Renal Development - Blueprint Basics
- Kidney development stages: 📌 Primary Model Matures
- Pronephros: Wk 4, transient.
- Mesonephros: Wk 4-8, interim; part of male genital tract.
- Metanephros: Wk 5+, forms permanent kidney.
- Metanephros arises from:
- Ureteric bud (derived from mesonephric duct) → Forms collecting system (ureter, pelvis, calyces, collecting ducts).
- Metanephric blastema (mesenchyme) → Forms nephrons (glomerulus to DCT).
- Reciprocal induction between ureteric bud and metanephric blastema is essential.
- Key congenital anomaly mechanisms: Failure of induction, abnormal differentiation.

⭐ Ureteric bud (a mesonephric duct derivative) and metanephric blastema interaction is critical for normal kidney formation; defects lead to anomalies like renal agenesis or dysplasia.
Number & Position Anomalies - Hide & Seek Kidneys
-
Renal Agenesis: Absence of kidney tissue.
- Unilateral: Asymptomatic; compensatory hypertrophy of other kidney.
- Bilateral: Fatal; leads to Potter sequence.
- 📌 POTTER: Pulmonary hypoplasia, Oligohydramnios, Twisted face (Potter facies), Twisted skin, Extremity defects, Renal agenesis.
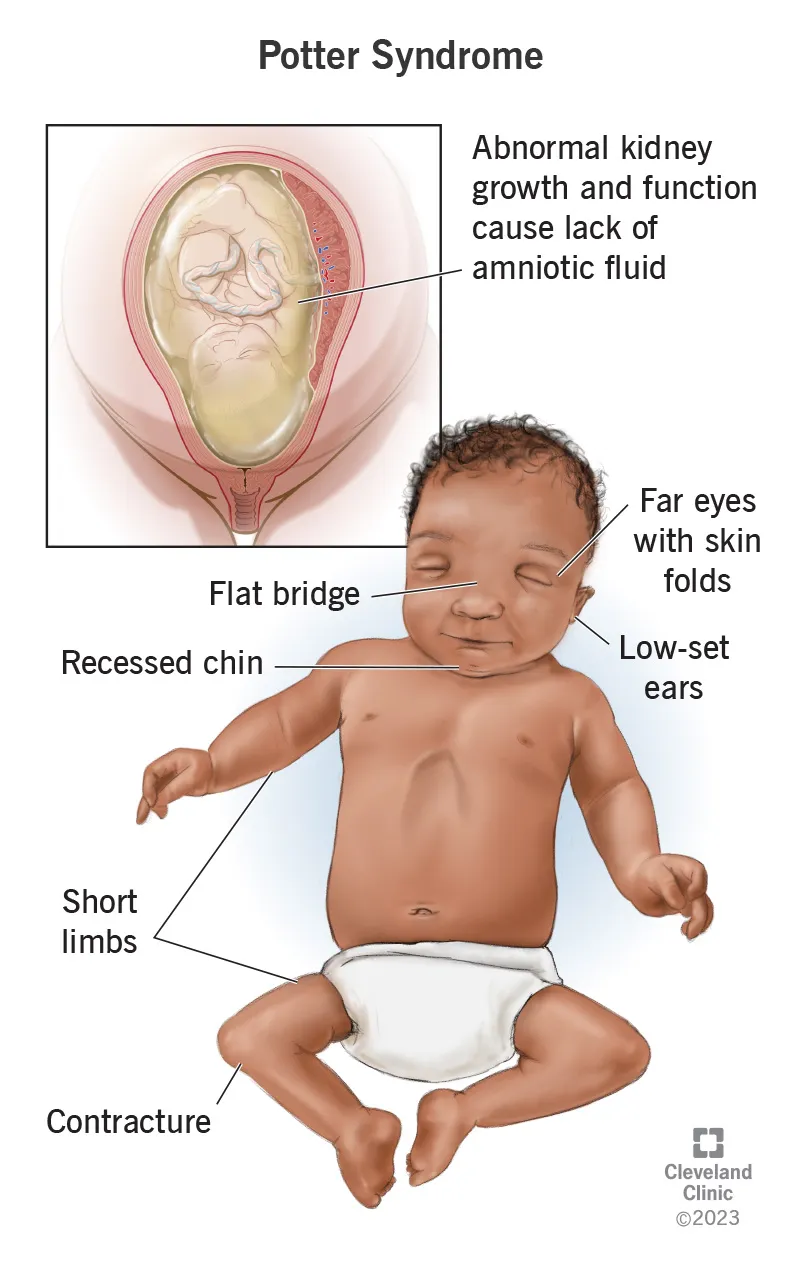
- 📌 POTTER: Pulmonary hypoplasia, Oligohydramnios, Twisted face (Potter facies), Twisted skin, Extremity defects, Renal agenesis.
-
Renal Hypoplasia: Small kidney, ↓ nephrons (developmental).
- True: Congenital, fewer nephrons.
- Acquired: Due to later insults (vascular, infection, obstruction).
-
Ectopic Kidneys: Abnormal kidney position.
- Sites: Pelvic (commonest), iliac, thoracic.
- ↑ Risk: Obstruction, UTIs, stones.
-
Horseshoe Kidney: Fusion at lower poles (usually 90%), across midline.
- Trapped by Inferior Mesenteric Artery (IMA) during ascent.

