Hirschsprung's: Intro & Pathophysiology - Gut's Nerve Nap
- Pathophysiology: Congenital aganglionosis of distal gut.
- Due to failed neural crest cell migration (neuroblasts) to hindgut.
- Arrest occurs during 5th-12th weeks gestation.
- Progression: Craniocaudal (distal to proximal).
- Key Features:
- Rectum always involved.
- Leads to functional obstruction; affected segment remains tonically contracted.
- 📌 Mnemonic: 'HIrschsprung = HIgh up the colon involvement is less common' (short segment more common).
⭐ The aganglionosis in Hirschsprung's disease always involves the rectum and extends proximally for a variable distance.
 oka
oka
Hirschsprung's: Clinical Features - The Poop Stoppage
- Neonatal Onset (Most Common):
- Delayed meconium passage: No stool within 24-48 hours post-birth.
- Bilious (green) emesis.
- Progressive abdominal distension.
- Feeding refusal or intolerance.
- Tight anal sphincter; explosive stool/gas on DRE (digital rectal exam) ("squirt sign" - suggestive).
- Later Presentation (Infancy/Childhood):
- Chronic, intractable constipation (often since birth).
- Foul-smelling, "ribbon-like" or pellet-like stools.
- Marked abdominal distension, sometimes with visible peristalsis.
- Failure to thrive (FTT); malnutrition.
- ⚠️ Hirschsprung-Associated Enterocolitis (HAEC): fever, explosive diarrhea, distension, sepsis risk.
⭐ Failure to pass meconium in the first 24-48 hours of life is a cardinal sign of Hirschsprung's disease in a full-term infant.
Hirschsprung's: Diagnosis - Finding the Freeze
- Initial Imaging:
- Abdominal X-ray (AXR): Suggestive findings include dilated proximal bowel loops, paucity of gas distally.
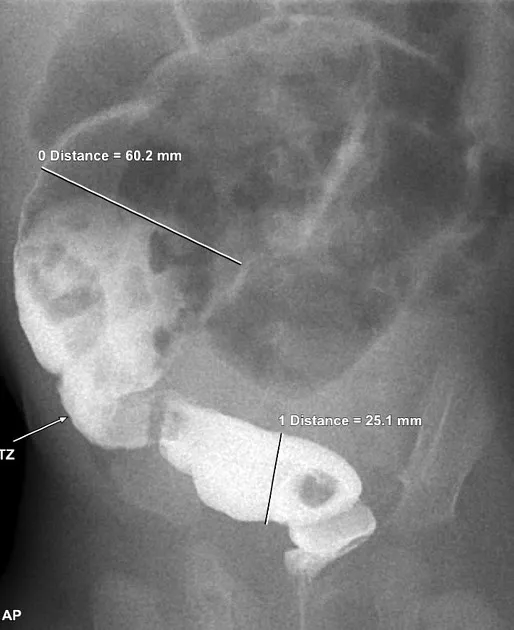
- Contrast Enema (Barium/water-soluble): Crucial for identifying the transition zone (narrowed aganglionic segment, dilated ganglionic proximal colon). Retention of contrast > 24 hours is highly suggestive.
- 📌 "Transition Zone = Trouble Zone"
- Functional Test:
- Anorectal Manometry: Demonstrates absence of the Rectoanal Inhibitory Reflex (RAIR). Especially useful in older children; less reliable in neonates.
- Gold Standard Confirmation:
- Rectal Suction Biopsy: Shows absence of ganglion cells in the submucosa. Increased acetylcholinesterase staining in nerve fibers is characteristic.
⭐ Full-thickness rectal biopsy (shows absent ganglion cells in submucosal & myenteric plexuses) is the gold standard.
- Full-thickness biopsy if suction biopsy is inconclusive or for atypical cases.
- Rectal Suction Biopsy: Shows absence of ganglion cells in the submucosa. Increased acetylcholinesterase staining in nerve fibers is characteristic.
Hirschsprung's: Management - Rerouting the Gut
- Initial:
- Decompression: Rectal irrigation, NG tube.
- IV fluids, antibiotics.
- Nutritional support.
- Surgical:
- Goal: Resect aganglionic bowel, pull-through ganglionic segment to anus.
- Single-stage pull-through vs. Staged (colostomy, then pull-through).
- Procedures:
- Swenson: Resection, end-to-end anastomosis.
- Soave: Endorectal mucosectomy, pull-through.
- Duhamel: Retrorectal pull-through.

- Complications:
- Hirschsprung-Associated Enterocolitis (HAEC).
⭐ Hirschsprung-Associated Enterocolitis (HAEC) is the most common and life-threatening complication, even post-surgery.
- Anastomotic leak/stricture.
- Incontinence, obstructive symptoms.
- Hirschsprung-Associated Enterocolitis (HAEC).
Hirschsprung's: Genetics & Syndromes - Family Ties & Woes
- Key Genetic Loci:
- RET proto-oncogene: Most common; mutations often in familial & long-segment HSCR.
- EDNRB & EDN3: Endothelin-B receptor pathway genes.
- Associated Syndromes (Increased Risk):
- Down syndrome (Trisomy 21)
- Waardenburg syndrome (Type IV)
- MEN 2A/2B (RET mutations)
- Mowat-Wilson syndrome (ZEB2)
⭐ Mutations in the RET proto-oncogene are the most frequently identified genetic cause of Hirschsprung's disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Congenital aganglionosis of the distal bowel, primarily due to failed neural crest cell migration.
- Most commonly affects the rectosigmoid colon (short-segment disease).
- Key presentation: Failure to pass meconium within 24-48 hours, bilious vomiting, and abdominal distension.
- Gold standard for diagnosis: Rectal suction biopsy demonstrating the absence of ganglion cells.
- Barium enema often shows a transition zone between a narrowed aganglionic segment and a dilated proximal bowel.
- Strong association with Down syndrome (Trisomy 21).
- Definitive treatment involves surgical resection of the aganglionic segment; monitor for Hirschsprung-Associated Enterocolitis (HAEC) post-operatively.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

