Clinical Assessment - Heart's First Clues
- History:
- Feeding: Sweating, fatigue, ↓intake, poor weight gain (FTT).
- Cyanosis: Onset, squatting. Exercise intolerance.
- Maternal: Diabetes, infections. Family Hx of CHD.
- General Exam:
- Syndromic facies (e.g., Down's, Turner's, Noonan's).
- Vitals: HR, RR, 4-limb BP (coarctation), SpO2 (pre & post-ductal).
- Clubbing, cyanosis (central/peripheral), edema.
- CVS Exam:
- Palpation: Apex beat (location), thrills, heaves. Pulses: Radio-femoral delay.
- Auscultation: Heart sounds (S1, S2 splitting, S3, S4, clicks). Murmurs: Systolic/Diastolic, Grade (1-6), location, radiation, quality.

⭐ Differential cyanosis (lower limb SpO2 < upper limb SpO2 by >3-5%) strongly suggests Persistent Ductus Arteriosus (PDA) with right-to-left shunt or interrupted aortic arch.
Chest X-Ray - X-Ray Vision
- CT Ratio: Neonate <0.6; Infant (<1yr) <0.55; Child (>1yr) <0.5.
- Pulmonary Vascular Markings (PVM):
- ↑ Plethora: L→R shunts (VSD, ASD, PDA).
- ↓ Oligemia: ↓ Pulm. Blood Flow (TOF, Pulm. Atresia).
- Venous Congestion: LV failure, MS.
- Classic Cardiac Silhouettes & Signs:
- "Boot-shaped": TOF.
- "Egg-on-string": TGA.
- "Snowman sign" / "Figure of 8": TAPVC (supracardiac).
- "Box-shaped" / "Wall-to-wall": Ebstein anomaly.
- Rib notching: Coarctation of Aorta.
⭐ "Boot-shaped" heart (Coeur en sabot) in Tetralogy of Fallot signifies RV hypertrophy & upturned cardiac apex.
Pediatric ECG - Electric Heartbeats
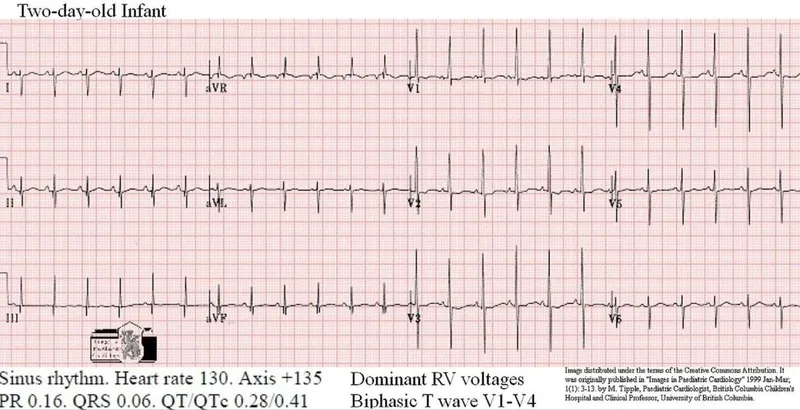
- Key Differences vs. Adult ECG:
- Rate: Faster (Neonate 100-180 bpm, ↓ with age).
- Rhythm: Sinus arrhythmia common.
- Axis: Right axis deviation (RAD) normal in neonates (+90° to +180°), shifts left with age.
- Intervals (PR, QRS): Shorter, ↑ with age. QTc normal <0.44s (<0.46s infants <1yr).
- T waves: Inverted in V1-V3 (juvenile pattern) after 1st week until adolescence.
- RV Dominance: Prominent R in V1, S in V6 in newborns; LV dominance by ~3 yrs.
⭐ Upright T wave in V1 beyond the first week of life (up to ~6 years) or a qR pattern in V1 can suggest Right Ventricular Hypertrophy (RVH).
Echocardiography - Ultrasound Insights
- Non-invasive gold standard for cardiac structure, function, hemodynamics.
- Modes:
- 2D: Real-time anatomical views, chamber dimensions (e.g., LA/Ao ratio), wall motion, pericardial effusion.
- M-mode: Precise measurements of wall thickness, chamber size, LVEF (e.g., Teichholz, Simpson).
- Doppler: Assesses blood flow direction, velocity, turbulence.
- Color Doppler: Visualizes shunts (VSD, ASD), valvular regurgitation.
- Pulsed Wave (PW): Measures velocity at specific points (e.g., E/A ratio for diastolic function).
- Continuous Wave (CW): Measures high velocities (e.g., aortic stenosis peak gradient).
- Applications: Congenital heart defects (CHD), valvular heart disease, cardiomyopathies, infective endocarditis, pulmonary hypertension.
- Transthoracic (TTE) is standard; Transesophageal (TEE) for superior views of posterior structures, LA appendage, prosthetic valves.

⭐ In Tetralogy of Fallot, echocardiography demonstrates an overriding aorta, VSD, RVH, and pulmonary stenosis; Doppler quantifies the PS gradient and shunt.
Advanced Diagnostics - Deeper Dives
-
Cardiac MRI (CMR): Gold standard: RV assessment (volume, function), fibrosis (LGE). For complex anatomy, ARVD, myocarditis. No radiation.
-
Cardiac CT (CCT): Coronary/vascular ring assessment, airway compression. Rapid. Radiation.
-
Cardiac Catheterization: Measures pressures, $O_2$ sats ($Q_p/Q_s$), angiography. Therapeutic: device closures, valvuloplasty.
⭐ Oxygen step-up >7% (SVC/IVC to PA) suggests ASD; >5% (RV to PA) suggests VSD.
-
EPS: Arrhythmia evaluation/ablation.
-
Genetic Testing: Syndromic CHDs, inherited arrhythmia/cardiomyopathy_._
High‑Yield Points - ⚡ Biggest Takeaways
- VSD is the most common CHD; ASD often shows RAD on ECG.
- Echocardiography is the gold standard for CHD diagnosis.
- TOF features: "boot-shaped" heart (CXR), RVH (ECG), cyanosis.
- PGE1 maintains ductal patency in duct-dependent lesions (e.g., TGA, severe PS).
- TGA shows "egg-on-string" (CXR); TAPVC (supracardiac) shows "snowman sign".
- Pulse oximetry screening is vital for detecting critical CHDs in newborns.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

