Normal Puberty & Definitions - Timing is Everything
- Normal Onset: Girls 8-13 yrs (thelarche); Boys 9-14 yrs (gonadarche).
- Definitions:
- Precocious: Girls <8 yrs; Boys <9 yrs.
- Delayed: Girls >13 yrs (no thelarche) or no menarche by 15 yrs; Boys >14 yrs (no gonadarche).
- Sequence (Girls): Thelarche → Pubarche → PHV → Menarche. (📌 B-P-P-M: Breast, Pubic hair, Peak height, Menarche)
- Sequence (Boys): Gonadarche → Pubarche → Spermarche → PHV.
- Hormonal Axis: Hypothalamic-Pituitary-Gonadal (HPG) axis activation. Adrenarche (adrenal androgens).
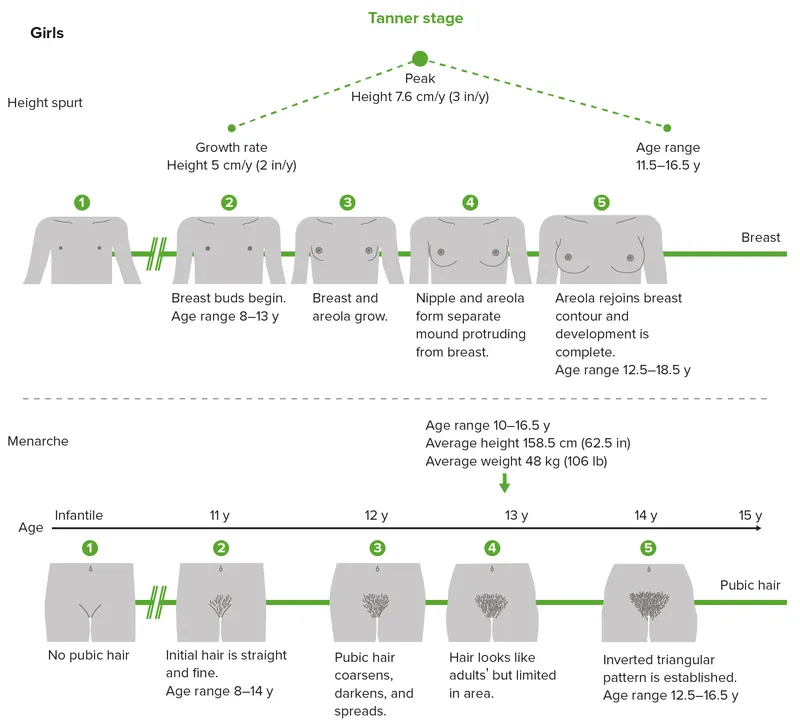
⭐ The first sign of puberty in girls is usually thelarche (breast budding), while in boys it is testicular enlargement (≥4ml volume or ≥2.5cm length).
Precocious Puberty - Early Bloomers Unveiled
- Onset of secondary sexual characteristics: Girls <8 yrs, Boys <9 yrs.
- Types:
- Central (GnRH-dependent): Premature HPG axis activation.
- Causes: Idiopathic (most common, esp. girls), CNS lesions (hamartoma, glioma).
- Peripheral (GnRH-independent): Excess sex steroids (gonadal/adrenal/exogenous).
- Causes: McCune-Albright syndrome (MAS), CAH, tumors (ovarian, testicular, adrenal).
- Central (GnRH-dependent): Premature HPG axis activation.
- Clinical: Early thelarche/menarche (girls); testicular enlargement (>4ml or >2.5cm) (boys); accelerated growth, advanced bone age.
- Investigations:
- Bone Age (X-ray hand/wrist).
- Basal LH, FSH; Estradiol/Testosterone.
- GnRH Stimulation Test: Differentiates Central (↑LH) vs. Peripheral (↓LH).
- Imaging: Brain MRI (if Central); Pelvic/Testicular USG.
