Overview of Tissue Repair - Healing's ABCs
- Goal: Restore tissue structure & function post-injury.
- Two Paths:
- Regeneration: Complete replacement by original cells; no scar.
- Repair (Scarring): Fibrous tissue fills defect if regeneration fails.
- Cell Proliferative Potential:
- Labile: Always cycling (e.g., skin, gut, marrow).
- Stable: Quiescent (G0), can divide (e.g., liver, kidney).
- Permanent: No significant regeneration (e.g., neurons, cardiac muscle).
- Outcome: Depends on injury severity & tissue's regenerative capacity.
⭐ Cardiac muscle, being composed of permanent cells, typically heals by fibrosis (scar formation) after an infarction, not by regeneration of myocytes.
Repair Mechanisms & Angiogenesis - New Pipes & Scaffolds
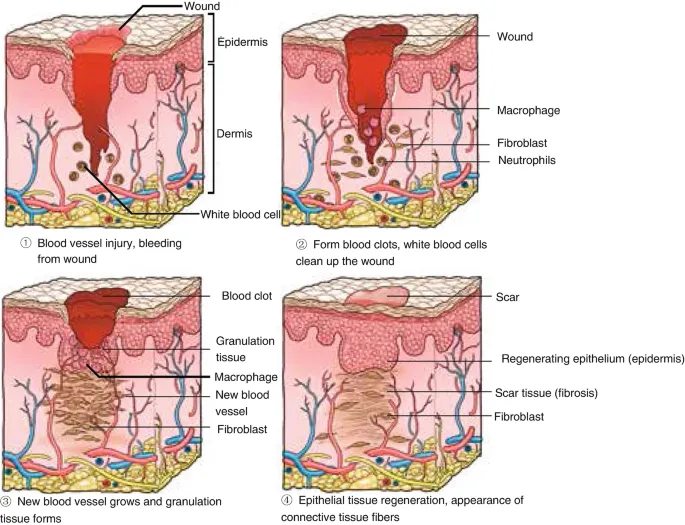
- Repair Phases:
- Inflammation: Clears debris, initiates repair.
- Proliferation: Granulation tissue formation, angiogenesis, re-epithelialization.
- Remodeling: ECM deposition, scar maturation.
- Granulation Tissue: Hallmark of healing.
- Fibroblasts (collagen synthesis).
- New thin-walled capillaries (angiogenesis).
- Loose ECM.
- Inflammatory cells (macrophages).
- Angiogenesis (New Vessel Formation):
- Key growth factors: VEGF, FGF-2.
- Steps: Vasodilation & ↑permeability → Proteolytic degradation of BM → Endothelial cell migration & proliferation → Tube formation → Maturation.

⭐ VEGF (Vascular Endothelial Growth Factor) is the most important growth factor in angiogenesis, stimulated by hypoxia via HIF-1α.
- ECM Deposition & Remodeling:
- TGF-β: Potent fibrogenic agent; stimulates collagen, fibronectin, proteoglycan synthesis.
- MMPs (Matrix Metalloproteinases): Degrade ECM, crucial for remodeling. Balanced by TIMPs (Tissue Inhibitors of Metalloproteinases).
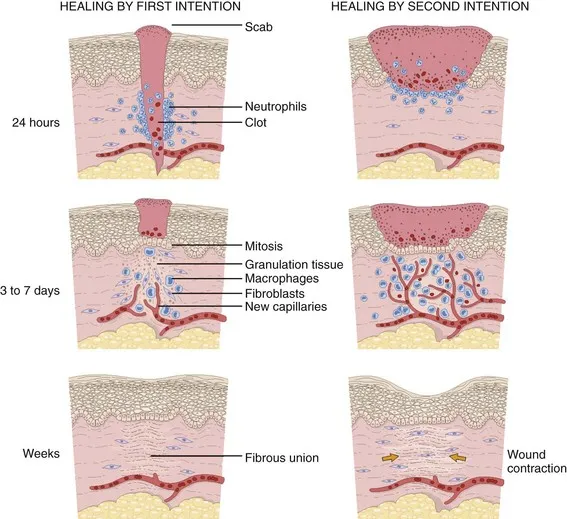
Wound Healing & Scars - Skin's Patchwork
- First Intention (Primary Union): Clean, incised, apposed edges (e.g., surgical). Minimal granulation, fibrin clot, rapid re-epithelialization, less scarring.
