AMR Basics - Resistance 101
- Antimicrobial Resistance (AMR): A microbe's ability to withstand antimicrobial drugs, rendering treatments ineffective and infections persistent.
- Resistance Categories:
- MDR (Multidrug Resistance): Resistance to at least one agent in ≥3 antimicrobial categories.
- XDR (Extensive Drug Resistance): Resistance to all but ≤2 antimicrobial categories.
- PDR (Pandrug Resistance): Resistance to all agents in all antimicrobial categories.
- Impact & Burden:
- A critical global health security threat.
- Leads to treatment failures, ↑ morbidity, mortality, and economic burden.
- India carries a high burden of AMR.
⭐ Globally, MDR-TB is a major public health crisis, with India having one of the highest burdens of the disease and its drug-resistant forms.
Resistance Tricks - Bugs Fight Back
Bacteria evade antibiotics via:
- Enzymatic Inactivation: e.g., β-lactamases cleave β-lactam drugs.
- Target Site Modification:
- Altered PBPs (e.g., PBP2a in MRSA) $\rightarrow$ ↓ β-lactam binding.
- Altered D-Ala-D-Lac (VanA/VanB in VRE) $\rightarrow$ ↓ vancomycin binding.
- rRNA methylation $\rightarrow$ ↓ macrolide/clindamycin binding.
- Reduced Permeability: Porin loss (Gram-negatives) limits drug entry.
- Active Efflux Pumps: Expel antibiotics from the cell.

Genetic Basis:
- Intrinsic: Natural, inherent resistance.
- Acquired: New resistance via mutation or Horizontal Gene Transfer (HGT).
⭐ The most common mechanism of resistance to β-lactam antibiotics is the production of β-lactamase enzymes, which hydrolyze the β-lactam ring.
Horizontal Gene Transfer (HGT) Mechanisms: 📌 Mnemonic: Cats Try Treats (Conjugation, Transduction, Transformation)
Superbugs Spotlight - Rogues' Gallery
📌 ESKAPE pathogens & others:
| Pathogen | Key Resistance (Gene/Mechanism) | Clinical Impact |
|---|---|---|
| Staphylococcus aureus (MRSA) | mecA | Methicillin-R; SSTI |
| Enterococcus faecium (VRE) | vanA, vanB | Vancomycin-R; UTIs |
| Klebsiella pneumoniae (ESBL/CRE) | CTX-M; NDM-1, KPC, OXA-48 | Carbapenem-R, HAIs |
| Acinetobacter baumannii (MDR) | OXA-carbapenemases | MDR; VAP, HAIs |
| Pseudomonas aeruginosa (MDR) | Metallo-β-lactamases (MBLs) | MDR; HAIs, CF inf. |
| Enterobacter spp. (ESBL/CRE) | CTX-M; NDM-1 | Carbapenem-R, HAIs |
| Mycobacterium tuberculosis (MDR/XDR) | rpoB, katG; +FQ/SLI | Difficult TB, ↑mortality |
Lab Detectives - Finding Foes
- Phenotypic Methods:
- Disk diffusion (Kirby-Bauer): Zone sizes show susceptibility.
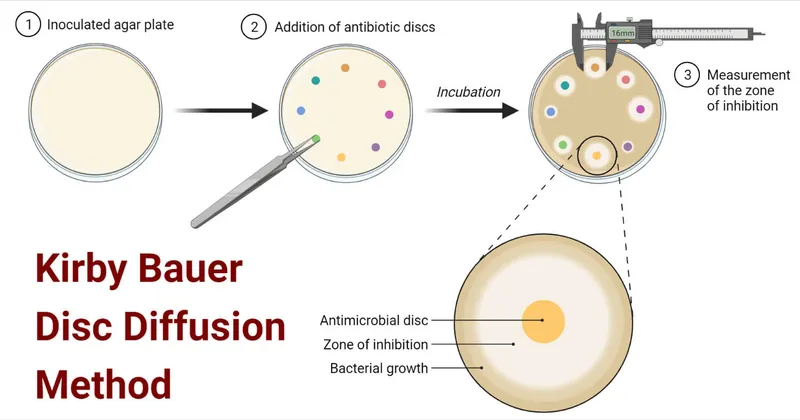
- MIC determination: Broth dilution, E-test (gradient).
- Automated systems (e.g., VITEK).
- Use CLSI/EUCAST breakpoints for interpretation.
- Disk diffusion (Kirby-Bauer): Zone sizes show susceptibility.
- Specific Phenotypic Tests:
- D-test: For inducible clindamycin resistance (📌 D-shape zone).
- MHT/Carba NP test: Detects carbapenemases.
- Genotypic Methods:
- PCR: For resistance genes (e.g., mecA, vanA, blaKPC, blaNDM, blaOXA-48).
- Sequencing: For detailed genetic analysis.
⭐ The D-test is used to detect inducible clindamycin resistance in Staphylococcus aureus strains that appear erythromycin-resistant and clindamycin-susceptible in routine testing.
AMR Counterattack - Our Battle Plan
- Antimicrobial Stewardship Programs (ASP): Optimize antibiotic use, ↓resistance, improve patient outcomes.
⭐ Key elements of Antimicrobial Stewardship Programs include prospective audit with intervention and feedback, and formulary restriction with preauthorization.
- Infection Prevention & Control (IPC): Crucial measures include:
- Additional Strategies: Promote rational drug use, invest in new drug R&D, explore combination therapies, and develop vaccines.
- National Guidance: India's National Action Plan on AMR coordinates national efforts.
High‑Yield Points - ⚡ Biggest Takeaways
- ESBLs confer resistance to penicillins, cephalosporins, monobactams; often plasmid-mediated.
- MRSA due to mecA gene (altered PBP2a) resists most beta-lactams.
- VRE via VanA/VanB genes alters peptidoglycan target (D-Ala-D-Lac) for vancomycin resistance.
- Carbapenemases (e.g., KPC, NDM-1) hydrolyze carbapenems, causing broad beta-lactam resistance.
- MDR-TB signifies resistance to at least isoniazid and rifampicin.
- Key resistance mechanisms: enzymatic inactivation, target site modification, active efflux pumps.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