- Management:
- Central: GnRH agonists (e.g., Leuprolide).
- Peripheral: Treat underlying cause.
⭐ McCune-Albright Syndrome: Triad of polyostotic fibrous dysplasia, irregular café-au-lait spots ("Coast of Maine" border), and autonomous endocrine hyperfunction (e.g., GnRH-independent precocious puberty).
Delayed Puberty - Late Starters Explained
- No secondary sex characteristics: girls by 13 yrs, boys by 14 yrs. No menarche by 16 yrs.
- Causes:
- Constitutional Delay of Growth & Puberty (CDGP): Most common, family Hx. "Late bloomers".
- Hypogonadotropic Hypogonadism (↓FSH/LH): Kallmann (anosmia), CNS issues (tumors), chronic illness, malnutrition.
- Hypergonadotropic Hypogonadism (↑FSH/LH): Gonadal failure (Turner XO, Klinefelter XXY), chemo/radiotherapy.
- Clinical Features:
- Girls: No thelarche by 13 yrs, no menarche by 16 yrs.
- Boys: Testicular volume < 4ml or length < 2.5cm by 14 yrs.
- Short stature, delayed bone age.
- Investigations:
- Bone age (X-ray wrist).
- Hormones: LH, FSH, Estradiol/Testosterone. Karyotype.
- GnRH stimulation test (differentiates CDGP from hypogonadotropic hypogonadism).
- Imaging: Pelvic USG (girls), MRI brain (if CNS signs/symptoms).
- Management:
- CDGP: Reassurance. Short-term low-dose sex steroids if significant psychosocial distress.
- Specific: Treat underlying cause. Hormone Replacement Therapy (HRT).
⭐ Constitutional delay of growth and puberty (CDGP) is the most common cause of delayed puberty, often with a positive family history.
