ABO System - The A‑B‑Cs of Blood
- Antigens: A, B on RBCs. Antibodies: Anti-A, Anti-B in plasma.
- H antigen: Precursor for A & B antigens.
- Genetics: ABO gene; A & B codominant, O recessive.
| Group | RBC Antigen | Plasma Ab |
|---|---|---|
| A | A | Anti-B |
| B | B | Anti-A |
| AB | A, B | None |
| O | H | Anti-A, Anti-B |
- Universal Recipient (RBCs): AB.
⭐ Landsteiner's Law: ABO antigen on RBCs means corresponding antibody absent in plasma; antigen absent means antibody present (exceptions: newborns).

Rh System & HDN - Positively D‑angerous
- Rh Antigens: D is most immunogenic. Rh(D)+ (D antigen present), Rh(D)- (D antigen absent).
- Anti-D Antibodies: IgG; form after sensitization (e.g., Rh(D)+ fetal cells enter maternal circulation during pregnancy/delivery).
- HDFN Pathophysiology:
- Condition: Rh(D)- mother, Rh(D)+ fetus.
- Mechanism: Maternal IgG anti-D crosses placenta → fetal RBC hemolysis.
- Clinical Triad: Anemia, jaundice (↑bilirubin → kernicterus risk), hydrops fetalis.
- Prevention: Administration of Anti-D immunoglobulin (RhoGAM).
⭐ Anti-D immunoglobulin (RhoGAM) is administered to Rh-negative mothers carrying an Rh-positive fetus at approximately 28 weeks gestation and within 72 hours postpartum to prevent sensitization.

Compatibility Testing - Perfect Match Protocol
- Aim: Ensure safe transfusion; prevent hemolytic reactions.
- Core Protocol:
- ABO/Rh re-typing: Confirms donor & recipient groups.
- Antibody Screen: Recipient serum for unexpected antibodies.
- Crossmatch:
- Major: Recipient Serum vs Donor RBCs. Critical.
- (Minor: Donor Serum vs Recipient RBCs - less common).
- Auto-control: Recipient Serum vs Recipient RBCs.
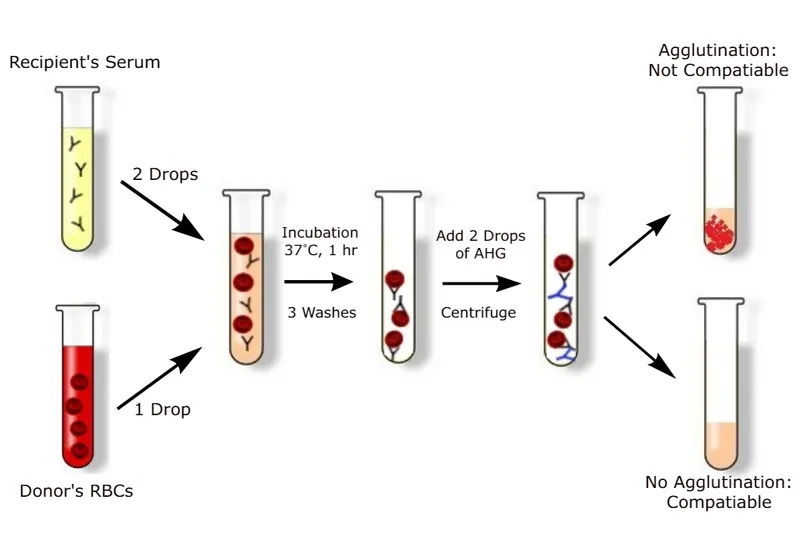
⭐ The major crossmatch, which tests the recipient's serum against the donor's red blood cells, is the most critical pre-transfusion test to prevent severe hemolytic reactions.
Transfusion Reactions - Transfusions Turn Treacherous
- Adverse events post-transfusion. ⚠️ Stop transfusion immediately! Investigate.
- Acute Hemolytic (AHTR):
⭐ AHTR: Most often ABO incompatibility (clerical error). Fever, chills, hemoglobinuria, hypotension, back pain.
- Febrile Non-Hemolytic (FNHTR): Most common. Cytokines from donor WBCs.
- Allergic/Anaphylactic: Urticaria to anaphylaxis (IgA deficiency).
- TRALI: Donor antibodies vs. recipient neutrophils; acute respiratory distress.
- TACO: Circulatory overload; dyspnea, hypertension.
- Delayed Hemolytic: Extravascular hemolysis; jaundice, ↓Hb days later.
Blood Products & Massive Transfusion - Component Toolkit
- PRBCs: ↑ Hb 1 g/dL or Hct 3%. Store 1-6°C.
- Platelets: ↑ count 5,000-10,000/μL per unit. Store 20-24°C with agitation.
- FFP: Contains all coagulation factors. Store ≤ -18°C.
⭐ Fresh Frozen Plasma (FFP) is indicated for the correction of multiple coagulation factor deficiencies, such as in liver disease, DIC, or warfarin overdose (along with Vitamin K). It should be ABO compatible.
- Cryoprecipitate: Rich in Fibrinogen, Factor VIII, vWF, Factor XIII. Store ≤ -18°C.
- Massive Transfusion: Replacement of >1 blood volume in 24 hrs or >50% in 4 hrs.
- Aim for 1:1:1 ratio (PRBC:FFP:Platelets).
- Risks: Hypothermia, coagulopathy, hypocalcemia (citrate), hyperkalemia.
High‑Yield Points - ⚡ Biggest Takeaways
- ABO antibodies: IgM, naturally occurring. Rh antibodies: IgG, immune, cross placenta (HDN risk).
- Universal donor: O Rh-negative (RBCs). Universal recipient: AB Rh-positive (RBCs).
- Bombay blood group (Oh): Lacks H antigen; has anti-A, anti-B, anti-H. Only Oh blood compatible.
- Major cross-match (donor RBCs + recipient serum) prevents acute hemolytic reactions.
- Febrile non-hemolytic reaction: Most common; due to leukocyte cytokines.
- Massive transfusion: Risks include hypocalcemia, hyperkalemia, coagulopathy, hypothermia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

