Navigation & Robotics: Fundamentals - Guiding Stars
- Navigation (CAS): Real-time image-guidance for surgical precision. Acts as a surgical GPS.
- Core Components: Computer workstation, trackers (optical/EM), patient-specific imaging (CT/MRI/fluoro).
- Key Process: Registration (crucial image-to-patient anatomy alignment), then real-time instrument/implant tracking.
- Benefits: ↑Accuracy in placement, ↓radiation exposure, supports MIS.
- Robotics: Robotic systems enhance surgeon's actions, offering superior control.
- Types: Haptic (tactile feedback), active (autonomous tasks), shared-control (collaborative).
- Advantages: ↑Precision, tremor filtration, improved dexterity.

⭐ Registration is the pivotal step in CAS, accurately mapping pre-operative imaging data to the patient's live anatomical position for precise surgical execution.
Orthopaedic Navigation: Systems & Workflow - Digital Eyes
- Core: Real-time tracking of instruments/implants relative to patient anatomy for guided surgery.
- System Types:
- Optical: Infrared cameras track reflective/emitting markers.
- Active: IR-emitting markers (LEDs). Accurate, wired.
- Passive: IR-reflecting markers. Wireless, line-of-sight needed.
- Electromagnetic: Sensors tracked in magnetic fields. No line-of-sight issues; metallic interference.
- CT-based: Pre-op CT for 3D plan; intra-op registration needed.
- Fluoro-based: Uses C-arm images (2D/3D). Real-time; radiation.
- Imageless: Uses digitized landmarks, kinematic data. Less radiation.
- Optical: Infrared cameras track reflective/emitting markers.
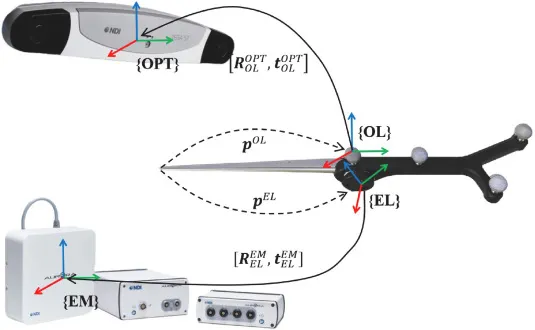
- Typical Workflow:
⭐ Registration accuracy is key for navigation success (errors < 2 mm & < 2°). Links pre-op plans to intra-op reality.
Robotic-Assisted Orthopaedics: Types & Tech - Surgeon's Smart Hand
- Robotic Systems: Enhance surgical precision & accuracy.
- Active: Autonomous execution of pre-planned tasks (e.g., ROBODOC for bone milling). Surgeon supervises.
- Semi-Active (Haptic/Shared-Control): Surgeon-guided with robotic constraints & tactile feedback (e.g., MAKO, NAVIO, ROSA). Most common.
- Passive: Instrument/camera holders; surgeon fully controls actions (advanced navigation aid).
- Core Technology:
- Planning: CT/MRI-based 3D models.
- Registration: Aligning patient anatomy to plan intraoperatively.
- Robotic Arm: Executes tasks or guides surgeon.
- Tracking: Optical/electromagnetic systems for real-time positioning.
⭐ Semi-active robotic systems (e.g., MAKO) in arthroplasty show improved accuracy in implant positioning and limb alignment versus conventional methods.
Clinical Applications & Challenges: Real-World Impact - Precision & Pitfalls
- Precision Benefits (Navigation & Robotics):
- ↑ Accuracy: Implant placement (THA cup, TKA cuts), osteotomies, screw paths.
- ↓ Complications: Reduced malpositioning, neurovascular injury risk.
- ↓ Radiation: Key for spine procedures (surgeon/staff).
- MIS: Facilitates smaller incisions, less tissue trauma.
- Key Clinical Applications:
- Arthroplasty: TKA, THA, UKA - bone cuts, component alignment, leg length.
- Spine: Pedicle screws, cage insertion, deformity.
- Trauma: Pelvic/acetabular #, complex intra-articular #.
- Oncology: Tumor resection, limb salvage.

- Pitfalls & Challenges:
- Cost: High initial & maintenance.
- Learning Curve: Steep; dedicated training needed.
- Operative Time: Can be ↑ initially; registration process.
- Registration Errors: Can propagate, affecting accuracy.
- System Limits: Bulkiness, tech malfunction, ↓ tactile feedback (robotics).
⭐ Robotic-assisted TKA aims for mechanical axis alignment within ±3°, showing improved accuracy over conventional methods.
High‑Yield Points - ⚡ Biggest Takeaways
- Navigation (CAS) improves implant accuracy in THR (acetabular cup) & TKR (femoral/tibial cuts).
- Imageless navigation avoids radiation exposure unlike CT-based systems, reducing patient risk.
- Robotic surgery offers sub-millimeter precision and aims for reproducible results.
- Registration (e.g., point-based, surface mapping) is crucial for matching patient anatomy to the surgical plan.
- Haptic feedback in many robotic systems guides surgeons, preventing excessive bone resection.
- Potential benefits include reduced malalignment, improved joint kinematics, and potentially better long-term implant survivorship.
- Key challenges include high initial cost, a steep learning curve, and potential for longer initial operative times.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

