Venous Access & Imaging - Gateway Guidance
- Preferred Access Sites:
- Internal Jugular Vein (IJV): Right IJV preferred (straighter course to SVC).
- Femoral Vein: Higher risk of DVT/infection.
- Subclavian Vein: Higher risk of pneumothorax.
- Basilic/Cephalic Veins (PICC lines).
- Techniques:
- Seldinger technique: Needle → guidewire → dilator → catheter.
- Ultrasound guidance: Standard of care for IJV access; improves success, ↓ complications.
- Needle visible as hyperechoic line.
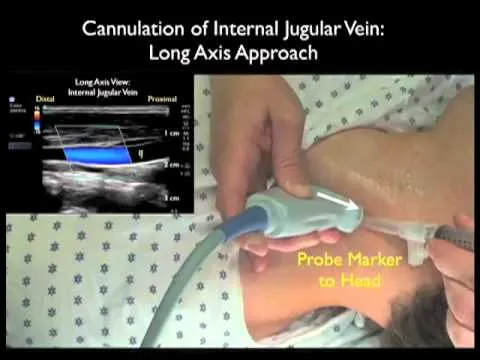
- Needle visible as hyperechoic line.
- Imaging Modalities:
- Duplex Ultrasound: Initial assessment; thrombus detection, vessel patency & diameter.
- Contrast Venography: Gold standard for detailed venous anatomy, stenosis, occlusion.
- Digital Subtraction Angiography (DSA) commonly used.
⭐ The most common non-infectious complication of central venous catheterization is catheter-related thrombosis.
- Pre-procedure: Coagulation profile (INR < 1.5, Platelets > 50,000/μL).
IVC Filters & Thrombolysis - Clot Busters
-
IVC Filters: Prevent Pulmonary Embolism (PE) from Deep Vein Thrombosis (DVT).
- Indications: Anticoagulation (AC) contraindication/complication/failure; High-risk prophylaxis (e.g., major trauma, surgery); Large free-floating iliofemoral thrombus.
- Types: Permanent; Retrievable (preferred for transient risk, aim retrieval 29-54 days post-implantation).
- Placement: Typically infrarenal; Suprarenal for specific cases (e.g., renal vein thrombus, pregnancy).
- Complications: Access site issues, filter migration/fracture, IVC thrombosis, caval perforation.
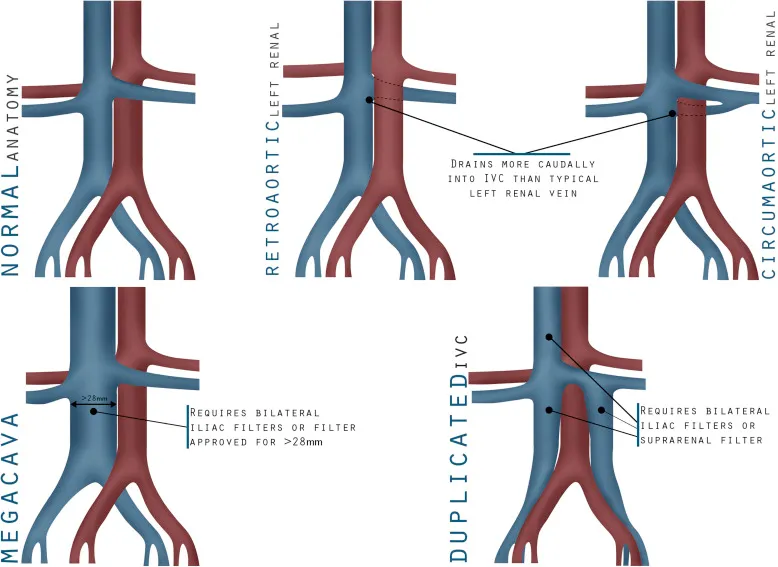
-
Thrombolysis (Catheter-Directed - CDT): Rapid clot dissolution in severe DVT/PE.
- Agents: Alteplase (tPA), Urokinase.
- Indications: Massive PE with hemodynamic instability; Extensive DVT (e.g., iliofemoral) with severe symptoms or limb threat.
- Key Contraindications: Active bleeding; recent Cerebrovascular Accident (CVA) (<3 months); major surgery/trauma (<3 weeks); uncontrolled Hypertension (HTN) (>185/110 mmHg).
- Complications: Bleeding (major risk, esp. intracranial), hematoma, allergic reaction.
⭐ For retrievable IVC filters, the FDA recommends evaluation for removal between 29 and 54 days after implantation, once the risk of PE has passed, to reduce long-term filter-related complications like thrombosis or fracture.
Portal Hypertension Solutions - Pressure Plungers
-
Core Aim: Alleviate high portal pressure ($P_{portal}$) & its sequelae (e.g., variceal bleeds, refractory ascites).
-
TIPS (Transjugular Intrahepatic Portosystemic Shunt): Key "pressure plunger".
