Celiac Basics - Gluten's Gut Grudge
- Chronic small intestinal immune-mediated enteropathy triggered by dietary gluten.
- Genetic Susceptibility: Primarily HLA-DQ2 (90-95%) and HLA-DQ8 (5-10%).
- Trigger: Gluten (gliadin protein) in Wheat, Rye, Barley. (📌 Mnemonic: Avoid B.R.O.W. - Barley, Rye, Oats*, Wheat. *Oats often contaminated).
- Pathophysiology:
- Ingested gluten (gliadin) is deamidated by tissue transglutaminase (tTG).
- Deamidated gliadin presented by APCs (via HLA-DQ2/DQ8) to CD4+ T-cells.
- Leads to mucosal inflammation: villous atrophy, crypt hyperplasia, ↑Intraepithelial Lymphocytes (IELs).

⭐ Strongest genetic association is with HLA-DQ2.5.
Symptom Spectrum - The Celiac Chameleon
- Gastrointestinal (GI) - Common in younger children:
- Chronic diarrhea (steatorrhea: pale, foul, bulky stools)
- Failure to Thrive (FTT), weight loss
- Abdominal distension, pain, bloating
- Vomiting, anorexia
- Constipation (less common, may occur in older children)
- Extra-intestinal Manifestations (EIMs) - "The Chameleon", esp. older children/adolescents:
- Iron Deficiency Anemia (IDA) - often refractory to oral iron
- Short stature, delayed puberty
- Dermatitis Herpetiformis (DH) - intensely itchy vesicles (elbows, knees, buttocks)
- Dental enamel defects (permanent dentition)
- Recurrent aphthous stomatitis
- Osteopenia/Osteoporosis, arthralgia
- Elevated transaminases (unexplained)
- Silent/Latent Celiac Disease:
- Asymptomatic or minimal symptoms despite positive serology/histology.
⭐ Dermatitis herpetiformis is a highly specific skin manifestation; biopsy of unaffected perilesional skin shows granular IgA deposits at the dermoepidermal junction.

Diagnostic Drill‑Down - Confirming Celiac
- Initial Serology (on gluten diet):
- IgA anti-tissue Transglutaminase (IgA-tTG) - preferred.
- Total IgA (rule out IgA deficiency).
- If IgA deficient: IgG-tTG, IgG-Deamidated Gliadin Peptide (DGP).
- ESPGHAN Guidelines (2020) - Symptomatic Children:
- IgA-tTG > 10x ULN: Confirm with IgA Endomysial Antibody (EMA) (2nd sample).
- If both positive + HLA-DQ2/DQ8 positive (supportive) → Diagnosis without biopsy.
- IgA-tTG < 10x ULN or EMA negative → Duodenal biopsy.
- IgA-tTG > 10x ULN: Confirm with IgA Endomysial Antibody (EMA) (2nd sample).
- Duodenal Biopsy:
- Gold standard; multiple samples (D2/D3, bulb).
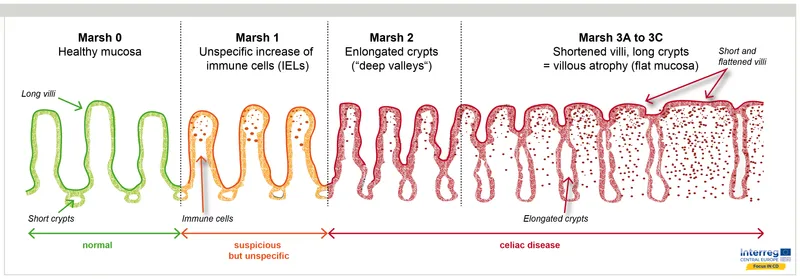
- Histopathology: Marsh-Oberhuber Classification.
- Marsh 0: Normal.
- Marsh I: ↑IELs (>25/100 enterocytes).
- Marsh II: Crypt hyperplasia.
- Marsh III (a,b,c): Villous atrophy (mild, marked, total).
⭐ Marsh IIIc (total villous atrophy) is classic in symptomatic celiac disease.
- Genetic Testing:
- HLA-DQ2/DQ8: High negative predictive value (rules out if negative).
- HLA-DQ2/DQ8: High negative predictive value (rules out if negative).
Treatment & Troubles - Gluten‑Free & Beyond
- Gluten-Free Diet (GFD): Cornerstone
- Lifelong, strict: No Wheat, Rye, Barley, Oats (📌 WRBO: We Read Big Outs).
- Safe: Rice, Corn, Millets, Soya, Potato.
- Beware: Hidden gluten (processed foods, meds). Dietician vital.
- Nutritional Support:
- Correct deficiencies: Fe, Folate, B12, Vit D, Ca, Zn.
- Lactose intolerance: Often transient.
- Monitoring & Follow-up:
- Clinical improvement: Weeks.
- Serology (tTG-IgA): Normalizes in 6-12 months.
- Assess growth & GFD adherence.
- Troubles & Associations:
- Persistent symptoms: Poor GFD adherence commonest.
⭐ Poor GFD adherence: #1 cause of non-response.
- Refractory Celiac Disease (RCD): Rare.
- Long-term risks: Osteoporosis, anemia, infertility, malignancy (EATL), autoimmune (T1DM, thyroiditis).
- Vaccination: Pneumococcal (due to hyposplenism risk).

- Persistent symptoms: Poor GFD adherence commonest.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac disease: Immune reaction to gluten in genetically susceptible individuals (HLA-DQ2/DQ8).
- Presents with chronic diarrhea, malabsorption, weight loss, or anemia; failure to thrive in children.
- Dermatitis herpetiformis is a highly specific skin manifestation.
- Serology: IgA anti-tTG is the preferred initial test; IgA EMA for confirmation.
- Duodenal biopsy showing villous atrophy, crypt hyperplasia, and ↑IELs is diagnostic.
- Lifelong strict gluten-free diet (GFD) is the only treatment.
- Untreated: ↑ risk of lymphoma (e.g., EATL).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

