GI Arterial Supply - Gut's Red Rivers
- Foregut (Celiac Trunk): Stomach, Spleen, Liver, Gallbladder, Pancreas, Duodenum (proximal).
- Branches: Left Gastric, Splenic, Common Hepatic.
- Midgut (Superior Mesenteric Artery - SMA): Duodenum (distal) to Transverse Colon (proximal 2/3).
- Branches: Inferior Pancreaticoduodenal, Jejunal, Ileal, Ileocolic, Right Colic, Middle Colic.
- 📌 Mnemonic (SMA): Inferior Pancreaticoduodenal, Jejunal, Ileal, Ileocolic, Right Colic, Middle Colic (I Just Inherited Riches Man!)
- Hindgut (Inferior Mesenteric Artery - IMA): Transverse Colon (distal 1/3) to Rectum (upper part).
- Branches: Left Colic, Sigmoid, Superior Rectal.
- Key Anastomoses:
- Pancreaticoduodenal Arcades (Celiac & SMA).
- Marginal Artery of Drummond (SMA & IMA).
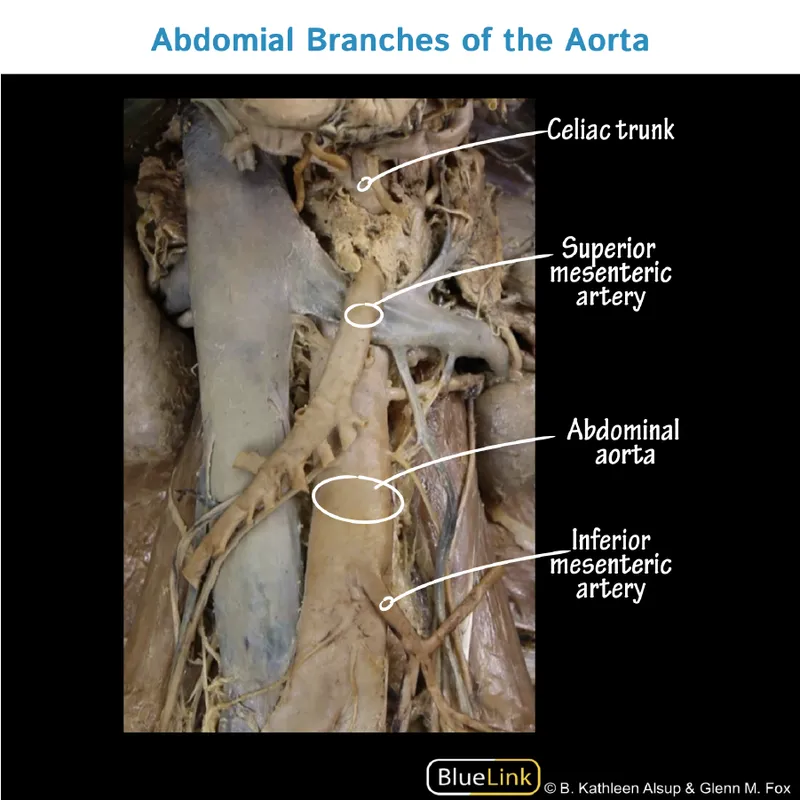
⭐ Watershed areas like Griffith's point (splenic flexure; SMA-IMA junction) and Sudeck's point (rectosigmoid junction; IMA-iliac artery junction) are vulnerable to ischemia.
GI Venous Drainage - Portal Powerhouse
- Portal Vein: SMV + Splenic Vein (SV).
- IMV often joins SV.
- Tributaries: SMV, SV, IMV, Gastric, Cystic, Paraumbilical v.
- Portosystemic Anastomoses (Portal HTN signs):
- Gastroesophageal: (L. Gastric ↔ Azygos) → Esophageal varices.
- Paraumbilical: (Paraumbilical ↔ Epigastric) → Caput medusae.
- Rectal: (Sup. Rectal ↔ Mid/Inf. Rectal) → Internal hemorrhoids.
- Retroperitoneal: (Splenic/Colic ↔ Renal/Lumbar) → Often silent.
📌 Mnemonic: "GURS" (Gastroesophageal, Umbilical, Rectal, Splenorenal/Retroperitoneal).