- Mechanism: Creates a direct, low-resistance channel using a stent between the intrahepatic portal vein and a hepatic vein.
- Access: Transjugular (via internal jugular vein).
- Primary Indications:
- Refractory/recurrent variceal hemorrhage.
- Refractory ascites or hepatic hydrothorax.
- Therapeutic Goal: Achieve portosystemic gradient (PSG) < 12 mmHg.
⭐ A post-TIPS PSG < 12 mmHg is crucial for preventing variceal rebleeding.
- Major Complications: Hepatic encephalopathy (HE) (up to 30%), shunt dysfunction (stenosis/occlusion).
- Key Contraindications: Severe right heart failure, severe pulmonary hypertension (mPAP > 45 mmHg), active uncontrolled infection.
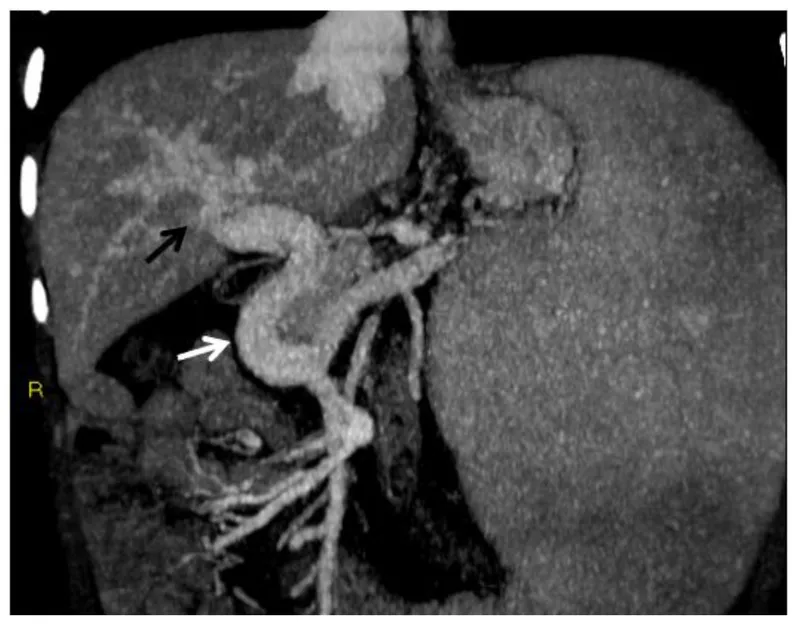
-
Procedural Overview & Pressure Dynamics
Dialysis Access & Misc - Flow Fixers
- Dialysis Access:
- AV Fistula (AVF): Preferred. Brescia-Cimino (radiocephalic). Maturation: 6-8 wks. 📌 Rule of 6s: Flow >600mL/min, Diameter >6mm, Depth <6mm.
- AV Graft (AVG): PTFE. Use if veins poor. Higher complications (stenosis, infection).
- Complications: Stenosis (juxta-anastomotic in AVF; venous outflow in AVG), thrombosis, steal syndrome.
- Intervention: Angioplasty (PTA), stenting, thrombectomy.
- SVC Syndrome: Obstruction (malignancy, catheter). Facial/arm swelling, dyspnea. Rx: Stenting, thrombolysis.
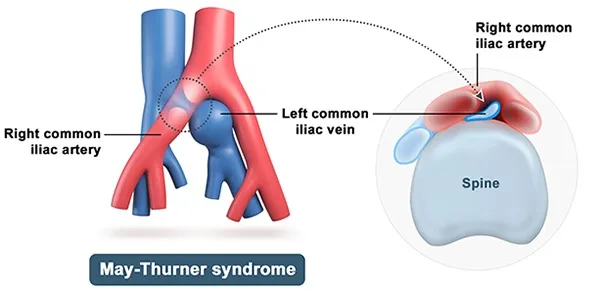
- May-Thurner Syndrome: Lt Common Iliac Vein (CIV) compression by Rt Common Iliac Artery (CIA). Lt leg DVT/swelling. Rx: Stenting.
- Nutcracker Syndrome: Lt Renal Vein (RV) compression (SMA/Aorta). Hematuria, flank pain. Rx: Stenting.
⭐ The most common site of stenosis in an AV fistula is at the venous anastomosis or immediate downstream vein (juxta-anastomotic).
High‑Yield Points - ⚡ Biggest Takeaways
- IVC filters are crucial for DVT/PE when anticoagulation is contraindicated or fails.
- Catheter-directed thrombolysis (CDT) is vital for massive PE and extensive DVT like iliofemoral.
- TIPS creation manages refractory variceal bleeding and ascites due to portal hypertension.
- Major TIPS complications include hepatic encephalopathy and shunt stenosis/occlusion.
- EVLA/RFA are first-line treatments for symptomatic superficial venous reflux (varicose veins).
- Adrenal venous sampling is gold standard to localize aldosterone-producing adenomas in Conn's syndrome (primary hyperaldosteronism).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

