Breathing-Related Sleep Disorders - Night's Silent Struggle
- Disorders characterized by abnormal respiration during sleep.
- Types:
- Obstructive Sleep Apnea (OSA): Most common.
- Central Sleep Apnea (CSA).
- Sleep-Related Hypoventilation Disorders.
- Sleep-Related Hypoxemia Disorder.
- Obstructive Sleep Apnea (OSA):
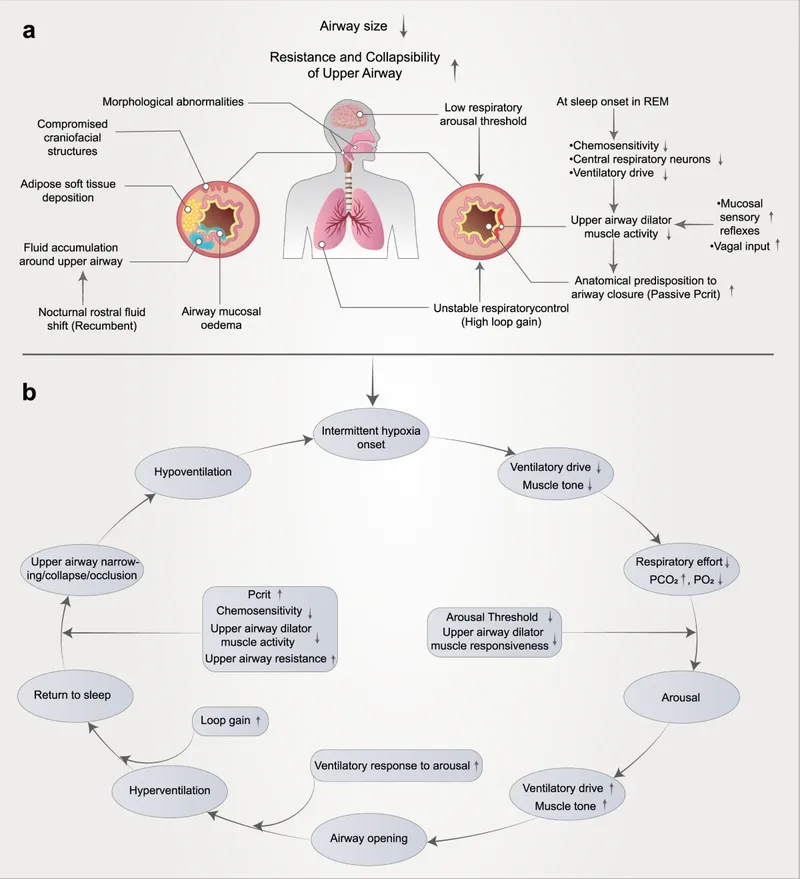
- Pathophysiology: Recurrent episodes of partial/complete upper airway obstruction during sleep → intermittent hypoxia, hypercapnia, sleep fragmentation.
- Risk factors: Obesity (BMI >30 kg/m²), male, age, craniofacial abnormalities, smoking.
- Symptoms: Loud snoring, witnessed apneas, daytime sleepiness.
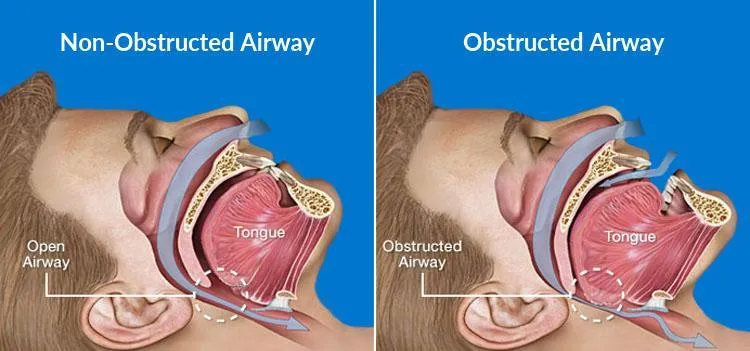
⭐ OSA is a major risk factor for hypertension, cardiovascular disease, and stroke. Apnea-Hypopnea Index (AHI) >5 events/hour is diagnostic; >15 moderate; >30 severe.
Breathing-Related Sleep Disorders - Diagnosis & Drama
-
Clinical Drama (Symptoms):
- Loud habitual snoring, choking/gasping episodes during sleep.
- Witnessed apneas reported by bed partner.
- Excessive Daytime Sleepiness (EDS); assess with Epworth Sleepiness Scale (ESS >10 is significant).
- Morning headaches, non-restorative sleep, fatigue, impaired concentration.
- 📌 Mnemonic STOP-BANG for OSA screening: Snoring, Tiredness, Observed apnea, high blood Pressure, BMI >35 kg/m², Age >50 yrs, Neck circumference >40cm, Gender male.
-
Diagnostic Evaluation:
- Polysomnography (PSG): Gold standard diagnostic test.
