IBD Overview - Gut Feeling Gone Wrong
- Definition: Chronic, relapsing inflammatory disorders of the gastrointestinal tract (GIT).
- Epidemiology:
- Bimodal age distribution: Peaks at 15-30 years and 50-80 years.
- Rising incidence globally, including a significant increase in India.
- Etiology (Multifactorial):
- Genetic predisposition: Key genes like NOD2/CARD15.
- Immune dysregulation: Aberrant immune response to gut flora.
- Gut microbiota: Dysbiosis, reduced diversity.
- Environmental triggers: Smoking (complex role: ↑Crohn's, ↓UC), diet, NSAIDs, infections.

⭐ The 'hygiene hypothesis' posits that decreased early-life microbial exposure might elevate IBD susceptibility.
Crohn's Disease - Skip & Strike
- Distribution: Any part of GIT ('gum to bum'); terminal ileum, colon typical.
- Pattern: Skip lesions (discontinuous).
- Inflammation: Transmural (full thickness).
- Linear ulcers, cobblestone appearance.
- Creeping fat (mesenteric fat wrapping bowel).
- Complications: Fistulae, strictures, abscesses.
- Microscopy: Non-caseating granulomas (pathognomonic, not always present).
- Pathogenesis: Th1/Th17 mediated immune response.
📌 Mnemonic: 'A Christmas GRANdma SKIPped over FAT COBBLEd WALLS from her MOUTH to her ANUS' (Crohn's, Granulomas, Skip lesions, Fat (creeping), Cobblestone, Transmural, Mouth to Anus involvement).

⭐ Smoking is a significant risk factor for Crohn's disease and worsens its course.
Ulcerative Colitis - Continuous Chaos
- Limited to colon & rectum; continuous inflammation starting from rectum, extends proximally.
- 📌 CLOSEUP: Continuous, Limited to colon/rectum, Only mucosa/submucosa, Smoking protective, Extends proximally, Ulcers (superficial, broad-based), Pseudopolyps/p-ANCA.
- Pathology:
- Gross: Diffuse erythema, friability, pseudopolyps.
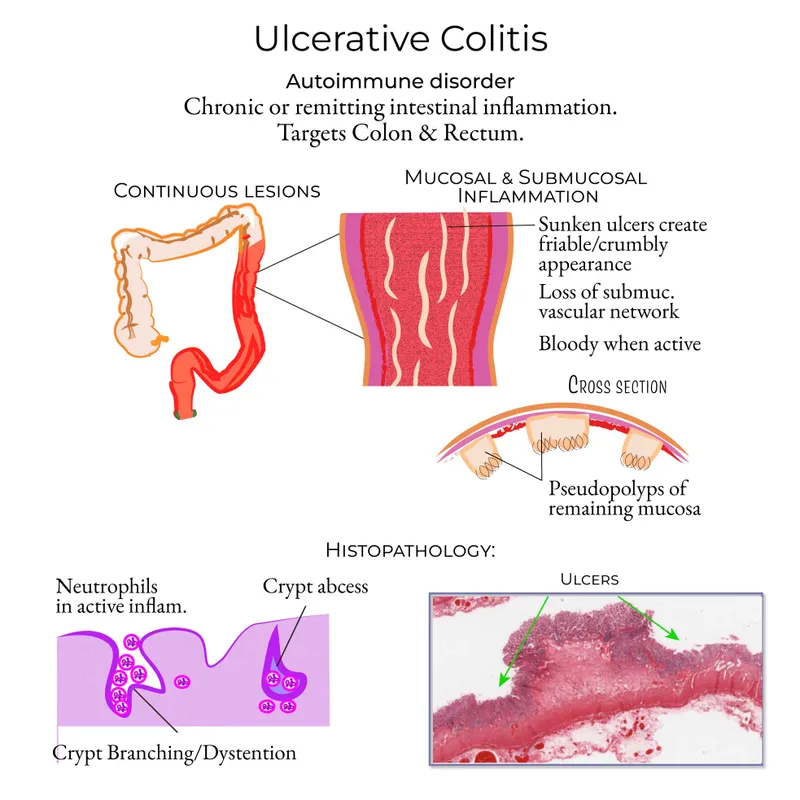
- Micro: Mucosal & submucosal inflammation ONLY; crypt abscesses, crypt distortion, goblet cell depletion.

- Gross: Diffuse erythema, friability, pseudopolyps.
- Immune: Th2 mediated (less clear-cut than CD).
⭐ p-ANCA (perinuclear anti-neutrophil cytoplasmic antibodies) are positive in about 60-70% of Ulcerative Colitis patients.
IBD Comparison & Diagnosis - Telling Them Apart
| Feature | Crohn's Disease (CD) | Ulcerative Colitis (UC) |
|---|---|---|
| Location | Any part of GIT (mouth to anus); skip lesions | Colon only (starts rectum); continuous |
| Gross | Transmural, linear ulcers, cobblestone, strictures | Mucosal/submucosal, pseudopolyps, lead pipe |
| Microscopic | Non-caseating granulomas (50%) | Crypt abscesses, crypt distortion |
| Complications | Fistulas, abscesses, strictures, malabsorption | Toxic megacolon, hemorrhage, ↑ CRC risk |
| Smoking | Worsens CD | Protective for UC |
| Serology | ASCA+ (~60%) | p-ANCA+ (~60%) |
- Imaging: CT/MR Enterography (evaluates extent/complications, esp. CD). Barium studies (less common).
- Stool Studies: Fecal calprotectin (monitors activity).

⭐ While ASCA is more common in Crohn's and p-ANCA in UC, their sensitivity and specificity are not absolute for diagnosis.
Complications & EIMs - Beyond the Bowel
Intestinal Complications:
- Crohn's Disease (CD): Fistulas, Strictures, Abscesses, Malabsorption, Perforation.
- Ulcerative Colitis (UC): Toxic megacolon, Severe hemorrhage, Perforation, ↑ Dysplasia/Colorectal Cancer (CRC) risk (esp. pancolitis >8-10 yrs).
Extra-intestinal Manifestations (EIMs): 📌 Mnemonic: A PIE SAC
- Arthritis (peripheral, ankylosing spondylitis)
- Pyoderma gangrenosum
- Iritis/Uveitis, Episcleritis
- Erythema nodosum
- Sclerosing cholangitis (Primary, strongly assoc. with UC)
- Aphthous stomatitis
- (Other EIMs: Osteoporosis, Clubbing)

⭐ Primary Sclerosing Cholangitis (PSC) is seen in about 5% of UC patients and significantly increases the risk of cholangiocarcinoma and colorectal cancer.
High‑Yield Points - ⚡ Biggest Takeaways
- Crohn's Disease: Transmural inflammation, skip lesions, non-caseating granulomas, cobblestone mucosa. Fistulas and strictures common.
- Ulcerative Colitis: Continuous mucosal/submucosal inflammation starting in rectum. Crypt abscesses, pseudopolyps, and bloody diarrhea are characteristic.
- Key Complications: Crohn's: malabsorption, fistulae. UC: toxic megacolon, significantly ↑ colorectal cancer risk.
- Associations: Crohn's: ASCA positive, smoking worsens. UC: p-ANCA positive, smoking is protective, PSC association.
- Shared Extraintestinal: Both can present with arthritis, uveitis, and erythema nodosum.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

