV are clinically significant and often require surgical correction.
NAC, Complications, Adjuncts - Finessing & Fixes
- Nipple-Areola Complex (NAC) Reconstruction:
- Timing: 3-6 months post-mound creation.
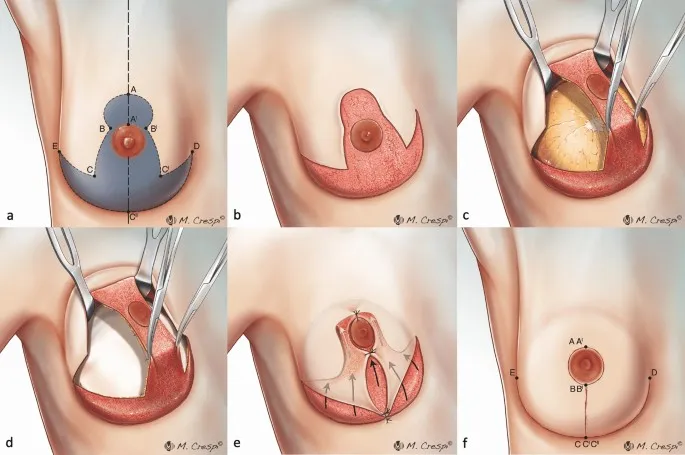
- Nipple: Local flaps (skate, C-V), composite grafts, nipple sharing.
- Areola: Full-thickness skin grafts (FTSG) (contralateral NAC, inner thigh), medical tattooing (3D).
- Complications:
- General: Hematoma, seroma, infection, dehiscence, pain, asymmetry.
- Implant-Based:
- Capsular contracture (Baker I-IV); 📌 Mnemonic: "BAKER makes implants HARD".
- Rupture, malposition, rippling, animation deformity.
⭐ Capsular contracture is the most common long-term complication of implant-based breast reconstruction. Baker Grade III/IV often requires surgical intervention.
- Autologous Flap: Partial/total flap loss, fat necrosis, donor site morbidity (hernia, seroma).
- Adjuncts & Finessing:
- Lipofilling: Contour, volume, skin quality.
- Symmetrization: Contralateral mastopexy, reduction, augmentation.
- Minor revisions: Dog-ear correction, scar revision_._
High‑Yield Points - ⚡ Biggest Takeaways
- Immediate reconstruction is common; delayed if inflammatory cancer or PMRT planned.
- Choose between autologous flaps (patient's tissue) or implant-based reconstruction.
- DIEP flap: Muscle-sparing abdominal flap, preferred for lower morbidity.
- TRAM flap: Abdominal flap with rectus muscle harvest, risks hernia/weakness.
- LD flap: Back flap, often requires an implant for volume projection.
- Implant risks: Capsular contracture, rupture, infection, and BIA-ALCL.
- Nipple-areola complex (NAC) reconstruction is a separate, staged procedure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

