Leukocyte Overview - The White Cell Wonders
- Mobile defense units; originate from hematopoietic stem cells in bone marrow.
- Total Leukocyte Count (TLC): 4,000-11,000/mm³.
- Main Categories:
- Granulocytes (cytoplasmic granules, lobed nuclei): Neutrophils (phagocytosis), Eosinophils (allergy, parasites), Basophils (histamine release).
- Agranulocytes (no prominent granules, round/kidney-shaped nuclei): Lymphocytes (specific immunity), Monocytes (phagocytosis, become macrophages).
- Differential Leukocyte Count (DLC) - % of total WBCs:
- Neutrophils: 40-75%
- Lymphocytes: 20-45%
- Monocytes: 2-10%
- Eosinophils: 1-6%
- Basophils: <1%
- 📌 Mnemonic (decreasing order of prevalence): Never Let Monkeys Eat Bananas.
⭐ Leukocytosis (↑WBC count, >11,000/mm³) often indicates infection or inflammation; Leukopenia (↓WBC count, <4,000/mm³) can suggest bone marrow suppression, severe infections, or autoimmune conditions.
Granulocytes - The First Responders
- Innate immunity; phagocytosis & inflammation.
- Cytoplasmic granules, multi-lobed nuclei.

1. Neutrophils (PMNs)
- Abundance: 40-75% WBCs.
- Nucleus: 3-5 lobes. Granules: Lysozyme, myeloperoxidase.
- Role: Bacterial/fungal phagocytosis; acute inflammation.
- Pus: Dead neutrophils.
⭐ Form Neutrophil Extracellular Traps (NETs) to ensnare pathogens.
2. Eosinophils
- Abundance: 1-6% WBCs.
- Nucleus: Bilobed. Granules: Major Basic Protein (MBP), histaminase.
- Role: Parasitic infections; allergic reactions (modulate).
- Eosinophilia: >500/μL.
3. Basophils
- Abundance: <1% WBCs.
- Nucleus: Bilobed/S-shaped (often obscured). Granules: Histamine, heparin.
- Role: Hypersensitivity reactions (anaphylaxis); release inflammatory mediators.
Agranulocytes - The Specialized Squad
- Lack specific granules; possess azurophilic (primary) granules.
- Lymphocytes (20-40% of WBCs): Large, spherical nucleus.
- T-Lymphocytes: Mature in Thymus. Cellular immunity.
- Helper T (CD4+): Activate B cells, cytotoxic T cells, macrophages.
- Cytotoxic T (CD8+): Kill virus-infected/tumor cells.
- Regulatory T: Suppress immune response.
- B-Lymphocytes: Mature in Bone marrow. Humoral immunity.
- Differentiate into plasma cells → produce antibodies (IgM, IgG, IgA, IgD, IgE).
- Natural Killer (NK) Cells: Innate immunity; kill tumor/virally infected cells without prior sensitization.
- T-Lymphocytes: Mature in Thymus. Cellular immunity.
- Monocytes (2-8% of WBCs): Largest WBCs; kidney/horseshoe-shaped nucleus.
- Circulate for ~8 hours, then migrate to tissues → differentiate into macrophages (e.g., Kupffer cells in liver, alveolar macrophages in lungs, osteoclasts in bone) or dendritic cells.
- Functions: Phagocytosis, antigen presentation, cytokine production.
⭐ DiGeorge Syndrome: Thymic aplasia leads to deficient T-cell maturation, causing recurrent viral/fungal infections. B-cell count is normal, but T-cell dependent antibody production is impaired. Associated with CATCH-22 (Cardiac defects, Abnormal facies, Thymic hypoplasia, Cleft palate, Hypocalcemia/Hypoparathyroidism) due to 22q11.2 deletion. 📌
Key Immune Functions - Leukocyte Taskforce
-
Innate Defense: Rapid, non-specific.
- Phagocytosis: Neutrophils, Macrophages engulf microbes. Key steps: Chemotaxis, Adherence, Ingestion, Digestion.
- Inflammation: Basophils (histamine), Mast cells (histamine, leukotrienes). Eosinophils (parasites, allergy).
- NK Cells: Lyse virus-infected & tumor cells without prior sensitization.
-
Adaptive Defense: Specific, memory.
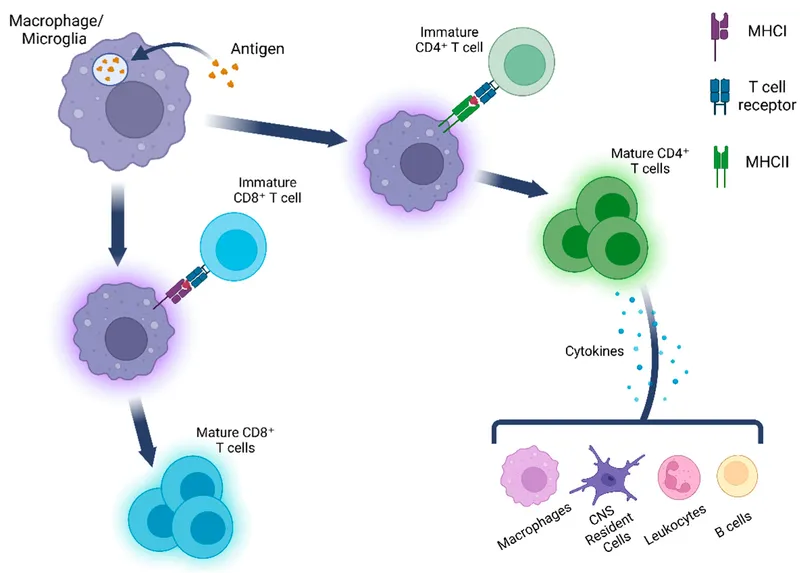
- Antigen Presentation: APCs (Macrophages, Dendritic cells, B-cells) present antigens via MHC to T-cells.
- Cell-Mediated (CMI): T-lymphocytes.
- CD4+ (Helper T cells): Orchestrate response (Th1, Th2).
- CD8+ (Cytotoxic T cells): Kill infected cells.
- Humoral (HMI): B-lymphocytes → Plasma cells → Antibodies (IgG, IgA, IgM, IgE, IgD - 📌 GAMED).
⭐ Opsonization: Coating of pathogens by opsonins (e.g., IgG, C3b) significantly enhances phagocytosis, crucial for clearing encapsulated bacteria like Streptococcus pneumoniae and Haemophilus influenzae.
High‑Yield Points - ⚡ Biggest Takeaways
- Neutrophils: Most abundant, phagocytosis in acute bacterial infections; Barr body in females.
- Eosinophils: Combat parasitic infections, mediate allergic reactions; Charcot-Leyden crystals.
- Basophils/Mast cells: Release histamine, heparin in Type I hypersensitivity via IgE.
- Monocytes become macrophages for phagocytosis, antigen presentation (e.g., Kupffer cells).
- B-lymphocytes for humoral immunity (antibodies); T-lymphocytes (CD4+, CD8+) for cell-mediated immunity.
- MHC I (all nucleated cells) presents to CD8+ T-cells; MHC II (APCs) presents to CD4+ T-cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

