Introduction & Embryology - Hernia Genesis
- CDH: Protrusion of abdominal viscera into thoracic cavity due to a congenital diaphragmatic defect.
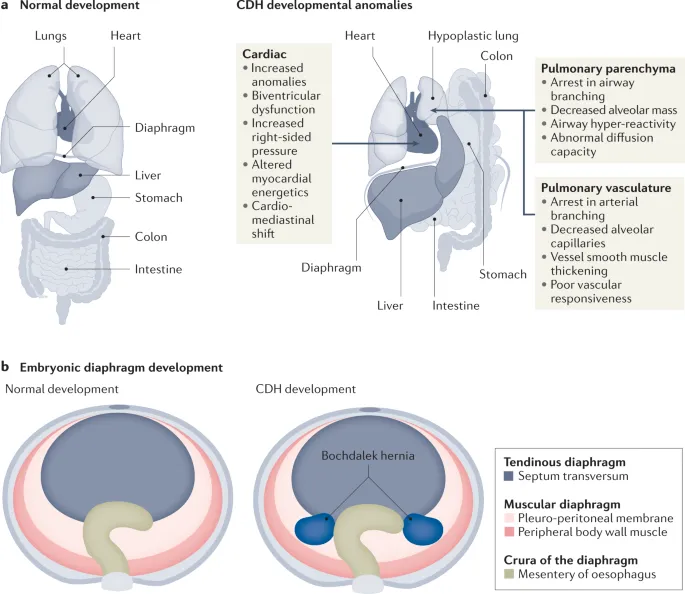
- Embryology: Diaphragm develops from four main embryonic structures:
- Septum transversum (forms central tendon)
- Pleuroperitoneal membranes (fuse to close pleuroperitoneal canals)
- Dorsal mesentery of esophagus (forms crura)
- Muscular ingrowth from lateral body walls.
- Hernia Genesis: Primarily due to failure of fusion of the pleuroperitoneal membranes, usually posterolaterally.
- Critical Window: This developmental failure occurs around 8-10 weeks of gestation.
⭐ Failure of pleuroperitoneal membrane closure, most commonly posterolaterally, around 8-10 weeks gestation leads to CDH.
Types & Associated Anomalies - Defect Varieties
- Bochdalek Hernia (Posterolateral): 📌 BPM LLL (Bochdalek Postero-lateral, More common, Left, Lung hypoplasia)
- Most common type (~85-90%).
- Predominantly left-sided (~85% of Bochdalek cases).
- Leads to pulmonary hypoplasia.
- Morgagni Hernia (Anteromedial/Retrosternal):
- Less common (~2-5%).
- Usually right-sided.
- Eventration of Diaphragm:
- Abnormal elevation; intact but thinned diaphragm.
- Associated Anomalies (~30-50% cases):
- Cardiac (e.g., VSD, ASD).
- CNS (e.g., neural tube defects).
- Renal, Skeletal.
- Chromosomal (e.g., Trisomy 13, 18, 21).
⭐ Bochdalek hernia (posterolateral) is the most common type (~85-90%), predominantly on the left (~85% of Bochdalek cases).
Pathophysiology & Clinical Features - Breathing Battle
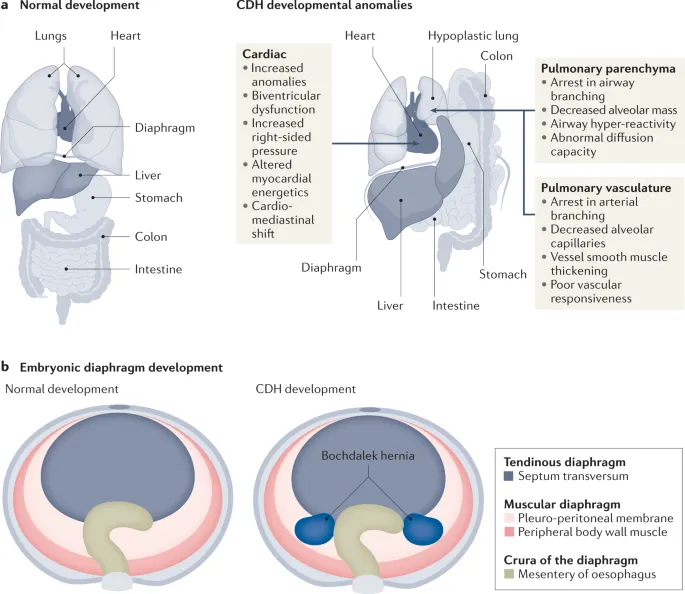
- Pathophysiology:
- Abdominal viscera herniate into thorax → lung compression.