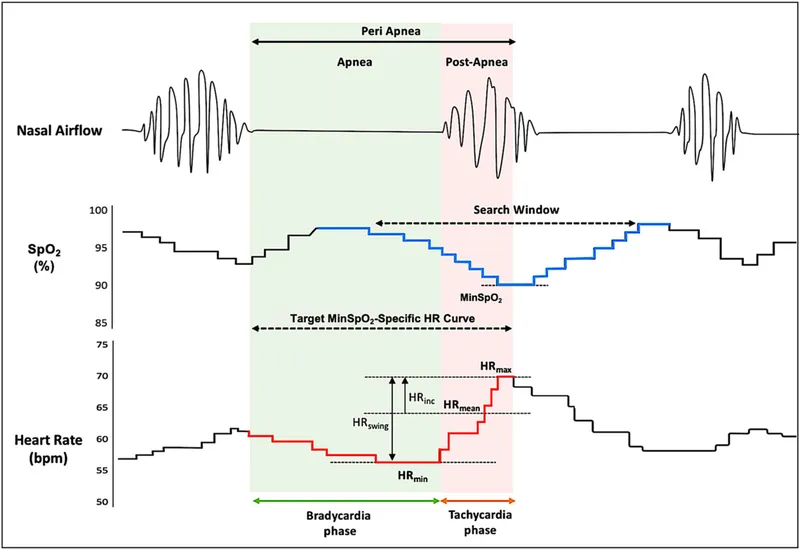
- Records: EEG (sleep staging), EOG (eye movements), EMG (muscle tone), ECG, airflow (nasal/oral), respiratory effort (chest/abdomen), SaO2 (pulse oximetry).
- Key parameter: Apnea-Hypopnea Index (AHI) = (Total apneas + hypopneas) / Total sleep time in hours.
- Apnea: Cessation of airflow ≥10 seconds.
- Hypopnea: Reduction in airflow ≥30% for ≥10 seconds associated with ≥3% oxygen desaturation or an arousal.
- AHI Severity for OSA (Adults):
- Mild: AHI 5-14 events/hour.
- Moderate: AHI 15-29 events/hour.
- Severe: AHI ≥30 events/hour.
- Polysomnography (PSG): Gold standard diagnostic test.
⭐ Untreated Obstructive Sleep Apnea (OSA) is a significant independent risk factor for systemic hypertension, cardiovascular disease (e.g., CAD, arrhythmias, heart failure), stroke, and type 2 diabetes mellitus.
Breathing-Related Sleep Disorders - Conquering the Collapse
- Goal: Prevent pharyngeal collapse, normalize breathing.
- Lifestyle: Weight loss, avoid alcohol/sedatives, positional therapy.
- CPAP (Pneumatic Splint):
- 1st line for Mod-Severe OSA (AHI ≥ 15).
- Maintains airway patency. Adherence vital.
- Alternatives:
- Oral Appliances (MADs): Mild-Mod OSA, CPAP intolerance.
- Surgery (UPPP, MMA): Anatomical issues. Tracheostomy (last resort).
- Risks (Untreated): HTN, arrhythmia, CVA, daytime somnolence.
⭐ CPAP adherence significantly reduces cardiovascular morbidity in OSA patients.
Breathing-Related Sleep Disorders - Brain's Breathing Blues
- Obstructive Sleep Apnea (OSA): Upper airway collapse.
- Symptoms: Snoring, daytime sleepiness, apneas. 📌 STOP-BANG risk.
- Dx: Polysomnography (PSG) AHI ≥ 15 or ≥ 5 + symptoms.
- Rx: CPAP, weight loss.
- Central Sleep Apnea (CSA): ↓/Absent ventilatory effort.
- Types: Idiopathic, Cheyne-Stokes (HF, stroke), opioid-induced.
- Dx: PSG shows central apneas.
- Rx: Treat cause, ASV, BiPAP.
- Sleep-Related Hypoventilation: ↑PaCO2 in sleep.
- Causes: Obesity Hypoventilation Syndrome (OHS), neuromuscular disease.
- Dx: PSG: sustained ↑PaCO2 (> 55 mmHg).
- Rx: NIV (BiPAP), treat cause.
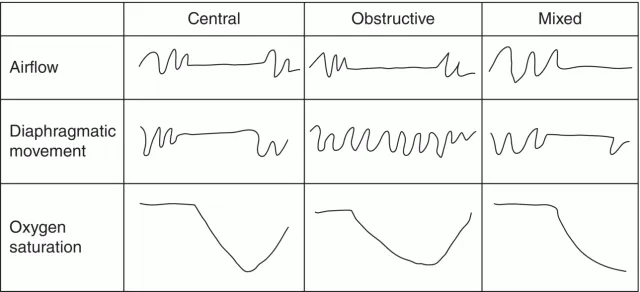
⭐ Cheyne-Stokes respiration, a pattern of CSA, is frequently seen in patients with congestive heart failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Obstructive Sleep Apnea (OSA): most common, due to recurrent upper airway collapse during sleep.
- Major OSA risk factors: obesity (↑BMI), male gender, older age, large neck circumference.
- Polysomnography (PSG) is the diagnostic gold standard; measures Apnea-Hypopnea Index (AHI).
- AHI >5 events/hour confirms diagnosis; CPAP is first-line for moderate-severe OSA (AHI ≥15).
- Central Sleep Apnea (CSA): cessation of airflow due to absent/reduced respiratory effort.
- Obesity Hypoventilation Syndrome (OHS): triad of obesity, daytime hypercapnia, and sleep-disordered breathing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

