Hydronephrosis: Definition & Overview - Swollen Kidneys 101
- Definition: Dilation of the renal pelvis and calyces due to impaired urine outflow (obstruction).
- Pathophysiology: Leads to ↑ intra-renal pressure, potentially causing progressive renal parenchymal damage, atrophy, and ↓ GFR.
- Key Classifications:
- Laterality: Unilateral or Bilateral.
- Etiology/Onset: Congenital (e.g., PUJO, VUR) or Acquired (e.g., calculi, tumors, strictures).
- Timing: Acute or Chronic.
- Severity Grading: Commonly by Society for Fetal Urology (SFU) system (Grades 0-IV).

⭐ [Placeholder for exam-favourite fact]
Hydronephrosis: Etiology & Pathophysiology - The Blockage Culprits
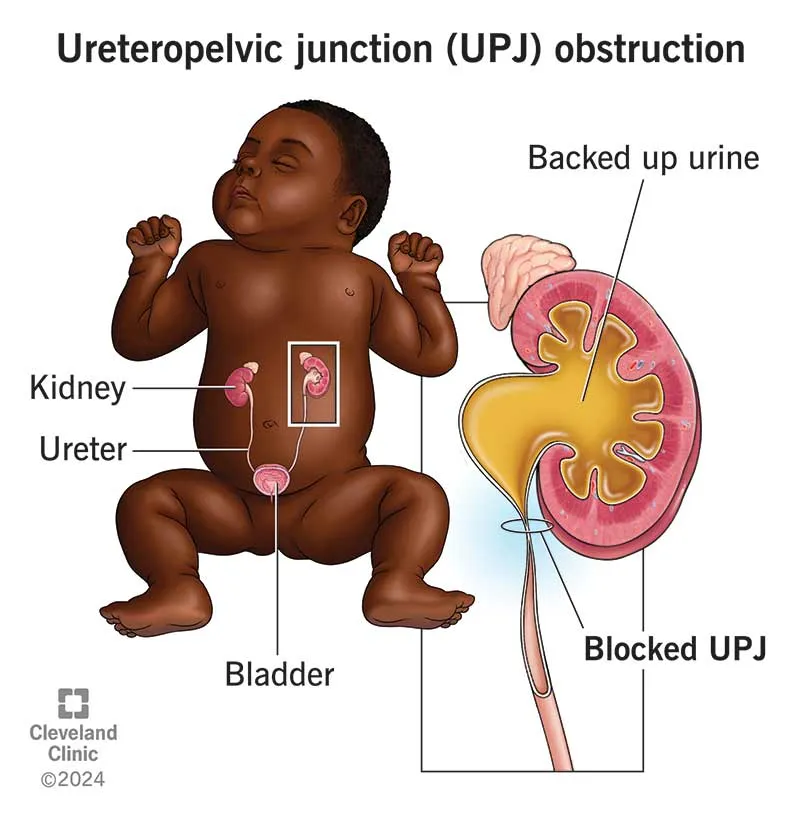
Pathophysiology: Obstruction → ↑ Pressure → Dilation → Damage
- Primary Blockage Culprits:
- Ureteropelvic Junction Obstruction (UPJO): Most common overall.
- Posterior Urethral Valves (PUV): Key cause in newborn males.
- Vesicoureteral Reflux (VUR): High grades (e.g., IV-V) can lead to hydronephrosis.
- Ureterovesical Junction Obstruction (UVJO).
- Other Contributing Factors:
- Ureterocele, ectopic ureter.
- Neurogenic bladder dysfunction.
- Acquired: Stones, strictures, extrinsic compression (e.g., aberrant vessels, tumors).
⭐ UPJO is the most common cause of significant antenatal hydronephrosis.
Hydronephrosis: Clinical Presentation - Spotting Trouble Signals
- Antenatal: Often an incidental finding on routine maternal ultrasound.
- Postnatal:
- Frequently asymptomatic, especially if unilateral.
- Palpable abdominal/flank mass.
- Recurrent UTIs: fever, irritability, vomiting, poor feeding.
- Failure to thrive (FTT).
- Gross or microscopic hematuria.
- Intermittent flank/abdominal pain (older children, Dietl's crisis).
- Rarely, hypertension.
⭐ Antenatal hydronephrosis (ANH) is the most common urological anomaly detected on prenatal ultrasound, affecting 1-5% of pregnancies.
Hydronephrosis: Diagnosis & Grading - Kidney Detective Work
- Initial Imaging: Ultrasonography (USG) is primary.
- Antenatal: Measures Anteroposterior Diameter (APD).
- Mild: APD <10mm (2nd tri), <10-15mm (3rd tri).
- Severe: APD >15mm (3rd tri).
- Postnatal: Confirms, monitors, guides further tests. APD >10mm significant.
- Antenatal: Measures Anteroposterior Diameter (APD).
- Diagnostic Flow:
- Key Investigations:
- Micturating Cystourethrogram (MCU): Essential for VUR, Posterior Urethral Valves (PUV).
- Diuretic Renography (MAG3/DTPA): Differentiates obstructive vs. non-obstructive.
⭐ T1/2 > 20 minutes post-furosemide strongly suggests obstruction.
- SFU Grading (Society for Fetal Urology):
- G1: Pelvis dilated. G2: Pelvis + some calyces.
- G3: All calyces dilated, normal parenchyma. G4: G3 + parenchymal thinning.

Hydronephrosis: Management Principles - Fixing the Plumbing
- Core Goals: Relieve obstruction, preserve renal function, prevent complications (UTI, stones).
- Strategy: Based on severity (SFU grade), symptoms, laterality, etiology, and renal function (DRF).
- Conservative: Watchful waiting, serial USG. Antibiotics for recurrent UTI / high-grade VUR.
- Intervention: ↑SFU grade, DRF < 40% or ↓ > 10%, symptoms, complications (UTI, stones).
- Surgical:
- Definitive (etiology-based): Pyeloplasty (PUJO), ureteric reimplantation (VUR/VUJO), valve ablation (PUV).
- Temporary (severe obstruction/sepsis): PCN, ureteric stent.
⭐ Most cases of antenatally detected, asymptomatic, unilateral hydronephrosis with good differential renal function (DRF > 40%) can be managed conservatively with serial monitoring.
High-Yield Points - ⚡ Biggest Takeaways
- Hydronephrosis, dilation of renal pelvis/calyces, is most commonly due to pelviureteric junction (PUJ) obstruction.
- Often first identified on routine antenatal ultrasound.
- Postnatal workup: renal ultrasound (RUS), MCU/VCUG (for VUR), and diuretic renography (DRS/MAG3 scan) to assess obstruction.
- The Society for Fetal Urology (SFU) grading system is widely used for severity.
- Complications include recurrent UTIs, renal scarring, and impaired renal function.
- Management: Observation or surgical pyeloplasty for significant PUJO and/or symptomatic cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