- Associations: Turner syndrome, other aneuploidies.
- Complications: Hydronephrosis, stones, ↑ risk Wilms tumor, RCC.
⭐ Horseshoe kidney: most common renal fusion anomaly.
- Trapped by Inferior Mesenteric Artery (IMA) during ascent.
Structural & Form Anomalies - Mis-Shapen Kidneys
-
Renal Dysplasia:
- Disorganized renal parenchyma; abnormal differentiation.
- Key histology: Primitive ducts surrounded by undifferentiated mesenchyme, +/- cartilage.

-
Multicystic Dysplastic Kidney (MCDK):
- Extreme form of dysplasia; non-hereditary, usually unilateral.
- Non-functional, appears as grape-like cysts.
- Often involutes.

⭐ MCDK is a common cause of an abdominal mass in newborns.
-
Duplication Anomalies: Results from premature division of the ureteric bud.
- Complete: 2 pelvicalyceal systems, 2 ureters.
- Incomplete: Partial division.
- 📌 Weigert-Meyer Rule (for complete duplication):
- Upper pole ureter: Ectopic, inferomedial insertion; often obstructed (ureterocele).
- Lower pole ureter: Orthotopic insertion; prone to Vesicoureteral Reflux (VUR).
-
Associated Complications:
- Vesicoureteral Reflux (VUR).
- Ureteropelvic Junction (UPJ) / Vesicoureteral Junction (VUJ) obstruction.
- Recurrent Urinary Tract Infections (UTIs).
Congenital Cystic Diseases - Bubble Trouble Kidneys
- Autosomal Recessive Polycystic Kidney Disease (ARPKD)
- Gene: PKHD1 (fibrocystin).
- Onset: Infantile.
- Kidneys: Bilateral, symmetrically enlarged; numerous small cysts (dilated collecting ducts, radial).

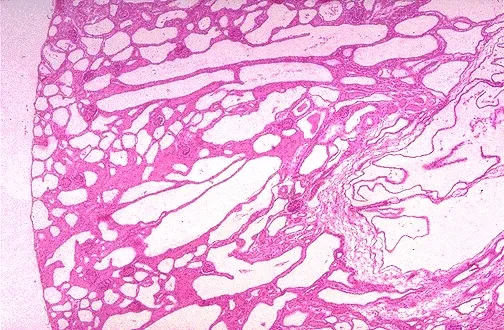
- Associations: Congenital hepatic fibrosis, Caroli syndrome.
⭐ ARPKD kidneys show a "sponge-like" appearance due to diffuse, small cysts.
- Autosomal Dominant Polycystic Kidney Disease (ADPKD)
- Genes: PKD1 (85%), PKD2 (15%).
- Onset: Typically adult; cysts develop over time.
- Medullary Sponge Kidney (MSK)
- Pathology: Cystic dilation of collecting ducts in medullary pyramids.

- Presentation: Often asymptomatic; may have hematuria, stones, UTIs in adults.
- Pathology: Cystic dilation of collecting ducts in medullary pyramids.
- Nephronophthisis Complex (NPH)
- Inheritance: Autosomal recessive (NPHP genes).
- Impact: Most common genetic cause of End-Stage Renal Disease (ESRD) in children/young adults.
- Features: Cysts at corticomedullary junction, tubulointerstitial fibrosis, polyuria, polydipsia.
High-Yield Points - ⚡ Biggest Takeaways
- Bilateral renal agenesis causes Potter sequence (oligohydramnios, pulmonary hypoplasia).
- Horseshoe kidney: Fused lower poles, trapped by IMA; ↑ risk of UPJ obstruction, stones, Wilms tumor.
- ADPKD (PKD1/PKD2 genes): Bilateral cysts, hypertension, berry aneurysms, liver cysts.
- ARPKD (PKHD1 gene): Infancy onset, renal failure, hepatic fibrosis, Potter sequence.
- Multicystic dysplastic kidney (MCDK): Unilateral, non-hereditary, often involutes; non-functional.
- UPJ obstruction: Most common cause of pediatric hydronephrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

