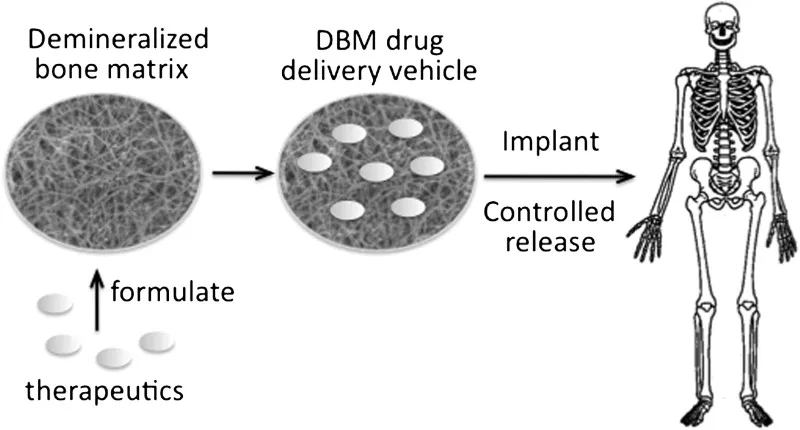
DBM Basics - Bone's Bare Bones
- Origin: Allograft; derived from human cadaveric cortical or cancellous bone.
- Processing:
- Demineralization via acid extraction (e.g., hydrochloric acid).
- Removes inorganic calcium phosphate (hydroxyapatite).
- Preserves organic matrix: primarily collagen and growth factors.
- Key Components:
- ~90% Type I Collagen: Provides an osteoconductive scaffold.
- Non-collagenous proteins: Including crucial Bone Morphogenetic Proteins (BMPs 2, 4, 7), transforming growth factor-beta (TGF-β).
- Mechanism: Primarily osteoinductive (due to BMPs) and osteoconductive.
- Forms: Powder, putty, gel, strips, granules.
⭐ The osteoinductive potential of DBM is directly related to the concentration and activity of retained BMPs, which can vary significantly between products.
DBM's Magic - How It Heals
- Osteoinduction: The Spark of Bone Formation
- DBM releases native Bone Morphogenetic Proteins (BMPs), notably BMP-2 & BMP-7.
- These growth factors recruit and trigger undifferentiated Mesenchymal Stem Cells (MSCs).
- MSCs differentiate into osteoprogenitor cells, then osteoblasts, initiating de novo bone formation.
- Osteoconduction: The Supportive Scaffold
- DBM provides a porous, three-dimensional collagenous matrix.
- This framework guides ingrowth of host capillaries (neovascularization) and osteogenic cells.
- Facilitates organized bone deposition onto its surface.
- Factors Influencing Efficacy:
- BMP Concentration: Highly variable; crucial for osteoinductive strength.
- Donor Factors: Age (↑age often means ↓BMPs), comorbidities.
- Processing Methods: Sterilization (e.g., gamma irradiation can ↓BMP activity), choice of carrier (e.g., glycerol, hyaluronic acid).
⭐ DBM primarily acts via osteoinduction, mediated by its inherent Bone Morphogenetic Proteins (BMPs), which stimulate host mesenchymal stem cells to differentiate into osteoblasts.
Using DBM - Clinical Toolkit
- Available Forms:
- Putty, gel, strips, powder, paste, crunch, injectable.
- Allows versatile application to diverse defect anatomies.
- Advantages:
- Readily available ("off-the-shelf"), sterile.
- Osteoconductive scaffold; biocompatible.
- Osteoinductive potential (BMP-dependent); resorbed by host.
- Versatile: adapts to various defect shapes.
- Disadvantages:
- Variable BMP concentration → unpredictable osteoinductivity.
- Lacks intrinsic structural support; not for primary load-bearing.
- Properties can be carrier-dependent (e.g., handling, resorption rate).
- Minimal, but present, risk of immunogenic response.
- Key Clinical Applications:
- Filling contained bone voids (e.g., cysts, benign tumors, trauma defects).
- Graft extender/enhancer in spinal fusion (e.g., posterolateral fusion).
- Treatment of non-unions or delayed unions.
- Maxillofacial and craniofacial reconstruction.
⭐ DBM's osteoinductive efficacy is critically dependent on the quality and quantity of retained Bone Morphogenetic Proteins (BMPs), which can vary significantly between manufacturers and batches, impacting clinical outcomes.
DBM Caveats - Handle With Care
- Variable Osteoinductivity:
- BMP content (key for bone growth) inconsistent.
- Affected by donor, processing, sterilization.
- Sterilization Impact:
- Gamma irradiation can ↓ BMP activity.
- Ethylene oxide: alternative, potential residuals.
- No Intrinsic Strength:
- Not for primary load-bearing.
- Minimal mechanical support.
- Potential Issues:
- Inflammatory/immune response (rare).
- Disease transmission risk (low, processed).
- Handling: some forms may migrate/washout.
- Contraindications:
- Active local infection.
- Known hypersensitivity.
⭐ DBM's osteoinductive efficacy is highly variable due to inconsistent Bone Morphogenetic Protein (BMP) levels, which sterilization (e.g., gamma irradiation) can significantly reduce.
High‑Yield Points - ⚡ Biggest Takeaways
- DBM is an allograft product, created by acid demineralization of cadaveric bone.
- Its primary mechanism is osteoinduction, driven by Bone Morphogenetic Proteins (BMPs).
- It also offers osteoconduction through its collagen matrix scaffold.
- DBM contains no viable cells (osteogenic potential) and offers negligible structural support.
- The concentration of BMPs can be highly variable between different DBM products.
- Commonly used as a bone graft extender or enhancer in fusions and filling defects.
- Available in various forms like putty, gel, strips, and powder.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more