- Leads to:
- Pulmonary hypoplasia: ↓ alveoli, bronchioles, vasculature (often bilateral).
- Persistent Pulmonary Hypertension (PPHN): ↑ pulmonary vascular resistance.
- Surfactant deficiency common.
- Clinical Features:
- Immediate/early severe respiratory distress: cyanosis, tachypnea, retractions.
- Scaphoid abdomen (empty, concave).
- Bowel sounds audible in chest.
- Barrel-shaped chest.
- Displaced heart sounds.
⭐ Key pathophysiological defects are pulmonary hypoplasia (often bilateral, though defect is unilateral) and persistent pulmonary hypertension (PPHN).
Diagnosis & Management - Spot, Stabilize, Sew
-
Diagnosis (Spot)
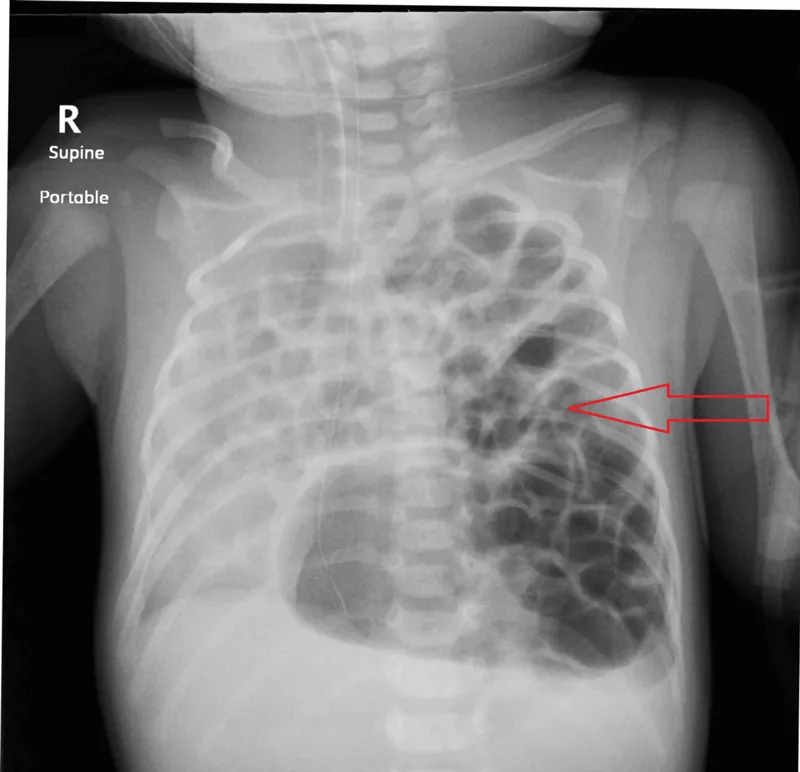
- Prenatal US: Polyhydramnios, mediastinal shift, bowel/liver in chest.
- Postnatal: Resp. distress, scaphoid abdomen, ↓ breath sounds. CXR confirms.
-
Management (Stabilize & Sew)
- 📌 Intubate, NG/OG tube, Stabilize, Surgery (INSure Survival!)
-
⭐ Immediate postnatal management: intubate, decompress stomach/bowel with NG/OG tube, and strictly avoid bag-mask ventilation.
- Stabilize: Gentle vent; Target $PaCO_2$ 45-65 mmHg; PPHN (iNO, ECMO).
- Surgical repair: After stabilization (24-72 hrs).
Prognosis & Complications - The Long Haul
- Survival: ~70-90% with modern neonatal care.
- Prognosis hinges on:
- Pulmonary hypoplasia severity.
- Associated anomalies.
- Persistent pulmonary hypertension (PPHN).
⭐ Prenatally measured Lung-to-Head Ratio (LHR) and liver herniation ('liver-up') are critical prognostic indicators.
- Long-term sequelae:
- Chronic lung disease, GERD.
- Neurodevelopmental delay, hearing loss.
- Recurrence, chest wall deformities (scoliosis/pectus).
High‑Yield Points - ⚡ Biggest Takeaways
- Bochdalek hernia (left posterolateral) is the most common CDH.
- Defect in pleuroperitoneal membrane closure is the cause.
- Pulmonary hypoplasia and pulmonary hypertension are critical determinants of survival.
- Presents with respiratory distress, scaphoid abdomen, and bowel sounds in chest at birth.
- Diagnosis: prenatal ultrasound or postnatal chest X-ray showing bowel in thorax.
- Management: Immediate intubation, gastric decompression, delayed surgical repair after stabilization.
- Associated anomalies, especially cardiac, are common and impact prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more