Fragility Fractures - Defining the Snap
- Fractures resulting from low-energy trauma (e.g., fall from standing height or less), indicating compromised bone strength.
- Strongly associated with osteoporosis; may be the first sign.
- Common sites: Vertebrae (compression), hip (femoral neck), distal radius (Colles'), proximal humerus.
- Epidemiology: Incidence ↑ with age, particularly in postmenopausal women and men >50 years.
- Impact: Significant pain, disability, ↓ quality of life, ↑ mortality risk, and substantial healthcare costs.
⭐ A fragility fracture is defined by the WHO as a fracture caused by injury that would be insufficient to fracture a normal bone; the result of reduced compressive and/or torsional strength of bone.
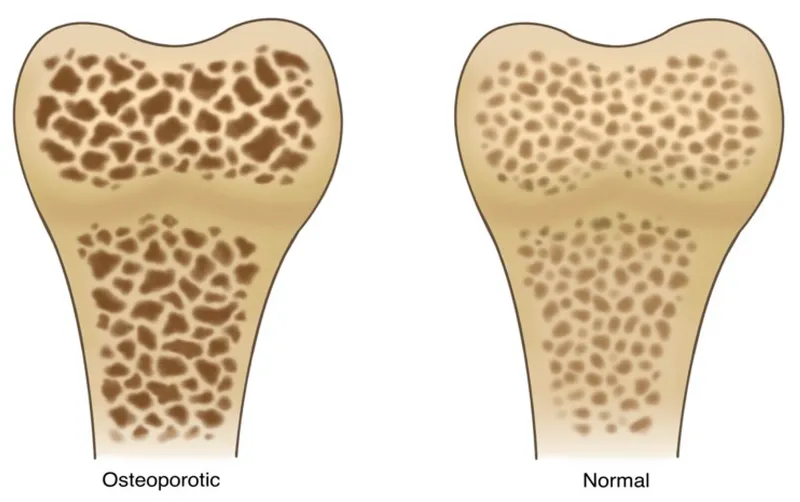
Fragility Fractures - Why They Crumble
⭐ Osteoporosis is the most common underlying cause, characterized by low bone mass (T-score ≤ -2.5) and microarchitectural deterioration of bone tissue.
- Definition: Fracture from low-energy trauma (e.g., fall from standing height or less).
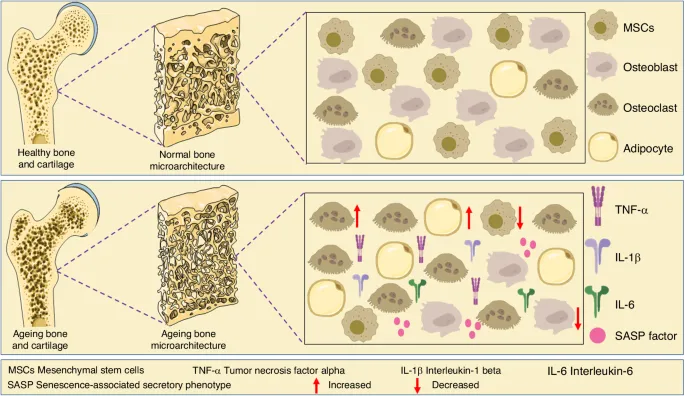
- Pathophysiology: Bone strength is compromised due to:
- ↓ Bone Mineral Density (BMD).
- Impaired bone quality (microarchitecture, turnover, mineralization).
- Key Underlying Causes:
- Osteoporosis: Primary culprit.
- Osteomalacia: Defective mineralization (often ↓ Vitamin D).
- Hyperparathyroidism: ↑ PTH → ↑ bone resorption.
- Paget's Disease: Disorganized, weak bone structure.
- Medications: e.g., chronic corticosteroids.
- Common Sites: Vertebrae (compression), hip, distal radius (Colles'), proximal humerus.
Fragility Fractures - Spotting the Risk
Fragility fracture: results from low-energy trauma (e.g., fall from standing height or less).
