Laparoscopic Access: Foundations - Prepping the Canvas
- Indications: Diagnostic (e.g., unexplained pain, staging laparoscopy) & Therapeutic (e.g., cholecystectomy, appendectomy, hernia repair).
- Contraindications:
- Absolute: Hemodynamic instability, uncorrected coagulopathy, generalized peritonitis with septic shock, extensive bowel distension.
- Relative: Multiple prior surgeries, severe cardiopulmonary disease, advanced pregnancy, morbid obesity.
- Patient Preparation: Informed consent, NPO 6-8 hrs, general anaesthesia (GA) with endotracheal intubation, bladder catheterization, nasogastric tube (selective), DVT prophylaxis.
- Anatomy (Layers for Port Entry): Skin → Subcutaneous tissue (Camper's, Scarpa's fascia) → Anterior rectus sheath / External oblique aponeurosis → Rectus abdominis muscle / Internal oblique muscle → Transversus abdominis muscle → Fascia transversalis → Preperitoneal fat → Peritoneum.

⭐ The umbilicus is the most common site for primary port placement due to its natural scar, thinnest abdominal wall, and central access.
Pneumoperitoneum Creation - The Insufflation Game
⭐ CO2 is standard: high diffusibility, rapid absorption, non-combustible, minimizing gas embolism risk vs air.
- Gas: Carbon Dioxide (CO2)
- 📌 Properties (CARD): Cheap, Absorbed (rapidly, less acidosis), Rapidly diffused, Doesn't support combustion.
- Flow rate: Initial low flow 1 L/min, then high flow >5 L/min once intraperitoneal.
- Insufflation Pressures:
- Adults: Maintain 12-15 mmHg. Max 20 mmHg briefly for trocar.
- Children/Pregnancy: Lower (8-12 mmHg), monitor closely.
- Veress Needle Technique: (Closed access technique)
- Insertion Points:
- Umbilicus: Commonest.
- Palmer's Point: LUQ (3 cm below left costal margin, MCL), for prior surgery/obesity.
- Angle: 45° towards pelvis (thin) to 90° (obese).
- Placement Confirmation:
- Double click sound (fascia, peritoneum).
- Aspiration test (no blood/bile/gut contents).
- Saline drop / Hanging drop test (confirms negative pressure).
- Initial insufflation pressure $P_{initial} < \mathbf{8-10}\text{ mmHg}$.
- Insertion Points:
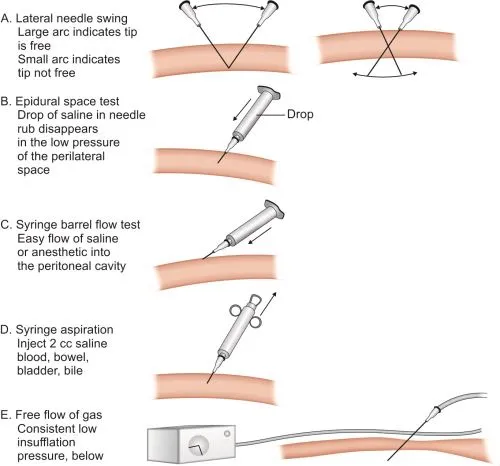
- Troubleshooting Insufflation:
Laparoscopic Entry Techniques - Gateway Tactics
Primary abdominal access is critical. Choice depends on patient factors and surgeon preference.
| Feature | Veress Needle (Closed) | Hasson Technique (Open) | Optical Trocar (Direct Vision) |
|---|---|---|---|
| Mechanism | Blind spring-loaded needle, then trocar | Mini-laparotomy, blunt trocar, stay sutures | Trocar with camera, visualised entry |
| Advantages | Rapid (experts), minimal scar | Safest (adhesions), controlled entry | Direct visualisation, ↓ blind injury |
| Disadv. | ↑ Blind visceral/vascular injury risk | Slower, larger incision, CO2 leak possible | Skill-dependent, vision obscured |
| Indications | Virgin abdomen, experienced surgeon | Prior surgery, adhesions, obesity, pregnancy | Most cases, preferred by many |
⭐ Hasson (open) technique is generally considered the safest method in patients with previous abdominal surgeries or suspected adhesions to avoid bowel/vascular injury.
Port Strategy & Complications - Safe Passage
- Ergonomics: Aim for "baseball diamond" or "instrument triangulation". Optimal working distance: 15-20 cm; angle between instruments: 60-90°.
- Secondary Ports:
- Site specific to procedure (e.g., cholecystectomy, appendectomy).
- Avoid epigastric vessels (💡 transilluminate!), rectus muscle.
- Direct visualization during insertion.

- Complications:
- Key risks: Vascular (epigastric, major vessels), bowel (↑ risk with adhesions), solid organ injury.
- Port-site issues: Bleeding, infection, hernia (close fascia for ports > 10mm, esp. midline).
- Gas-related: Surgical emphysema, gas embolism (⚠️ rare, potentially fatal).
- Safe Practices:
- Z-track insertion for bladeless trocars.

- Confirm hemostasis at port sites on removal.
- Z-track insertion for bladeless trocars.
⭐ Injury to major retroperitoneal vessels (aorta, IVC, iliacs) is the most feared and potentially lethal access complication, though rare.
High‑Yield Points - ⚡ Biggest Takeaways
- Veress needle: commonest at umbilicus; Palmer's point (LUQ) for adhesions. Confirm entry with low initial pressure (<8 mmHg).
- Open (Hasson) technique: safest for previous abdominal surgery; direct cut-down.
- Optical trocars: allow visualized entry, reducing blind injury risk.
- Pneumoperitoneum: CO2 insufflation; maintain pressure at 12-15 mmHg.
- Key complications: major vascular injury (aorta, IVC), bowel perforation, gas embolism.
- Direct trocar insertion (DTI): rapid access, but requires experience; higher risk of injury an undilated abdomen_.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

