Definition & Epidemiology - Oops Poops Happen
- Fecal Incontinence (FI): Involuntary passage of fecal material.
- Types:
- Urge FI: Strong urge, can't reach toilet.
- Passive FI: Unaware of stool passage.
- Soiling: Leakage, often with flatus/activity.
- Prevalence:
- General population: ~2-7%.
- Elderly (>65 yrs): ↑ up to 25%.
- Post-partum: ~5-25%.
⭐ Obstetric anal sphincter injuries (OASIS) are a leading cause of FI in parous women.
Anatomy & Physiology - Gatekeeper Control
- Internal Anal Sphincter (IAS): Smooth muscle, involuntary. Maintains ~80-85% of resting anal pressure.
- External Anal Sphincter (EAS): Striated muscle, voluntary. Provides conscious squeeze pressure; fatigues.
- Puborealis Muscle: Striated (levator ani). Forms sling, creates anorectal angle.
- Anorectal Angle: Acute angle (~80-100°) between rectum/anus. Key for flap-valve continence.
- Rectal Compliance: Rectum's viscoelastic ability to distend, allowing stool storage.
- Pudendal Nerve (S2-S4): Somatic nerve. Innervates EAS, puborectalis; crucial for voluntary control. 📌 "S2, S3, S4 keeps the poop off the floor."
⭐ The IAS contributes the majority (~80-85%) of resting anal tone, essential for passive continence; EAS allows voluntary squeeze.
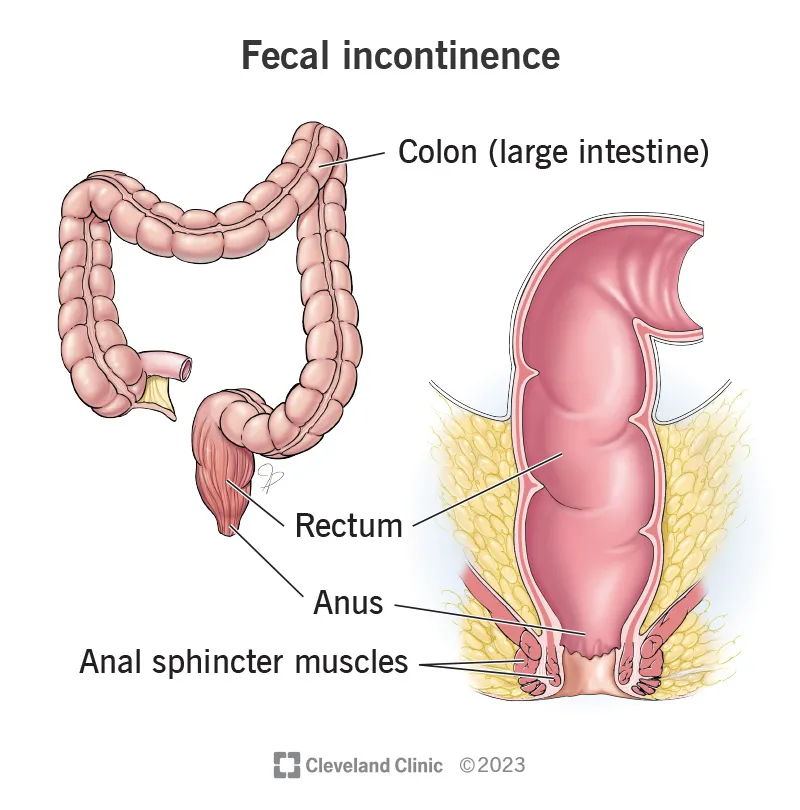 Caption: Anatomy of the anal canal and pelvic floor muscles involved in continence.
Caption: Anatomy of the anal canal and pelvic floor muscles involved in continence.
Etiology & Risk Factors - Why Leaks Occur
- Sphincter Weakness/Damage:
- Obstetric trauma (OASIS - Obstetric Anal Sphincter Injuries)
⭐ Obstetric trauma is the most common cause of major fecal incontinence in women.
- Iatrogenic: anorectal surgery (e.g., fistula, hemorrhoidectomy)
- Anorectal malformations
- Aging
- Obstetric trauma (OASIS - Obstetric Anal Sphincter Injuries)
- Neurological Disorders (Neuropathy):
- Diabetes mellitus (autonomic neuropathy)
- Multiple Sclerosis (MS)
- Spinal cord injury
- Pudendal nerve damage (childbirth, chronic straining)
- Loss of Storage Capacity/Compliance:
- Inflammatory Bowel Disease (IBD - Crohn's, Ulcerative Colitis)
- Pelvic radiation (proctitis)
- Altered Stool Consistency/Overflow:
- Chronic diarrhea (e.g., infective, malabsorption)
- Fecal impaction with overflow
Clinical Assessment & Investigations - Diagnosis Detective
- History: Onset, type (urge/passive), frequency, severity. Obstetric (tears, instrumental) & surgical Hx.
- Scoring: St. Mark’s (Vaizey) score / Wexner score (CCIS) to quantify severity.
- Physical Exam:
- Perianal: skin changes, fistula, prolapse, scars.
