Foundations - Guiding Principles Pronto
- Purpose: Standardize care, ensure Evidence-Based Medicine (EBM), improve patient outcomes, provide medico-legal support.
- Key Sources: Indian Psychiatric Society (IPS), NICE, APA.
- Core Tenets:
- Diagnosis precedes treatment.
- Shared decision-making with patient.
- Titration: "Start low, go slow."
- Adequate trial: Minimum 4-6 weeks at therapeutic dose.
- Prefer monotherapy; minimize polypharmacy.
- Regularly monitor efficacy and Adverse Drug Reactions (ADRs).
- Employ Measurement-Based Care (MBC).
- Consider patient factors: age, pregnancy, comorbidities.
⭐ IPS guidelines are tailored for Indian population & resource settings, making them highly relevant for NEET PG.
Schizophrenia - Psychosis Pathway Pointers
- Initial Phase: Second-Generation Antipsychotics (SGAs) e.g., risperidone, olanzapine, aripiprazole, are first-line. Aim for 4-6 weeks trial.
- Non-response: Switch to another SGA or a First-Generation Antipsychotic (FGA).
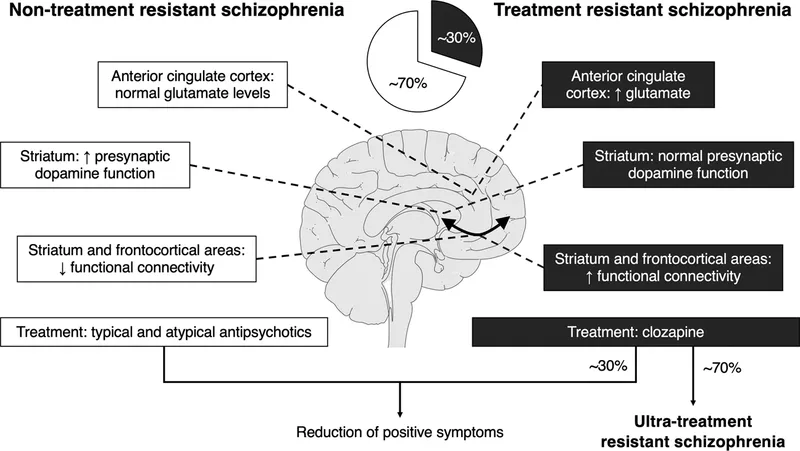
- Treatment-Resistant Schizophrenia (TRS): Defined by failure of ≥2 antipsychotics (adequate dose/duration).
- Clozapine is the drug of choice.
- Requires strict Absolute Neutrophil Count (ANC) monitoring: weekly for first 18 weeks, then fortnightly up to 1 year, then monthly. 📌 ANC: "Always Needs Checking".
- Adherence: Long-Acting Injectables (LAIs) are crucial for poor adherence.
- Augmentation: Electroconvulsive Therapy (ECT), psychosocial support.
⭐ Clozapine is the only FDA-approved medication for reducing suicide risk in schizophrenic patients.
Mood Disorders - Mood Maze Maps
-
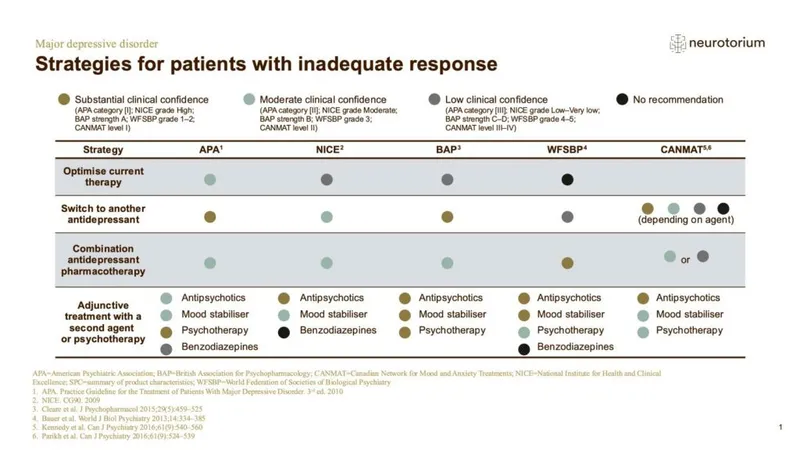
MDD: Stepwise Approach
- First-line: SSRIs/SNRIs (e.g., Escitalopram, Venlafaxine).
- Adequate trial: 4-8 weeks at therapeutic dose.
- Non/Partial Response:
- Switch SSRI/SNRI or class.
- Augment: Bupropion, Mirtazapine, AAPs (e.g., Aripiprazole), Lithium.
- TRD:
- ECT - most effective.
- Ketamine/Esketamine.
- VNS, TMS.
- First-line: SSRIs/SNRIs (e.g., Escitalopram, Venlafaxine).
-
Bipolar Disorder: Phase-Specific Tx
- Mania/Hypomania:
- Mood Stabilizers: Li (target: 0.6-1.2 $mEq/L$), Valproate, CBZ.
- AAPs: Olanzapine, Risperidone, Quetiapine.
- ⚠️ Avoid antidepressant (AD) monotherapy (risk of switch).
- Bipolar Depression:
- Mood Stabilizers: Lamotrigine (slow up), Li.
- AAPs: Quetiapine, Lurasidone, Olanzapine-Fluoxetine Combination (OFC).
- Maintenance:
- Mood stabilizers (Li, Valproate, Lamotrigine).
⭐ Lithium is gold standard for long-term prophylaxis in bipolar disorder, reducing suicide risk.
- Mania/Hypomania:
Anxiety/OCD - Jittery Journey Guides
- First-line: SSRIs (e.g., Escitalopram, Fluvoxamine for OCD). Start low, go slow. Titrate to effective dose. Adequate trial: 8-12 weeks.
- Second-line: Switch SSRI, SNRI (e.g., Venlafaxine), or Clomipramine (TCA - esp. for OCD, up to 250 mg/day).
- Augmentation: Antipsychotics (e.g., low-dose Risperidone for OCD), Buspirone (GAD).
- Adjuncts: Benzodiazepines (short-term, ⚠️ dependence). CBT (ERP for OCD) crucial.
⭐ Higher doses of SSRIs are generally required for OCD (e.g., Fluoxetine up to 80 mg/day) compared to depression.
High‑Yield Points - ⚡ Biggest Takeaways
- SSRIs are first-line for Major Depressive Disorder (MDD); TCAs/MAOIs are later choices.
- Acute mania (Bipolar) often needs mood stabilizers (Lithium, Valproate) +/- antipsychotics.
- Schizophrenia is treated with antipsychotics; clozapine is crucial for Treatment-Resistant Schizophrenia (TRS).
- Anxiety disorders (GAD, Panic) usually start with SSRIs/SNRIs; benzodiazepines for short-term use.
- ADHD first-line treatment involves stimulants like Methylphenidate.
- Adherence to NICE/IPS guidelines is critical for standardized care and optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

