Tourette's Syndrome: Definition & Epidemiology - Tic Talk Basics
- A neurodevelopmental disorder characterized by multiple motor tics AND one or more vocal (phonic) tics.
- Diagnostic criteria: Tics present for >1 year; onset before age 18.
- Peak tic severity often in early adolescence.
- Typical age of onset: 4-6 years.
- Prevalence: ~0.6-1% in school-aged children; higher in special education settings.
- Males affected more than females (M:F ratio ≈ 3-4:1).
- Common comorbidities: ADHD (most frequent), OCD.
⭐ Tics characteristically wax and wane in frequency, type, location, and severity over time; often improve in adulthood.
Tourette's Syndrome: Clinical Manifestations - The Tic Spectrum
- Core: Multiple motor tics AND ≥1 vocal tics present over time.
- Tic Features:
- Sudden, rapid, recurrent, non-rhythmic movements or vocalizations.
- Wax & wane in frequency/severity; premonitory sensory urge common.
- Temporarily suppressible; stress/fatigue worsen, concentration improves.
- Motor Tics:
- Simple: Eye blinking, head jerking, shoulder shrugging, grimacing.
- Complex: Gesturing, touching, jumping, copropraxia (obscene gestures), echopraxia.
- Vocal (Phonic) Tics:
- Simple: Throat clearing, sniffing, grunting, yelping, barking.
- Complex: Words, phrases; coprolalia (obscene words), echolalia, palilalia.
⭐ Coprolalia (involuntary swearing) is often highlighted but occurs in only about 10-15% of Tourette's Syndrome patients.
Tourette's Syndrome: Etiopathogenesis - Brain's Ticcing Clockwork
- Genetics: Strong genetic component; likely polygenic. High heritability (~77%).
- No single gene identified; multiple susceptibility genes (e.g., SLITRK1, HDC).
- Neurobiology: Primarily dysfunction in Cortico-Striato-Thalamo-Cortical (CSTC) circuits.
- Dopamine (DA) hyperactivity in striatum is a key theory.
- ↑ D2 receptor density.
- Possible roles for serotonin, norepinephrine, GABA, glutamate.
- Dopamine (DA) hyperactivity in striatum is a key theory.
- Environmental Factors: Perinatal insults, maternal smoking, psychosocial stress.
- PANDAS (Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections) - controversial link.
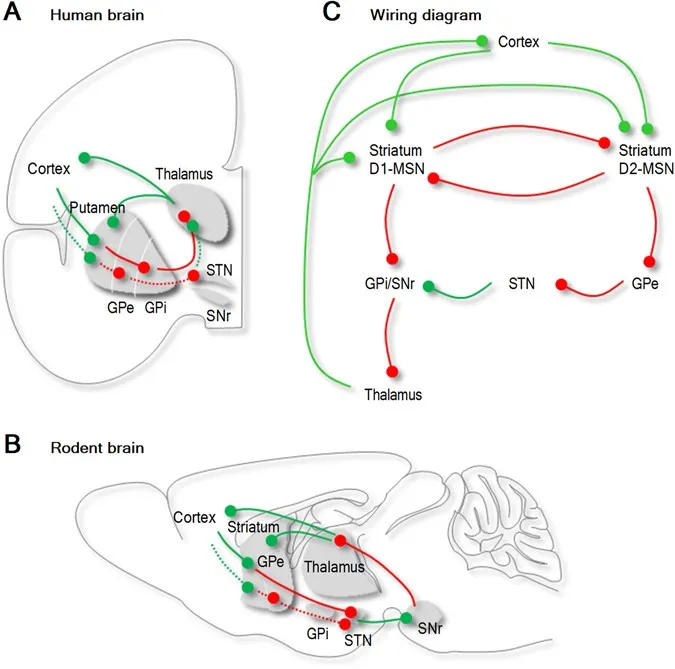 loop with dopamine pathways highlighted)
loop with dopamine pathways highlighted)
⭐ Basal ganglia, particularly the striatum (caudate and putamen), are central to tic generation due to dopaminergic dysregulation within the CSTC pathways. This is a frequent exam focus regarding Tourette's pathophysiology.
Tourette's Syndrome: Diagnosis & Differentials - Spotting the Tics
- Diagnosis (DSM-5):
- Multiple motor & ≥1 vocal tics (not always concurrent).
- Tics persist >1 year.
- Onset <18 years.
- Not due to substance/other medical cause.
- Differentials:
- Provisional Tic Disorder: Tics <1 year.
- Persistent Motor/Vocal Tic Disorder: >1 yr, motor OR vocal only.
- Movement disorders (dystonia, chorea), stereotypies, OCD.
⭐ Tics characteristically wax and wane in frequency, severity, type, and location over time.
Tourette's Syndrome: Management Strategies - Taming the Tics
- Goal: Symptom reduction, improved functioning. Not all tics require medication.
- First-line: Psychoeducation, supportive therapy, habit reversal training (HRT).
- Pharmacotherapy (for moderate-severe or impairing tics):
- Alpha-2 adrenergic agonists: Clonidine, Guanfacine (preferred initial agents, esp. with ADHD).
- Antipsychotics (Dopamine antagonists): Risperidone, Haloperidol, Pimozide (more effective for tics, but more side effects). Use lowest effective dose.
- Others: Topiramate, Tetrabenazine, Botulinum toxin injections (for focal tics).
⭐ Clonidine is often a first-line pharmacological choice, particularly if co-existing ADHD is present, due to its more favorable side-effect profile compared to antipsychotics.
High‑Yield Points - ⚡ Biggest Takeaways
- Tourette's Syndrome: Multiple motor AND ≥1 vocal tics for >1 year; onset <18 years.
- Most common comorbidities: ADHD (~60%) and OCD (~40%).
- Strong genetic link; involves basal ganglia dopaminergic hyperactivity.
- Treatment: Behavioral therapies (HRT, CBIT) first; then alpha-2 agonists (clonidine, guanfacine) or antipsychotics.
- Tics often peak in early adolescence, frequently improving in adulthood.
- Coprolalia (obscene vocalizations) is uncommon (~10-15%) and not required for diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