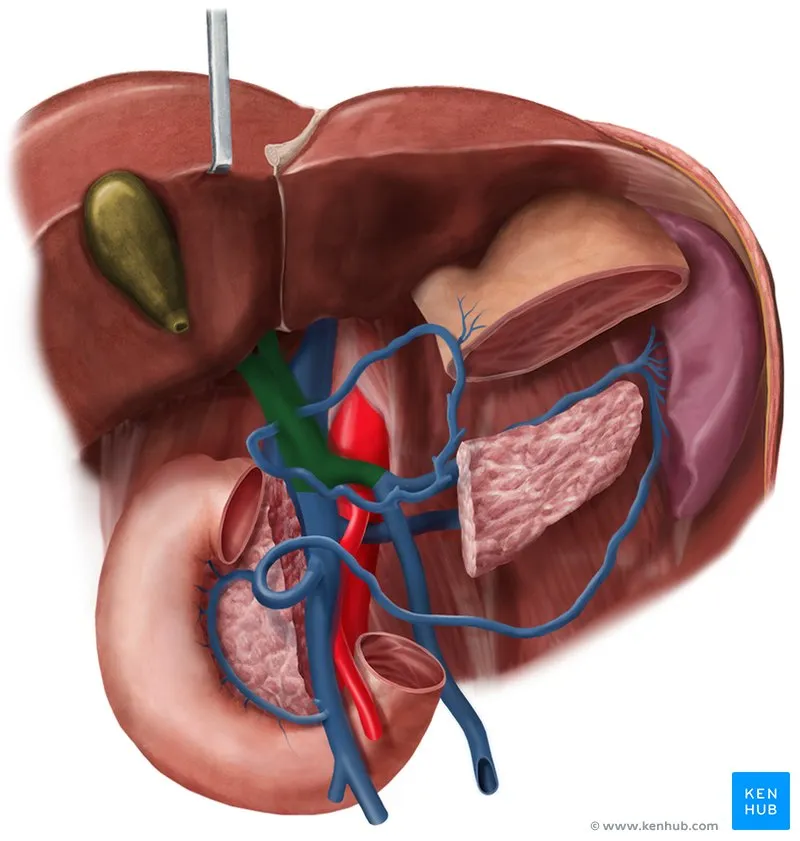
⭐ Esophageal varices, from portal hypertension and gastroesophageal shunting, are the most common cause of life-threatening upper GI bleeding in cirrhosis.
GI Blood Flow Regulation - Gut's Traffic Cops
- Nervous Control:
- Sympathetic: Primarily vasoconstriction via α-adrenergic receptors (↓ flow).
- Parasympathetic: Primarily vasodilation, often indirect (e.g., via enteric neurons or ↑ metabolic activity) (↑ flow).
- Hormonal/Paracrine Factors:
- Vasodilators: e.g., VIP, CCK, gastrin, secretin, bradykinin, prostaglandins E & I, histamine, adenosine (↑ flow).
- Vasoconstrictors: e.g., Angiotensin II, vasopressin, norepinephrine, endothelin (↓ flow).
- Local Metabolic Factors (Key for Functional Hyperemia):
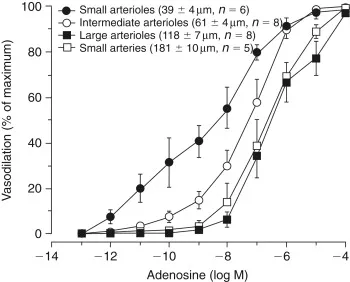
- ↓ $O_2$, ↑ $CO_2$, ↑ $H^+$ (↓ pH), ↑ adenosine, ↑ $K^+$, ↑ osmolarity - all lead to vasodilation (↑ flow).
- Autoregulation:
- Intrinsic ability to maintain constant blood flow despite changes in perfusion pressure (myogenic and metabolic mechanisms).
⭐ Adenosine is considered a principal mediator of postprandial (functional) hyperemia in the intestine, linking metabolic activity to increased blood flow.
Special GI Circulation Features - Gut's Unique Flow
- Postprandial (Functional) Hyperemia:
- Blood flow ↑ 2-8 fold for 2-4 hours post-meal.
- Mechanisms: Metabolic, hormonal (CCK, gastrin), neural (parasympathetic).
- Countercurrent Exchange in Villi:
- Arteriole-venule O₂ shunt before villus tip.
- Efficient absorption; villus tip hypoxia risk.
⭐ The countercurrent oxygen exchange mechanism in intestinal villi, while efficient for absorption, makes the villous tip the most vulnerable part of the mucosa to ischemic injury.
- Splanchnic Blood Reservoir:
- Gut/spleen veins store significant blood.
- Mobilized by sympathetic stimulation (stress: hemorrhage, exercise).
- Response to Ischemia & 'Autoregulatory Escape':
- Initial sympathetic vasoconstriction.
- 'Escape' via local vasodilator buildup (adenosine, K⁺, H⁺).
High‑Yield Points - ⚡ Biggest Takeaways
- Splanchnic circulation constitutes ~25% of cardiac output, with ↑ postprandial flow.
- Key arterial supply via celiac trunk, SMA, and IMA.
- Hepatic portal vein delivers nutrient-rich blood from gut to liver.
- Villus countercurrent exchange mechanism renders tips vulnerable to hypoxia.
- Sympathetic nerves cause vasoconstriction; parasympathetic activity generally ↑ blood flow.
- Functional hyperemia (postprandial) is mediated by metabolic factors and GI hormones like CCK_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

