AKI: Definition & Staging - Kidney SOS Stages
- Definition: Sudden ↓ kidney function: ↑ serum creatinine (sCr) & ↓ urine output (UO).
- Staging (KDIGO-based / Kidney SOS adapted):
- Stage 1:
- sCr: ↑ ≥0.3 mg/dL (in 48h) OR 1.5-1.9x baseline
- UO: < 0.5 mL/kg/hr for 6-12 hrs
- Stage 2:
- sCr: ↑ 2.0-2.9x baseline
- UO: < 0.5 mL/kg/hr for ≥12 hrs
⭐ Oliguria in neonates is defined as urine output < 1 mL/kg/hr, and < 0.5 mL/kg/hr in older children.
- Stage 3:
- sCr: ↑ ≥3.0x baseline OR sCr ≥4.0 mg/dL OR RRT init.
- UO: < 0.3 mL/kg/hr for ≥24 hrs OR Anuria ≥12 hrs
- Stage 1:
AKI: Etiology - Tiny Trouble Triggers
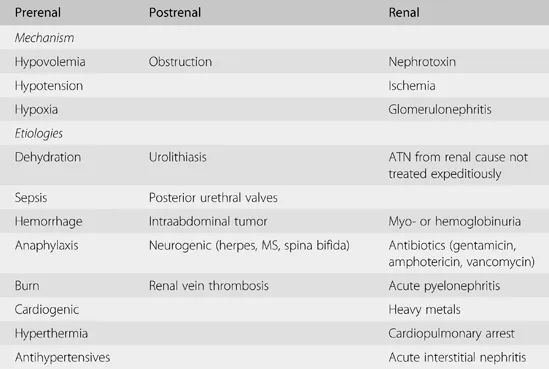
- AKI arises from prerenal, intrinsic renal, or postrenal causes.
- Prerenal (most common in children, ~70%):
- ↓ Perfusion: Dehydration (diarrhea, vomiting), sepsis, shock, hemorrhage.
- ↓ Effective volume: Heart failure, nephrotic syndrome.
- Intrinsic Renal (~20%):
- Acute Tubular Necrosis (ATN): Ischemia (prolonged prerenal), nephrotoxins (aminoglycosides, NSAIDs).
- Glomerulonephritis (GN): PSGN, IgA nephropathy.
- Hemolytic Uremic Syndrome (HUS). 📌 (D+ HUS: E.coli O157:H7)
- Acute Interstitial Nephritis (AIN): Drugs, infections.
- Postrenal (~5-10%):
- Posterior Urethral Valves (PUV) in boys.
- Stones, tumors, neurogenic bladder.
⭐ Hemolytic Uremic Syndrome (HUS) is a leading cause of intrinsic AKI in young children, often post-diarrheal (D+ HUS).
AKI: Diagnosis - Spotting Sick Kidneys
Clinical Clues:
- ↓UO: Oliguria (<0.5-1 mL/kg/hr), Anuria (<0.1 mL/kg/hr)
- Edema, Hypertension
- Hematuria, pallor, nausea
Key Investigations:
| Test | Finding |
|---|---|
| UO | ↓ (Oliguria/Anuria) |
| sCr/BUN | ↑ (sCr ↑ KDIGO: ≥0.3mg/dL or 1.5x baseline) |
| Electrolytes | K⁺↑, Na⁺↓, PO₄³⁻↑, Ca²⁺↓, Acidosis |
| Urinalysis | Casts (muddy brown in ATN), proteinuria |
| FeNa | $FeNa = \frac{U_{Na} \times P_{Cr}}{P_{Na} \times U_{Cr}} \times 100%$ (Prerenal <1%, Intrinsic >2%) |
| USG KUB | Obstruction, size, echotexture |
AKI: Management & Complications - Fixing & Future Foes
- General: Treat cause, optimize hemodynamics, avoid nephrotoxins, monitor I/O, weight.
- Fluids: Euovolemia goal. Challenge: 10-20 mL/kg isotonic crystalloid if hypovolemic. Restrict if overloaded/oliguric.
- Electrolytes:
- Hyperkalemia (K+ > 6.5 mEq/L or ECG changes): Ca gluconate, Insulin-Dextrose, Salbutamol.
- Acidosis (pH < 7.1): Bicarbonate (cautiously).
- Complications: CKD, HTN, anemia.
⭐ Life-threatening hyperkalemia (K+ > 6.5 mEq/L with ECG changes) is a critical emergency in AKI requiring immediate intervention including calcium gluconate, insulin-glucose, and beta-agonists.
High‑Yield Points - ⚡ Biggest Takeaways
- Prerenal azotemia (hypovolemia, sepsis) is the most common cause of pediatric AKI.
- Oliguria is a key sign; non-oliguric AKI also occurs.
- FeNa < 1% typically indicates prerenal AKI.
- Urine microscopy is vital: muddy brown casts suggest Acute Tubular Necrosis (ATN).
- Manage by treating cause, ensuring fluid balance, and correcting electrolytes.
- Hemolytic Uremic Syndrome (HUS) is a major cause of intrinsic renal AKI.
- Dialysis indications: AEIOU (Acidosis, Electrolytes, Intoxication, Overload, Uremia).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

