STT Intro & Class. - Squishy Suspects
- Definition: Soft Tissue Tumors (STT) are neoplasms from extraskeletal, non-epithelial (mesenchymal) tissues.
- Epidemiology: Benign STT are common. Malignant STT (Sarcomas) are rare, <1% of adult malignancies, ~15% of pediatric malignancies.
- Origin: Mesenchymal tissues (fat, fibrous, muscle, vessel, nerve).
- Classification & Key Differences:
- Benign: Slow growth, usually painless, well-circumscribed, rarely recur, no metastasis (e.g., lipoma, fibroma).
- Malignant (Sarcomas): Rapid/aggressive growth, often painful, ill-defined margins, high recurrence, metastatic potential (e.g., liposarcoma, rhabdomyosarcoma).
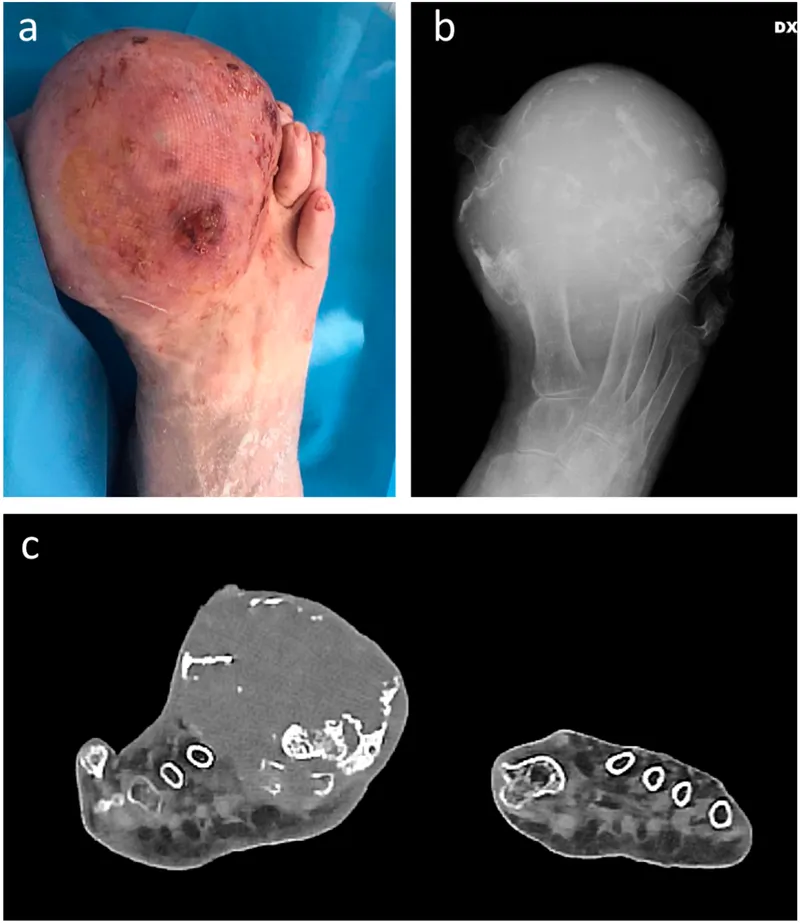
⭐ Sarcomas typically metastasize hematogenously, most commonly to the lungs.
Benign STT - Friendly Lumps
| Tumor | Tissue of Origin | Key Clinical/Path Feature(s) | Typical Location | Simple Management |
|---|---|---|---|---|
| Lipoma | Adipose | Most common STT; soft, mobile, painless, "slippage sign" | Subcutaneous | Excision if symptomatic |
| Fibroma | Fibrous | Firm, slow-growing; superficial (dermatofibroma) or deep (desmoid - locally aggressive) | Extremities, trunk | Observation, excision |
| Hemangioma | Blood Vessel | Red/blue, compressible; capillary (strawberry) or cavernous | Skin, muscle, synovium | Sclerotherapy, laser, excision |
| Neurofibroma | Nerve Sheath | Soft, fleshy, "buttonholing sign"; assoc. NF1 | Peripheral nerves | Excision if symptomatic |
| Schwannoma | Schwann Cells | Encapsulated, eccentric to nerve; Antoni A/B areas | Peripheral nerves | Excision (nerve sparing) |
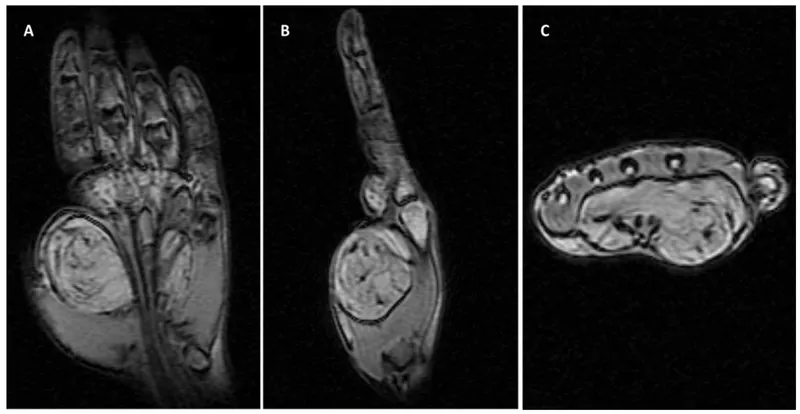
| GCTTS | Synovium | Firm, lobulated, painless mass; hemosiderin-laden macrophages | Fingers, hand, wrist | Marginal excision |
Malignant STT - Sinister Swellings
- General: Rare, deep-seated, >5cm, rapid growth, pain.
