Migraine Pathophysiology & Overview - Brain's Ache Saga
- Definition: Episodic headache disorder; with or without aura (transient focal neurological symptoms).
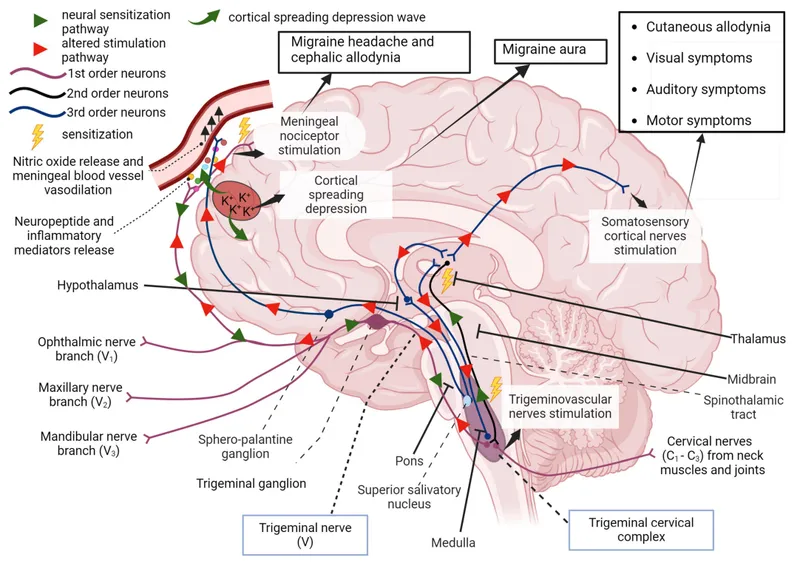
- Neurovascular Theory: Primary neuronal dysfunction triggers secondary vascular changes.
- Cortical Spreading Depression (CSD): Self-propagating wave of neuronal/glial depolarization; underlies migraine aura.
- Activates trigeminal nerve afferents.
- Trigeminovascular System Activation: Central to pain.
- Key Mediators:
- CGRP (Calcitonin Gene-Related Peptide): Potent vasodilator; neurogenic inflammation.
- Serotonin (5-HT): Imbalance; 5-HT1B/1D/1F receptor agonism is a key therapeutic target.
- Substance P, Neurokinin A.
⭐ Activation of the trigeminovascular system releases CGRP, a key player in migraine pain.
Acute Migraine Treatment - Attack Abort!
- Care Approaches:
- Stratified: Match initial treatment to attack severity.
- Step-care: Start with simple analgesics, escalate if no response.
⭐ Stratified care is often preferred for faster relief and improved outcomes in moderate to severe attacks.
- Non-Specific Analgesics (Limit use to <15 days/month to avoid MOH):
- NSAIDs: Ibuprofen, Naproxen, Diclofenac, Aspirin.
- Paracetamol.
- Antiemetics (Adjunctive for N/V; some have intrinsic anti-migraine effects):
- Metoclopramide, Domperidone, Prochlorperazine.
- Migraine-Specific Agents (Limit use to <10 days/month to avoid MOH):
- Triptans (5-HT1B/1D Agonists → vasoconstriction, ↓CGRP release):
- E.g., Sumatriptan, Rizatriptan, Zolmitriptan, Naratriptan, Eletriptan.
- ADRs: 'Triptan sensations' (chest tightness), flushing.
- CIs: CAD, stroke/TIA, uncontrolled HTN, hemiplegic/basilar migraine.
- 📌 Mnemonic: 'A TRIP to the ANus constricts vessels' (vasoconstriction).
- Ergot Alkaloids (Non-selective 5-HT1, $\alpha$-adrenergic, dopaminergic):
- Ergotamine, Dihydroergotamine (DHE).
- ADRs: N/V, ergotism.
- CIs: CAD, PVD, HTN, pregnancy, potent CYP3A4 inhibitors.
- CGRP Antagonists (Gepants) (Small molecule CGRP receptor antagonists):
- Ubrogepant, Rimegepant.
- Advantages: No vasoconstriction.
- 5-HT1F Receptor Agonists (Ditans) (Selective 5-HT1F agonist):
- Lasmiditan.
- Advantages: No vasoconstriction; useful if triptans CI due to CV risk.
- ADRs: Dizziness (driving impairment warning).
- Triptans (5-HT1B/1D Agonists → vasoconstriction, ↓CGRP release):
- Medication Overuse Headache (MOH):
- Prevention: Limit acute meds (simple analgesics <15 days/month; triptans/ergots/combo <10 days/month).
Preventive Migraine Treatment - Shield Up Strategies
Indications: ≥4 headache days/month, ≥2 with disability, debilitating attacks, or acute med issues.
- Oral Prophylactics (selected by comorbidity/ADR profile):
- Beta-blockers: Propranolol, Metoprolol. MOA: ?Modulate adrenergic/serotonergic systems. ADRs: Fatigue, bradycardia, hypotension. CIs: Asthma, heart block.
- Antidepressants: Amitriptyline (TCA). MOA: NE & 5-HT reuptake inhibition. ADRs: Sedation, anticholinergic, weight gain. Venlafaxine (SNRI) alternative.
- Anticonvulsants:
- Topiramate: MOA: Blocks Na+/Ca2+ channels, ↑GABA. ADRs: Paresthesia, cognitive slowing ('Dopamax'), weight loss, kidney stones. Teratogenic.
- Valproic Acid: MOA: ↑GABA, blocks Na+/T-type Ca2+ channels. ADRs: Weight gain, tremor, hepatotoxicity. ⚠️ Highly teratogenic.
⭐ 📌 Valproic Acid: Highly teratogenic (neural tube defects) - Black Box Warning.
- Injectable Prophylactics:
- CGRP Monoclonal Antibodies: Erenumab (receptor), Fremanezumab, Galcanezumab (ligand). SC monthly/quarterly. ADRs: Injection site reactions, constipation (Erenumab).
- OnabotulinumtoxinA: For chronic migraine (≥15 headache days/month). MOA: Inhibits CGRP release. Admin: 31 specific sites.
- Other Options: Candesartan (ARB), Riboflavin (Vit B2), Coenzyme Q10, Magnesium.
- Menstrual Migraine Prophylaxis: Frovatriptan, NSAIDs perimenstrually.

High‑Yield Points - ⚡ Biggest Takeaways
- Triptans (5-HT1B/1D agonists) are first-line for acute migraine attacks; contraindicated in CAD/PVD.
- Ergotamine (non-selective 5-HT agonist) causes significant vasoconstriction and nausea; less preferred.
- CGRP antagonists ("-gepants" for acute, "-mabs" for prophylaxis) are novel targeted therapies.
- Prophylaxis mainstays: Propranolol, Amitriptyline, Topiramate, Valproate, CGRP mAbs.
- Risk of Serotonin Syndrome with concurrent use of triptans/ergots and SSRIs/SNRIs.
- Medication Overuse Headache (MOH) is a critical concern with frequent acute drug use (≥10-15 days/month).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