-
Key Risk Factors:
- Age >50 yrs; Prior fragility fracture (strongest)
- Glucocorticoid use (e.g., ≥5mg pred/day, ≥3 months)
- Low BMI (<19 kg/m²); Parental hip fracture history
- Current smoking; Alcohol ≥3 units/day
- Secondary osteoporosis (e.g., RA, hypogonadism)
-
Assessment Tools:
- FRAX®: Estimates 10-yr major osteoporotic & hip fracture probability.
⭐ FRAX score predicting a 10-year probability of major osteoporotic fracture ≥ 20% or hip fracture ≥ 3% often warrants pharmacological intervention in many guidelines.
- BMD (DXA): T-score ≤ -2.5 indicates osteoporosis.
- FRAX®: Estimates 10-yr major osteoporotic & hip fracture probability.
Fragility Fractures - Sites & Fixes
- Definition: Fractures from low-energy trauma (e.g., fall from standing height) in weakened bone (osteoporosis).
- Common Sites:
- Vertebrae (spine)
- Hip (femoral neck, intertrochanteric)
- Distal Radius (Colles' fracture)
- Proximal Humerus
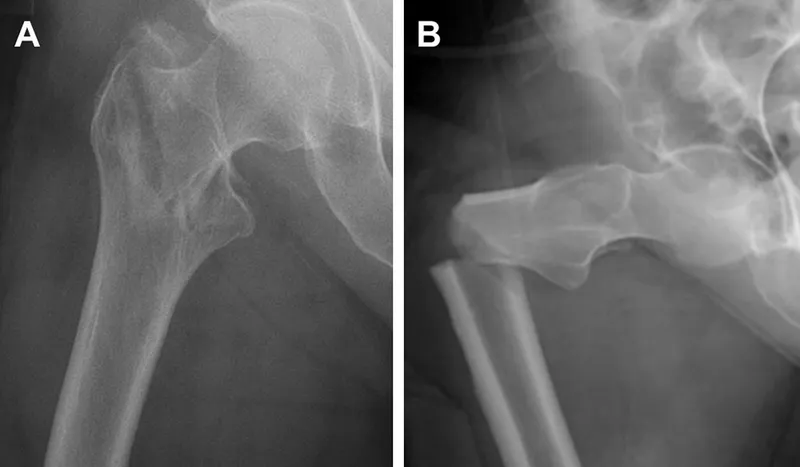
- Clinical Presentation:
- Sudden onset pain, often after minimal trauma.
- Deformity, swelling, ↓ range of motion.
- Vertebral: Height loss, kyphosis, back pain.
- Diagnosis:
- X-ray: Confirms fracture.
- DEXA scan: T-score ≤ -2.5 indicates osteoporosis.
- Management Principles:
- Acute Care: Pain relief (analgesics), immobilisation (splint/cast), DVT prophylaxis.
- Fixation (Site-Specific):
- Hip: ORIF (screws, plates, nails), hemiarthroplasty, total hip replacement (THR).
- Vertebral: Conservative (bracing, analgesia); vertebroplasty/kyphoplasty for persistent pain.
- Distal Radius: Closed reduction & casting; ORIF for unstable/displaced fractures.
- Secondary Prevention (Crucial):
- Calcium & Vitamin D supplementation.
- Anti-osteoporotic meds: Bisphosphonates (alendronate), teriparatide, denosumab, SERMs (raloxifene).
⭐ Vertebral, hip (femoral neck, intertrochanteric), and distal radius (Colles') fractures are the most common sites for fragility fractures.
- Goal: Restore function, prevent future fractures, improve quality of life. 📌 FRAX tool estimates 10-year fracture probability.
High‑Yield Points - ⚡ Biggest Takeaways
- Fragility fractures result from low-energy trauma (e.g., fall from standing height).
- Common sites: vertebrae, hip (proximal femur), wrist (distal radius).
- Osteoporosis is the primary cause; DEXA T-score ≤ -2.5 is diagnostic.
- FRAX score estimates 10-year major osteoporotic fracture risk.
- Management: calcium, vitamin D, bisphosphonates, and fall prevention.
- Rule out secondary causes like long-term steroid use.
- A prior fragility fracture strongly ↑ risk of future fractures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