- Second Intention (Secondary Union): Large defects, infected wounds, ulcers. More intense inflammation, abundant granulation tissue, significant wound contraction (myofibroblasts), larger, more prominent scar.
- Phases of Healing:
- Scar Strength: Reaches ~70-80% of normal skin by 3 months; Type I collagen dominates.
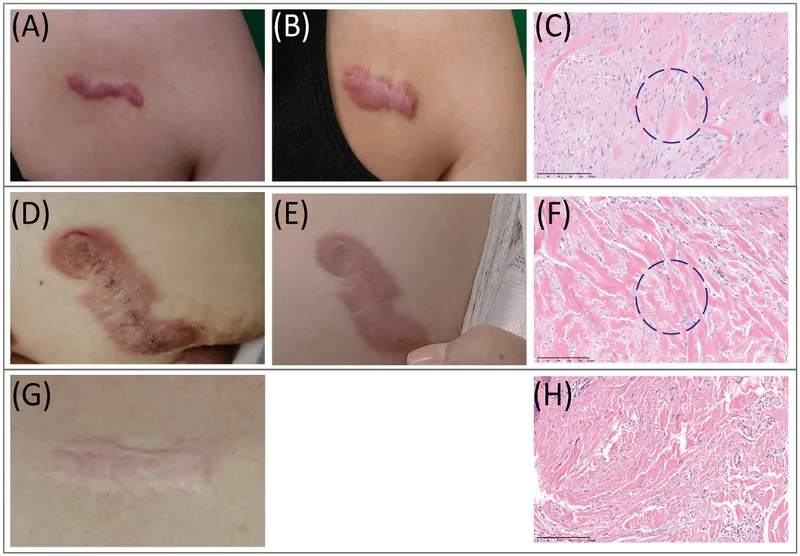
⭐ Hypertrophic scars remain within wound boundaries; Keloids (📌 KEEPS growing) extend beyond, are often familial, more common in darker skin, and rich in Type III collagen.
Pathologic Fibrosis - Scars Gone Wild
Aberrant wound healing: excessive collagen & ECM deposition leading to tissue scarring and organ dysfunction. Caused by chronic inflammation or persistent injury.
- Key Cell: Myofibroblast (activated fibroblast) - primary collagen producer.
- Key Mediator: TGF-β (Transforming Growth Factor-beta) - most potent fibrogenic cytokine.
- Promotes fibroblast migration, proliferation, & collagen synthesis.
- Inhibits ECM breakdown (↓MMPs, ↑TIMPs).
- Consequences: Organ failure (e.g., cirrhosis, pulmonary fibrosis), constrictures, keloids.
⭐ TGF-β is the principal profibrogenic cytokine, pivotal in fibrosis development across nearly all tissues.
Healing Factors & Flops - Fixer-Uppers & Fails
- Systemic Factors:
- Promote: Nutrition (Vit C, protein, zinc), adequate perfusion.
- Impair: Diabetes, glucocorticoids, poor circulation, advanced age.
- Local Factors:
- Promote: Good blood supply, no infection, immobilization.
- Impair: Infection (major delay!), foreign bodies, ischemia, movement.
- Complications (Flops):
- Deficient Scar: Dehiscence (rupture), ulceration.
- Excessive Scar: Hypertrophic (raised, within borders), Keloid (grows beyond; 📌 Keloid Klimbs).
- Contractures: Limits mobility (e.g., post-burn).
⭐ Keloids show haphazard collagen (Type I & III); common in African descent, earlobes, sternum.
High‑Yield Points - ⚡ Biggest Takeaways
- Granulation tissue formation, with fibroblasts, angiogenesis, and macrophages, is absolutely crucial for repair.
- TGF-β is the most potent fibrogenic cytokine, strongly stimulating collagen production.
- Myofibroblasts are key cells for effective wound contraction.
- Type III collagen (early) is replaced by Type I collagen (late, for strength).
- Keloids and hypertrophic scars result from excessive collagen deposition.
- Infection, diabetes, and steroids are major systemic inhibitors of wound healing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more