Pathogen Entry & Colonization - Gatecrashers & Squatters
- Portals of Entry (Gatecrashing): Microbial access points.
- Mucous Membranes: Resp (TB), GI (Cholera), GU (UTI), Conjunctiva.
- Skin: Parenteral route (cuts, bites).
- Placenta: TORCH (e.g., Rubella, CMV).
- 📌 ID₅₀: Dose for 50% infection; ↓ID₅₀ = ↑virulence.
- Adherence (Sticking On): Crucial binding to host cells.
- Pathogen adhesins (pili, M-protein) bind host receptors.
- Determines tissue tropism (e.g., S. mutans & teeth).
- Colonization (Squatting): Establishing foothold & multiplying.
- Overcoming local defenses (mucus, IgA, normal flora).
- IgA proteases (e.g., N. gonorrhoeae).
- Biofilms: Shielded communities, ↑resistance (e.g., P. aeruginosa in CF lungs, catheters).
- Quorum sensing: Coordinated gene expression.
- Overcoming local defenses (mucus, IgA, normal flora).

⭐ Helicobacter pylori uses urease to neutralize gastric acid (↑pH), allowing it to colonize the stomach lining and cause peptic ulcers.
Pathogen Virulence & Host Damage - Tiny Terrors' Tactics
-
Virulence Factors: Pathogen traits enhancing disease.
- Adhesion: Adhesins, pili, fimbriae aid colonization.
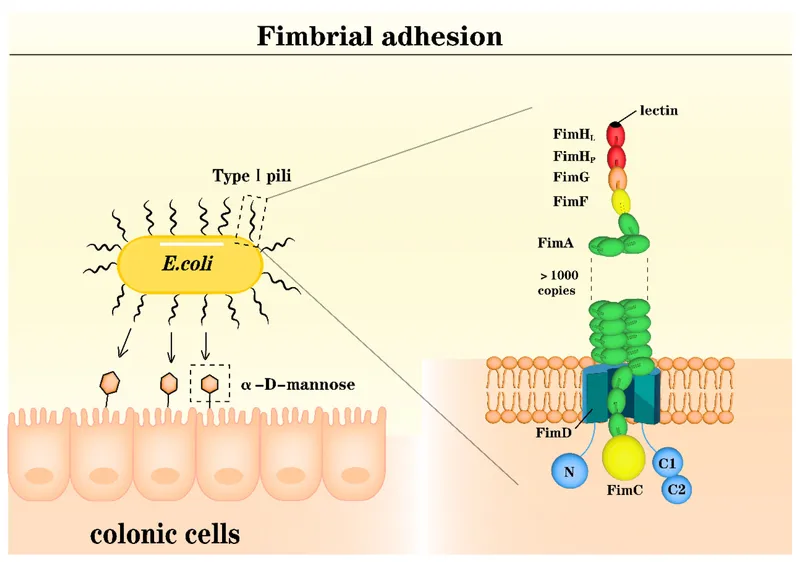
- Invasion: Hyaluronidase, collagenase aid tissue penetration.
- Evasion of Host Defenses:
- Capsules (e.g., S. pneumoniae): Antiphagocytic.
- Antigenic variation (e.g., Influenza, N. gonorrhoeae).
- Biofilms: Protection from drugs & immunity.
- Intracellular survival (e.g., M. tuberculosis).
- Toxin Production:
- Exotoxins: Secreted proteins; potent, specific.
- A-B toxins (Cholera, Diphtheria).
- Membrane-disrupting (Hemolysins).
- Superantigens (TSST-1, Toxic Shock).
- Endotoxins: Lipopolysaccharide ($LPS$) (Gram-negative outer membrane). Released on lysis.
⭐ LPS (Endotoxin), a PAMP, binds TLR4, releases TNF-α, IL-1, and IL-6, leading to fever, septic shock, and DIC.
- Exotoxins: Secreted proteins; potent, specific.
- Adhesion: Adhesins, pili, fimbriae aid colonization.
-
Host Damage Mechanisms:
- Direct Damage: Direct cell lysis, toxin effects.
- Indirect Damage (Immunopathology): Host immune response causes injury.
- Inflammation, cytokine release.
- Hypersensitivity reactions.
- Autoimmunity (molecular mimicry, Rheumatic fever).
Host Immune Response - Body's Border Patrol
- Innate Immunity (Rapid, Non-specific): First line of defense.
- Barriers: Skin, mucous membranes (physical/chemical).
- Cells: Phagocytes (Neutrophils, Macrophages), Natural Killer (NK) cells, Dendritic Cells (DCs).
- Receptors: Pattern Recognition Receptors (PRRs) like Toll-like Receptors (TLRs) detect Pathogen-Associated Molecular Patterns (PAMPs).
- Mediators: Inflammation (Pro-inflammatory cytokines: TNF-α, IL-1, IL-6), Complement system (Opsonization, Membrane Attack Complex - MAC).
- Adaptive Immunity (Specific, Memory): Tailored, potent response with memory.
- Antigen Presentation: Antigen Presenting Cells (APCs - Macrophages, DCs, B cells) process and present antigens.
- MHC-I: On all nucleated cells; presents endogenous antigens to CD8+ T cells.
- MHC-II: On APCs; presents exogenous antigens to CD4+ T cells.
- Cell-Mediated Immunity (CMI):
- CD4+ T Helper (Th) cells: Orchestrate response. Th1 (intracellular pathogens, e.g., IFN-γ release); Th2 (parasites, allergy).
- CD8+ Cytotoxic T Lymphocytes (CTLs): Directly kill infected host cells.
- Humoral Immunity:
- B-lymphocytes differentiate into Plasma cells → produce Antibodies (e.g., IgG, IgM, IgA).
- Antibody functions: Neutralization, opsonization, complement activation.
- Antigen Presentation: Antigen Presenting Cells (APCs - Macrophages, DCs, B cells) process and present antigens.

⭐ IFN-γ, produced by Th1 cells and NK cells, is crucial for macrophage activation and control of intracellular pathogens like Mycobacterium tuberculosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Adherence via adhesins (pili) to host receptors is the crucial first step.
- Invasion occurs via M cells, or zipper/trigger mechanisms; intracellular survival is key for some.
- Exotoxins are specific secreted proteins; Endotoxin (LPS) from Gram-negatives causes septic shock.
- Immune evasion mechanisms include capsules, antigenic variation, and biofilms.
- Host immunodeficiency, genetics (CCR5-HIV), and age significantly impact susceptibility.
- Type III/IV secretion systems inject effector proteins, manipulating host cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

