Bacterial Meningitis - Pus Under Pressure
Life-threatening CNS emergency! Early diagnosis & treatment crucial.
CSF Analysis - Comparative Table:
| Feature | Bacterial | Viral | TB Meningitis |
|---|---|---|---|
| Glucose | ↓ (<40 mg/dL) | Normal | ↓ (<40 mg/dL) |
| Protein | ↑↑ (>100 mg/dL) | Normal/Slightly ↑ | ↑↑ (100-1000 mg/dL) |
| Cells (WBC) | ↑↑ (PMNs >1000/µL) | ↑ (Lymphs <500/µL) | ↑ (Lymphs 100-500/µL) |
| Gram Stain | Positive | Negative | Negative (AFB for TB) |
- Neonates (<1mo): 📌 "LEGS" - Listeria, E. coli, Group B Strep.
- 1mo-12yr: S. pneumoniae, N. meningitidis, Hib (unimmunized).
-
12yr: N. meningitidis, S. pneumoniae.
Empirical Antibiotics (IV):
- Neonates: Ampicillin + Cefotaxime.
- 1mo-50yr: Vancomycin + Ceftriaxone.
-
50yr/Immunocompromised: Add Ampicillin (for Listeria). Duration: 7-21 days (organism-dependent).
⭐ CSF opening pressure is typically elevated (>180 mmH₂O) in bacterial meningitis.

Viral CNS & ADEM - Viral Invaders & Autoimmune Storms
-
Viral (Aseptic) vs. Bacterial Meningitis (CSF Findings):
Feature Viral Meningitis Bacterial Meningitis Opening Pressure Normal / Slightly ↑ Markedly ↑ WBCs Lymphocytic pleocytosis Neutrophilic pleocytosis Protein Normal / Mildly ↑ Markedly ↑ Glucose Normal ↓ (often < 40 mg/dL) Gram Stain Negative Often Positive -
Herpes Simplex Encephalitis (HSE):
- Most common cause of sporadic fatal encephalitis.
- Key: Temporal lobe predilection, hemorrhagic changes.
- Rx: Acyclovir 10-15 mg/kg IV q8h.
-
Japanese Encephalitis (JE):
- Flavivirus; mosquito vector (Culex).
- Key: Extrapyramidal symptoms (parkinsonism, dystonia), thalamic lesions.
- Prevention: Vaccination, mosquito control.
-
Acute Disseminated Encephalomyelitis (ADEM):
- Post-infectious/post-vaccinal immune-mediated demyelination.
- MRI: Multifocal, asymmetric white matter lesions (often large, fluffy).
- Rx: High-dose corticosteroids.
⭐ ADEM is typically monophasic; recurrent or multiphasic forms raise suspicion for Multiple Sclerosis (MS).
Chronic & Focal CNS Infections - Stealthy & Stubborn Foes
- Tuberculous Meningitis (TBM)
- Stages: I (non-specific), II (meningism, CN palsies), III (coma, severe deficits).
- CSF: Cobweb coagulum, ↑Protein (100-500 mg/dL), ↓Glucose (<45 mg/dL or <40% blood glucose), lymphocytes, ↑ADA (>10 U/L).
- Rx: ATT (RHEZ) + Steroids (e.g., Dexamethasone 0.4 mg/kg/day).
- Complications: Hydrocephalus, vasculitis, tuberculomas.
- Fungal Meningitis (esp. Cryptococcal)
- Risk: Immunocompromised (HIV, steroids).
- Dx: India ink stain (CSF), Cryptococcal antigen (CrAg) test.
- Rx: Amphotericin B + Flucytosine, then Fluconazole.
- Neurocysticercosis (NCC)
- Commonest parasitic CNS infection in India.
- Stages: Vesicular → Colloidal → Granular → Calcified.
- Presentation: Seizures (most common).
- Rx: Albendazole (15 mg/kg/day) + Steroids (for viable cysts).
⭐ Scolex seen within the cyst in the vesicular stage on imaging is pathognomonic for NCC.
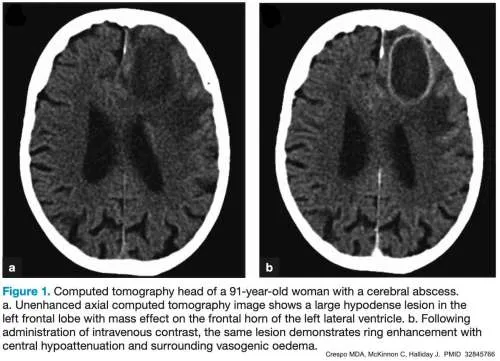
- Brain Abscess
- Predisposing: Otitis, sinusitis, dental sepsis, CHD.
- Classic triad (often incomplete <50%): Fever, headache, focal deficits.
- Imaging: Ring-enhancing lesion on CT/MRI.
- Rx: IV antibiotics +/- surgical drainage.
Neonatal & Congenital CNS Infections - Early Onset Onslaught
- Neonatal Meningitis:
- Onset: Early (<7 days), Late (7-90 days).
- Pathogens: Group B Strep (GBS), E. coli, Listeria monocytogenes.
- Signs: Subtle (fever, poor feeding, irritability, lethargy, seizures).
- Rx: Empirical Ampicillin + Gentamicin or Cefotaxime.
- Congenital (TORCH) CNS Infections:
- CMV: Periventricular calcifications, microcephaly, SNHL.
- Toxoplasmosis: Classic triad (chorioretinitis, hydrocephalus, intracranial calcifications). 📌 Sabin-Feldman dye test.
- Rubella: Microcephaly, cataracts, deafness, PDA, "blueberry muffin" rash.
- HSV: Skin vesicles, encephalitis (temporal lobe), seizures.

⭐ CMV is the most common congenital infection.
High‑Yield Points - ⚡ Biggest Takeaways
- Neonatal meningitis: Pathogens: Group B Strep, E. coli, Listeria.
- Childhood bacterial meningitis: S. pneumoniae, N. meningitidis common; Hib (unvaccinated).
- CSF: Bacterial (↑protein, ↓glucose, PMNs); Viral (N/↑protein, N glucose, lymphocytes); TB (↑↑protein, ↓↓glucose, lymphocytes).
- Tuberculous meningitis: Basal exudates, cranial nerve palsies, hydrocephalus; CSF: markedly low glucose.
- Herpes Simplex Encephalitis: Hemorrhagic temporal lobe involvement; treat with IV Acyclovir.
- Bacterial meningitis sequelae: Sensorineural hearing loss (most common), seizures, hydrocephalus.
- Brain abscess: Ring-enhancing lesion; risk: cyanotic heart disease, sinusitis/otitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