 Mnemonic: 📌 "LATE": Low hormones (central), Age (bone age delayed), Turner's/Klinefelter's (gonadal), Expectant (constitutional).
Mnemonic: 📌 "LATE": Low hormones (central), Age (bone age delayed), Turner's/Klinefelter's (gonadal), Expectant (constitutional).
Diagnostic Algorithm - Pubertal Puzzles Solved
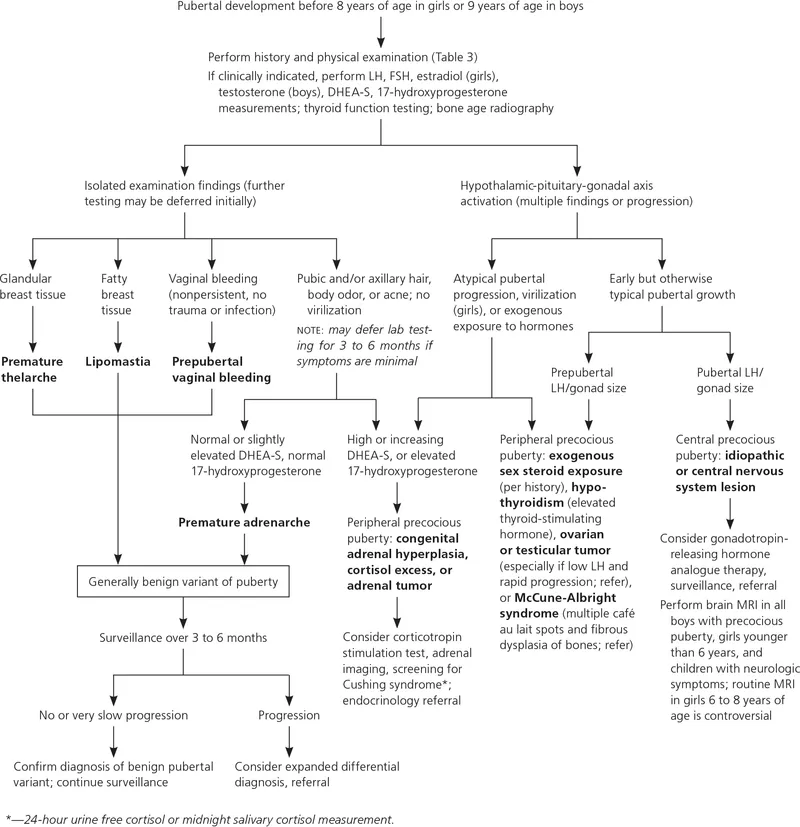
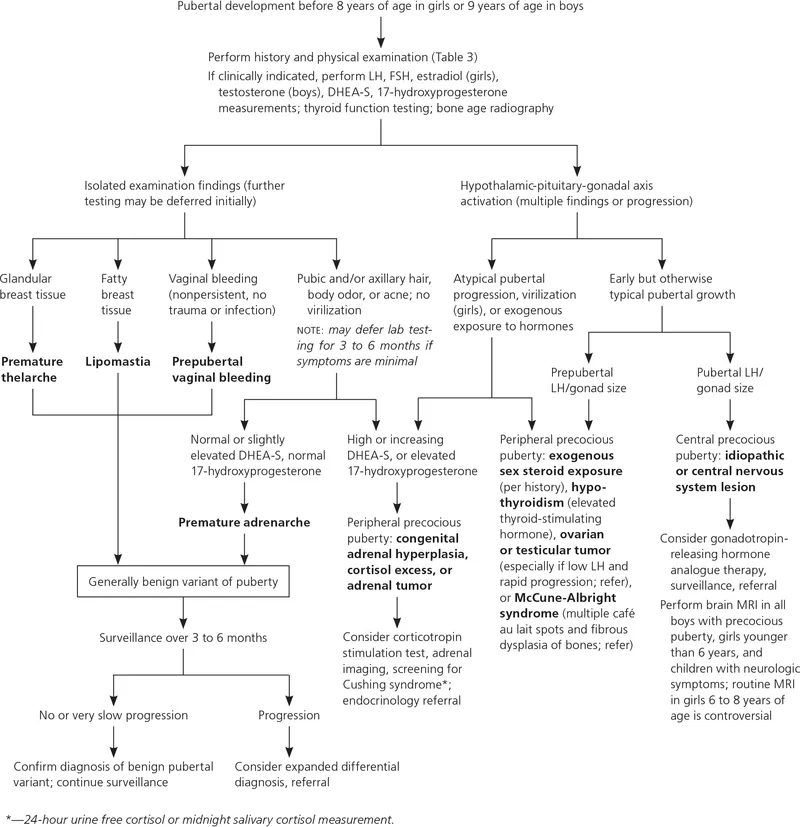
- Precocious Puberty (PP): Girls <8 yrs, Boys <9 yrs. Central (↑LH, GnRH-dependent) vs Peripheral (↓LH, GnRH-independent).
- Delayed Puberty (DP): Girls >13 yrs (no thelarche), Boys >14 yrs (testes <4ml). Hypo-gonadotropic (↓LH/FSH, e.g. CDGP) vs Hyper-gonadotropic (↑LH/FSH, e.g. Turner's).
⭐ CDGP: bone age delayed, matches height age.
High‑Yield Points - ⚡ Biggest Takeaways
- Precocious Puberty: Girls < 8 yrs, Boys < 9 yrs. Central (GnRH-dependent) is most common; treat with GnRH agonists.
- Peripheral Precocious Puberty: GnRH-independent. Key causes: CAH, gonadal tumors, McCune-Albright syndrome.
- Delayed Puberty: Girls > 13 yrs (no breast development), Boys > 14 yrs (no testicular enlargement).
- Constitutional Delay (CDGP): Most frequent cause of delayed puberty; characterized by delayed bone age.
- Kallmann Syndrome: Hypogonadotropic hypogonadism with anosmia. Differentiate from hypergonadotropic causes (e.g., Turner's, Klinefelter's).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

