IBD: Pathophysiology - Gut's Blood Crisis
Definition: Intestinal ischemia: critical gut injury from severely insufficient blood supply.
-
Etiology:
- Occlusive (vascular blockage):
- Arterial: Embolism (e.g., Atrial Fibrillation - AF), thrombosis (atherosclerosis).
- Venous: Thrombosis (e.g., hypercoagulable states, portal HTN).
- Non-occlusive (low flow states): Shock (cardiogenic, hypovolemic, septic), potent vasopressors.
- Occlusive (vascular blockage):
-
Pathophysiology:
- Hypoxic Injury: Initial damage from $↓O₂$; leads to $↓ATP$, cell swelling, mucosal barrier compromise.
- Reperfusion Injury: Paradoxical exacerbated damage on reperfusion; driven by reactive oxygen species ($↑ROS$), neutrophils, inflammatory mediators.
-
Key Risk Factors:
- Atherosclerosis (major for arterial occlusion)
- Atrial Fibrillation (AF) (key emboli source)
- Shock (all types cause hypoperfusion)
- Vasculitis (e.g., PAN, SLE)
- Hypercoagulable states
- Advanced age, prior abdominal surgery.
⭐ Watershed areas (splenic flexure, rectosigmoid junction) are most vulnerable to ischemia due to limited collateral circulation.
IBD: Morphology - Damage Unveiled
- Spectrum of Infarction (Ischemic Bowel Disease):
- Mucosal: Superficial necrosis, mucosa only; due to hypoperfusion.
- Mural: Necrosis extends into submucosa; from severe hypoperfusion or partial occlusion.
- Transmural: Full-thickness necrosis involving all layers; typically acute arterial occlusion.
- Gross Features:
- Affected segment: Segmental or diffuse; sharply demarcated in arterial occlusion.
- Color: Dusky, cyanotic to purple-red, later hemorrhagic.
- Wall: Edematous, thickened.
- Mucosa: Ulceration, friability, sloughing. Perforation in severe transmural cases.
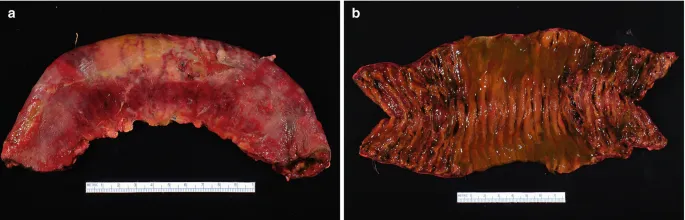
- Microscopic Features:
- Early: Coagulative necrosis, edema, hemorrhage.
- Epithelium: Villous blunting/atrophy, crypt destruction.
- Inflammation: Neutrophils, later chronic inflammation. Pseudomembrane formation.
- Watershed Areas (Most Vulnerable):
- Splenic flexure (Griffiths' point): SMA & IMA junction.
- Rectosigmoid junction (Sudeck's point): IMA & iliac artery supply.
⭐ Transmural infarction often presents with bloody diarrhea and can rapidly progress to sepsis and shock.
IBD: Clinical Syndromes - Gut Attack Scenarios
Vascular compromise leading to intestinal injury. High index of suspicion is key.
- Acute Mesenteric Ischemia (AMI): Life-threatening!
- Causes:
- Arterial embolism (e.g., AFib) / thrombosis (atherosclerosis)
- Non-Occlusive Mesenteric Ischemia (NOMI; low flow states)
- Mesenteric venous thrombosis (hypercoagulable states)
- Sx: Severe, acute abdominal pain "out of proportion" to physical findings.
- Dx: CT Angiography (CTA) is gold standard. ↑Lactate.
- Mortality: High (>50-70%).
- Causes:
- Chronic Mesenteric Ischemia (CMI):
- "Intestinal angina": Postprandial abdominal pain, food fear, weight loss.
- Dx: CTA.
- Ischemic Colitis (IC):
- Most common form of intestinal ischemia.
- Often transient, segmental inflammation (watershed areas).
- Sx: LLQ pain, hematochezia.

⭐ Ischemic colitis most commonly affects watershed areas, particularly the splenic flexure and sigmoid colon.
Other Vascular Lesions - Bleeding Mysteries
- Angiodysplasia:
- Pathogenesis: Acquired; ectatic, thin-walled submucosal vessels.
- Location: Cecum & right colon (most common). 📌 Right side, Right site!
- Associations: Aortic stenosis (Heyde's syndrome), von Willebrand Disease (vWD), End-Stage Renal Disease (ESRD).
- Presentation: Recurrent, painless Lower GI Bleeding (LGIB) (occult or melena).

- Radiation Enterocolitis/Proctitis:
- Cause: Post-pelvic radiation therapy (XRT).
- Path: Chronic ischemia, obliterative endarteritis, submucosal fibrosis, telangiectasias.
- Sx: Rectal bleeding, pain, diarrhea, strictures.
- Necrotizing Enterocolitis (NEC):
- Population: Premature infants, low birth weight.
- Path: Ischemic necrosis (typically terminal ileum/colon); gas in bowel wall (pneumatosis intestinalis).
- Sx: Bloody stools, abdominal distension, feeding intolerance.
⭐ Heyde's syndrome triad: Aortic stenosis, acquired vWD (Type 2A)-like defect, and bleeding from GI angiodysplasia. Bleeding often improves after aortic valve replacement!
High‑Yield Points - ⚡ Biggest Takeaways
- Ischemic bowel disease most commonly affects watershed areas like the splenic flexure and sigmoid colon.
- Acute mesenteric ischemia (AMI) presents with severe abdominal pain out of proportion to clinical findings, often due to arterial embolism.
- Chronic mesenteric ischemia (CMI) is characterized by postprandial abdominal pain ("intestinal angina") and weight loss, typically from atherosclerosis.
- Non-occlusive mesenteric ischemia (NOMI) is seen in critically ill patients, often associated with shock or vasopressor use.
- Colonic ischemia is the most common form of intestinal ischemia; thumbprinting may be seen on imaging.
- Angiodysplasia is a frequent cause of lower GI bleeding in the elderly, commonly found in the cecum and right colon.
- Hemorrhoids are dilated submucosal veins in the anal canal, a common cause of painless rectal bleeding with defecation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

