Indications & Pre-Tx Eval - Liver Lifeline Launch
- Indications:
- Acute Liver Failure (ALF): e.g., viral, drug-induced.
- Chronic Liver Disease (CLD): Decompensated (ascites, varices, encephalopathy); MELD > 15.
- Hepatocellular Carcinoma (HCC): Within Milan Criteria.
- Metabolic: Wilson's, A1AT deficiency.
- Cholestatic (end-stage): PSC, PBC.
- Pre-Tx Evaluation:
- Severity: MELD/PELD score.
- 📌 MELD: Bilirubin, Creatinine, INR.
- HCC Staging: Milan Criteria (1 lesion ≤5cm; or ≤3 lesions, each ≤3cm; no major vascular/extrahepatic spread).
- Contraindications: Active sepsis/extrahepatic malignancy, severe cardiorespiratory disease, active substance abuse.
- Workup: Cardiac, pulmonary, renal, infectious, psychosocial.
- Severity: MELD/PELD score.
⭐ MELD score (Bilirubin, Creatinine, INR) is key to predict 3-month mortality in cirrhosis & prioritize transplant.

Graft Types & Immunosuppression - Organ Offers & Immune Ops
-
Graft Types:
- Deceased Donor (DDLT): Whole, split, reduced-size.
- Living Donor (LDLT): Right lobe (adults), left lateral (children).
-
Immunosuppression:
- Phases: Induction, Maintenance, Rejection treatment.
- Key Drugs:
Class Drugs MoA (Key) Key SE (Path) CNIs Tacrolimus, Cyclosporine ↓IL-2, ↓T-cell act. Nephro/Neurotoxicity Antimetabolites MMF, AZA ↓Lymph. prolif. BM suppression, GI (MMF) mTOR inh. Sirolimus, Everolimus Block IL-2 signal, ↓T prolif Delayed healing, Ulcers Steroids Prednisone Broad anti-inflam. Hyperglycemia, ↑Infection
-
Immune Ops: ABO compatibility essential. HLA matching beneficial. Crossmatch vital.
⭐ Tacrolimus, a common calcineurin inhibitor, is notorious for causing nephrotoxicity and neurotoxicity.
Rejection Pathology - Graft's Immune Gauntlet
| Type | Timing | Mechanism | Key Histo Features | Key Banff (ACR: V,B,E) |
|---|---|---|---|---|
| Hyperacute | Mins-hrs | Pre-formed Ab (ABO) | Thrombosis, fibrinoid necrosis, PMNs | N/A |
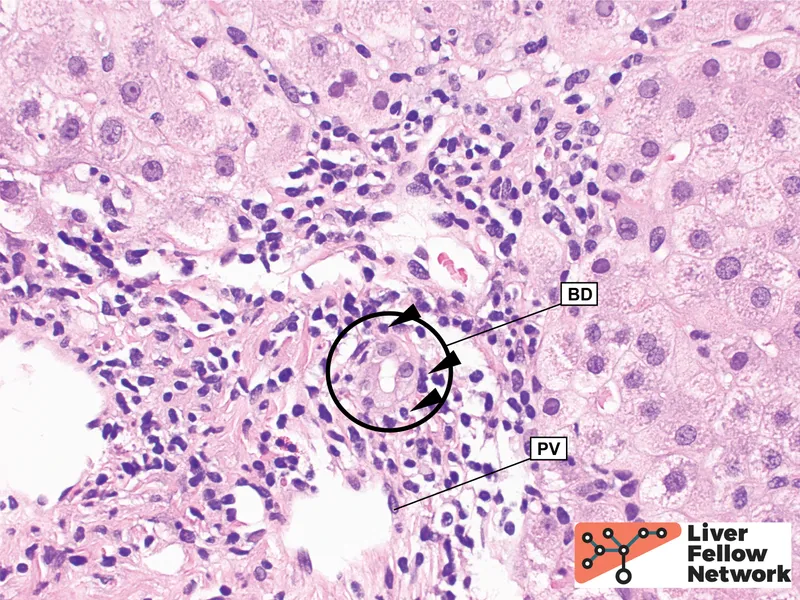
| ACR | Days-wks (<3mo) | T-cell mediated | Venous endotheliitis (V), Bile duct damage (B), Portal inflammation (E) | V,B,E criteria met |
| AMR | Days-wks (late) | DSA (anti-HLA), C4d+ | Capillaritis, C4d deposition, microvascular inflammation (MVI) | C4d+, MVI, DSA+ |
| Chronic | Months-yrs | Mixed; fibrosis | Vanishing bile duct syndrome (VBDS), obliterative arteriopathy | Ductopenia, fibrosis |
⭐ Classic ACR triad (Banff V,B,E criteria): Venous endothelialitis (V), Bile duct injury (B), and Portal inflammation (E). At least two components usually needed for diagnosis.
Non-Rejection Complications - Post-Op Perils & Pathogens
- Vascular: Hepatic Artery Thrombosis (HAT) (early, common), Portal Vein Thrombosis (PVT).
- Biliary: Leaks (early), Strictures (anastomotic/ischemic, later).
- Infections: See table & timeline. Key examples:
-
CMV: "Owl's eye" inclusions.
-
EBV (PTLD): Atypical lymphoid infiltrates.
-
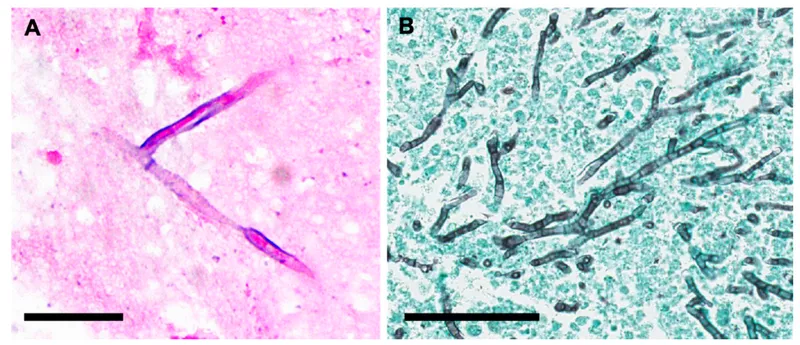
Aspergillus: Angioinvasion, septate hyphae.
-
- Disease Recurrence: HCV, HBV, HCC, PSC.
- Drug Toxicity: CNI nephrotoxicity.
⭐ HAT: most common vascular issue, risks graft loss. CMV: key opportunistic pathogen (1-6 mo).
Common Post-Transplant Infections
| Pathogen | Timing | Key Pathology |
|---|---|---|
| Bacteria | <1 mo | Abscesses, cholangitis |
| Candida spp. | <1 mo | Microabscesses |
| CMV | 1-6 mo | "Owl's eye" inclusions, hepatitis |
| EBV (PTLD) | 1-6 mo+ | Atypical lymphoid infiltrates |
| Aspergillus spp. | 1-6 mo | Angioinvasion, necrosis |
High-Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection: Minutes-hours, preformed anti-donor antibodies (ABO/HLA), irreversible graft damage.
- Acute cellular rejection (ACR): Most common (days-weeks), T-cell mediated; triad: endotheliitis, bile duct injury, eosinophils. Responds to immunosuppression.
- Chronic rejection: Months-years, ductopenic (vanishing bile duct syndrome) or vascular (obliterative arteriopathy), leads to graft loss.
- PTLD: EBV-driven B-cell proliferation; risk with high immunosuppression.
- Recurrence of primary disease (HCV, HCC) is a major concern.
- Opportunistic infections (CMV, fungal) are key complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

