PHPT Basics - Gland Overdrive
Primary Hyperparathyroidism (PHPT): Autonomous ↑PTH secretion causing hypercalcemia. Common in postmenopausal women.
- Etiology: Most commonly:
- Solitary Adenoma (80-85%)
- Glandular Hyperplasia (10-15%)
- Parathyroid Carcinoma (<1%)
- Associations: MEN 1 (📌 3Ps: Parathyroid, Pituitary, Pancreas), MEN 2A.
- PTH Action: ↑Bone resorption (↑Ca²⁺, ↑PO₄³⁻). Kidney: ↑Ca²⁺ reabsorption, ↓PO₄³⁻ reabsorption, ↑Vit D activation. Intestine (via Vit D): ↑Ca²⁺ absorption.

⭐ Most common cause of PHPT is a single parathyroid adenoma (80-85%).
Clinical Picture - Symptom Symphony
- Many patients are asymptomatic (discovered on routine labs).
- Symptomatic presentation: 📌 "Bones, stones, abdominal groans, and psychic moans."
- Skeletal: Osteitis fibrosa cystica (brown tumors), bone pain, fractures, subperiosteal resorption.

- Renal: Nephrolithiasis (calcium oxalate), nephrocalcinosis, polyuria.
- GI: Constipation, peptic ulcer disease (PUD), pancreatitis, nausea.
- Neuromuscular/Psychiatric: Fatigue, weakness, depression, confusion, memory loss.
- Cardiovascular: Hypertension (HTN), arrhythmias, short QT interval.
- Skeletal: Osteitis fibrosa cystica (brown tumors), bone pain, fractures, subperiosteal resorption.
⭐ Nephrolithiasis (calcium oxalate stones) is the most common symptomatic manifestation of PHPT (Primary Hyperparathyroidism).
Diagnostic Drilldown - Lab & Localize
Biochemical Profile (PHPT):
- ↑ Serum Ca (total & ionized), ↑ PTH (inappropriately normal/high)
- ↓ Serum PO4, ↑ ALP
- Assess Vitamin D (replete if deficient)
Key Differentiators:
| Condition | Serum Ca | Serum PTH | Key Feature |
|---|---|---|---|
| PHPT | ↑ | ↑ / Inapp. N | ↑ Urine Ca, Cl/PO4 ratio > 33 |
| FHH | ↑ (mild) | N / Mild ↑ | ↓ Urine Ca (Ca/CrCl ratio < 0.01) |
| Secondary HPT | ↓ / N | ↑↑ | Cause: CKD, Vit D def. |
| Tertiary HPT | ↑ | ↑↑↑ (autonomous) | Hx of prolonged Secondary HPT |
- USG neck (initial), Sestamibi scan (99mTc-MIBI)
- SPECT/CT (Sestamibi + CT), 4D-CT, MRI (complex/recurrent)
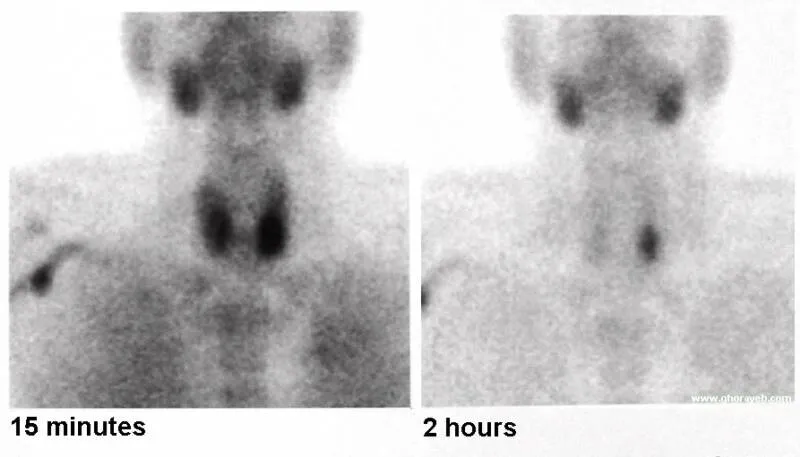
⭐ A Sestamibi scan combined with SPECT/CT is highly effective for pre-operative localization of solitary parathyroid adenomas.
Treatment Tactics - Surgical Solutions
- Surgical Indications (NIH 2022):
- Age <50
- Serum Ca >1 mg/dL above ULN
- CrCl <60 mL/min
- T-score ≤ -2.5 SD or vertebral fracture
- Nephrolithiasis/calcinosis
- Medical Management (Non-surgical):
- Cinacalcet, bisphosphonates
- Fluids, Vit D repletion (if deficient)
- Surgical Options:
- Minimally Invasive Parathyroidectomy (MIP) / Focused (if localized)
- Bilateral Neck Exploration (BNE)
- Intraoperative PTH (IOPTH):
- Miami criterion: >50% ↓ from baseline AND into normal range in 10-15 min post-excision.
⭐ Successful parathyroidectomy is confirmed by intraoperative PTH (IOPTH) monitoring, with a >50% drop from pre-excision baseline (Miami criterion) indicating cure.
Aftermath & Alerts - Post-Op Pointers
- Post-Op Complications:
- Hypocalcemia:
- Transient (common) vs. Permanent hypoparathyroidism.
- Hungry Bone Syndrome (HBS): severe ↓$Ca^{2+}$, ↓$PO_4^{3-}$, ↓$Mg^{2+}$.
- Recurrent Laryngeal Nerve (RLN) injury: hoarseness.
- Neck Hematoma (⚠️ airway risk!), Infection.
- Hypocalcemia:
- Hypocalcemia Management:
- Oral/IV Calcium, Vitamin D (Calcitriol).
- Follow-up: Serial serum $Ca^{2+}$ monitoring.
⭐ Hungry Bone Syndrome, characterized by severe and prolonged hypocalcemia, hypophosphatemia, and hypomagnesemia, can occur post-parathyroidectomy in patients with pre-existing severe bone disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Solitary parathyroid adenoma is the most common cause (~85%).
- Hallmark: Hypercalcemia (↑Ca²⁺) with inappropriately elevated PTH.
- Symptoms: "Stones, bones, groans, moans"; nephrolithiasis is most common. Many are asymptomatic.
- Bone disease: Osteitis fibrosa cystica (brown tumors) is classic but rare.
- Localization: Sestamibi scan and neck ultrasound are key pre-op.
- Treatment: Surgical parathyroidectomy is curative for symptomatic patients.
- Intraoperative PTH monitoring (drop >50%) confirms successful resection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