- DRE: resting tone, squeeze pressure, anocutaneous reflex.
- Initial Scope: Proctoscopy/Sigmoidoscopy (rule out local pathology).
- Key Investigations:
- Endoanal Ultrasound (EAUS): sphincter integrity.
- Anorectal Manometry: pressures, rectal sensation, reflexes.
- EMG/Pudendal Nerve Terminal Motor Latency (PNTML): neuropathy.
⭐ > Endoanal ultrasound (EAUS) is the gold standard for imaging anal sphincter integrity.
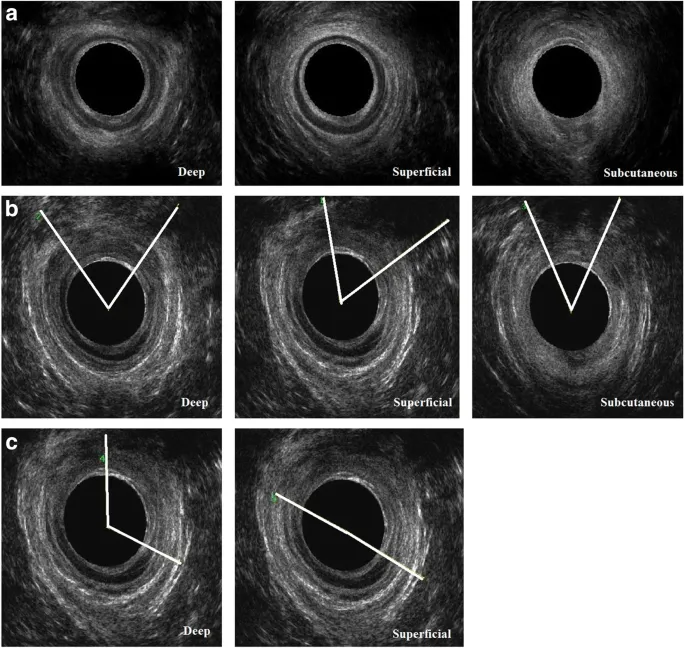 Caption: Endoanal ultrasound showing sphincter defect OR table for Wexner/St. Mark's score.
Caption: Endoanal ultrasound showing sphincter defect OR table for Wexner/St. Mark's score.
Management - Plugging The Leaks
- Conservative First!
- Diet: ↑Fiber, ↑fluids.
- Pelvic Floor Muscle Training (PFMT/Kegel) ± Biofeedback.
- Antidiarrheals: Loperamide (max 16mg/day), Diphenoxylate.
- Medical Adjuncts:
- Bulking agents (Psyllium, Methylcellulose).
- Amitriptyline (low dose for urgency/IBS-D).
- Surgical Options:
| Option | Key Indication(s) | Brief Note |
|---|---|---|
| Sphincteroplasty | EAS defect (e.g., obstetric trauma) | Direct anatomical repair |
| SNS | Intact sphincter or minor defect, neurogenic FI | Neuromodulation |
| Injectable Agents | IAS dysfunction, augment sphincter | Minimally invasive |
| PTNS | Neuromodulation option | Office-based, less invasive than SNS |
| ABS | Severe, refractory FI | Mechanical sphincter |
| Colostomy | Intractable FI, palliative care | Fecal diversion, last resort |
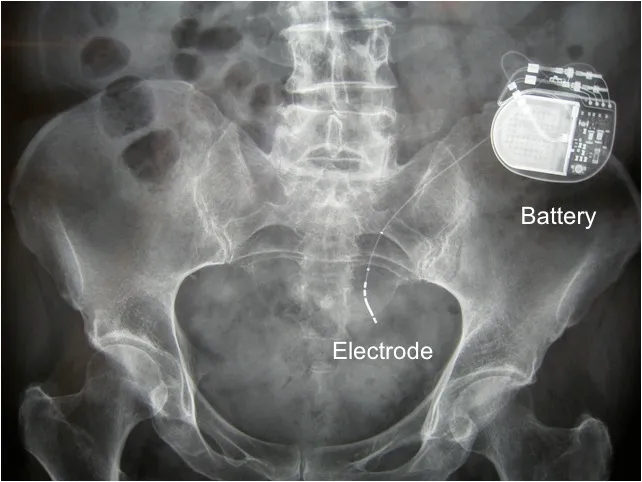 Caption: Sacral nerve stimulator (SNS) device.
Caption: Sacral nerve stimulator (SNS) device.
High‑Yield Points - ⚡ Biggest Takeaways
- Fecal incontinence (FI) is the involuntary passage of fecal material.
- Obstetric injury to the anal sphincter or pudendal nerve is a primary cause.
- Anorectal manometry assesses sphincter pressures; endoanal ultrasound (EAUS) visualizes sphincter defects.
- Conservative therapy: High-fiber diet, antidiarrheals (loperamide), biofeedback, pelvic floor exercises.
- Sphincteroplasty is for anterior sphincter defects; Sacral Nerve Stimulation (SNS) for neurogenic/idiopathic FI.
- Permanent colostomy is a last resort for intractable FI_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