- Grading: FNCLCC (Fédération Nationale des Centres de Lutte Contre le Cancer) - based on differentiation, mitosis, necrosis.
- Staging: AJCC TNM (Tumor, Node, Metastasis).
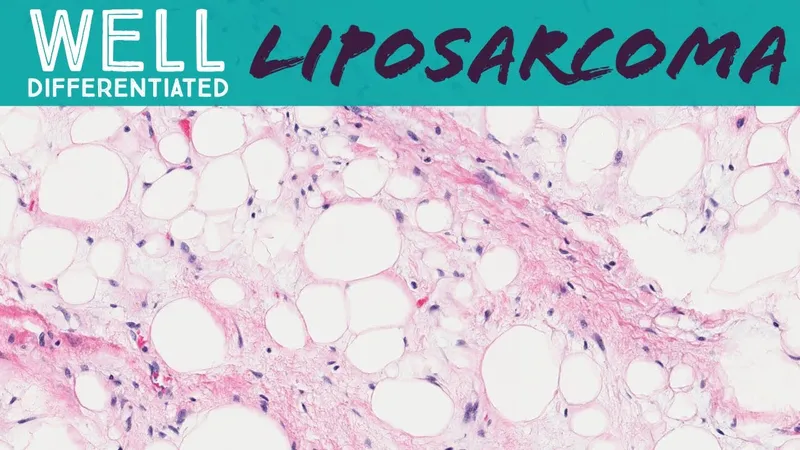
- Common Sarcomas & Key Features:
Sarcoma Key Genetic/Histo Feature Common Site(s) Prognostic Factor Liposarcoma MDM2 amplification (well-diff/de-diff) Thigh, retroperitoneum Subtype, grade Rhabdomyosarcoma Embryonal (botryoid), Alveolar (PAX-FOXO1) Head/Neck, GU tract Subtype, age Synovial Sarcoma SYT-SSX fusion (t(X;18)); biphasic pattern Extremities (knee) Size, grade Leiomyosarcoma Smooth muscle differentiation; spindle cells Uterus, retroperitoneum Grade, location MPNST NF1 association; S100+, SOX10+ Trunk, extremities NF1 status, size
⭐ Rhabdomyosarcoma is the most common soft tissue sarcoma in children, often presenting in head/neck or GU tract.
STT Dx & Mgmt - Unmasking & Tackling
- Clinical Evaluation: History (red flags: pain, rapid growth, size >5cm, deep to fascia), thorough physical exam.
- Imaging:
⭐ MRI is the imaging modality of choice for local staging and characterization of soft tissue tumors, detailing extent and neurovascular relations.
- X-ray (calcification, bone changes), CT chest (metastases), PET-CT (high-grade, staging, response).
- Biopsy: Image-guided core needle biopsy is standard; crucial for accurate diagnosis and grading before definitive treatment.
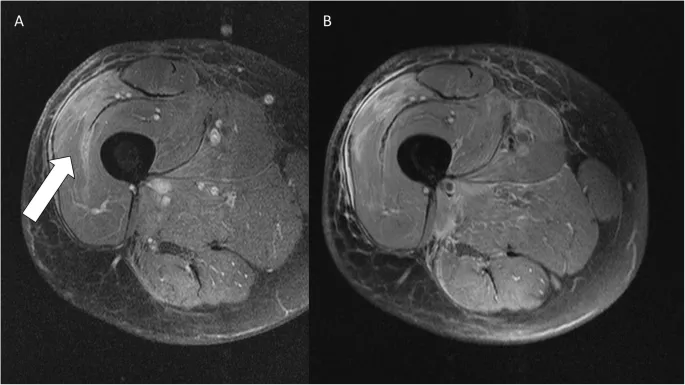
- Treatment Principles: Multidisciplinary team (MDT) approach is essential.
- Surgery: Aim for wide local excision with clear margins (R0 resection).
- Radiotherapy: Neo/adjuvant use common for improved local control.
- Chemotherapy: For chemosensitive types, advanced/metastatic disease, or neoadjuvant.
High‑Yield Points - ⚡ Biggest Takeaways
- UPS (MFH): Most common soft tissue sarcoma (STS) in adults.
- Rhabdomyosarcoma: Most common STS in children; embryonal subtype most frequent.
- Synovial Sarcoma: t(X;18) translocation (SYT-SSX); juxta-articular, not truly synovial.
- Liposarcoma: MDM2 amplification in well-diff/dediff types; often large, deep.
- MRI for local staging; biopsy (core/incisional) confirms diagnosis.
- Wide surgical excision with clear margins: primary treatment for sarcomas.
- Desmoid tumors: Locally aggressive, high recurrence, do not metastasize.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

