Amblyopia: Definition & Epidemiology - Lazy Eye Lowdown
- Unilateral or, less commonly, bilateral decrease in Best Corrected Visual Acuity (BCVA).
- Caused by abnormal visual experience during early childhood; no organic ocular pathology.
- Not immediately correctable by refractive means alone.
- Prevalence: 2-5% in the general population.
⭐ Amblyopia is the most common cause of preventable monocular vision loss in children and young adults globally (WHO).
Amblyopia: Pathophysiology & Critical Period - Brain's Blurry Bias
- Pathophysiology: Abnormal visual input (e.g., blur, misalignment) during the critical period.
- Leads to active cortical suppression of the affected eye's input.
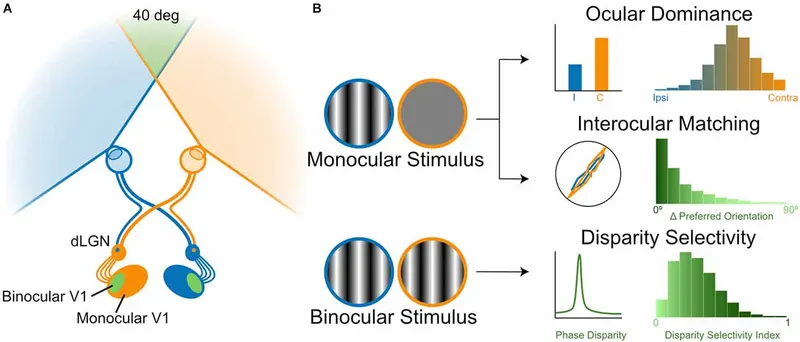
- Results in neurodevelopmental changes in visual cortex (V1) & LGN.
- Critical Period: Birth to ~7-8 years.
- Highest sensitivity: First 2 years of life.
- Neural plasticity for vision is maximal; treatment most effective.
⭐ Uncorrected anisometropia is the most common cause of amblyopia after 3 years of age.
Amblyopia: Etiology & Types - Vision Villain Varieties
- Strabismic Amblyopia:
- Constant unilateral ocular misalignment (tropia).
- Most common type.
- Anisometropic Amblyopia: Unequal refractive power between eyes.
- Hyperopic: > +1.50 D difference.
- Myopic: > -3.00 D difference.
- Astigmatic: > 1.50 D cylindrical difference.
- Stimulus Deprivation Amblyopia: Physical obstruction to clear vision.
- E.g., congenital cataract, significant ptosis, corneal opacity.
- Results in most severe amblyopia; poorest prognosis if untreated.
- Ametropic Amblyopia: Bilateral high, uncorrected refractive errors.
- Hyperopia: > +5.00 D.
- Myopia: > -8.00 D.
- Meridional Amblyopia: Significant uncorrected astigmatism.

⭐ Strabismic amblyopia is the most frequent type, often from esotropia.
Amblyopia: Clinical Features & Diagnosis - Spotting the Slacker Eye
- Often asymptomatic (esp. unilateral), detected on screening.
- Clinical Signs:
- Strabismus (eye turn), head tilt/posture
- Ptosis, nystagmus, abnormal red reflex (Bruckner test)
- Poor fixation/following (infants), ↓depth perception
- Hallmark: ↓Visual Acuity (VA), not fully correctable by glasses.
- Inter-ocular VA diff: ≥2 lines (Snellen)
- Absolute VA: <6/9 (>4y), <6/12 (3-4y)
- Crowding Phenomenon: Worse VA with linear vs. single optotypes.
- Diagnostic Approach:
- Age-appropriate VA (Lea, HOTV, Snellen)
- Cycloplegic refraction (must!)
- Cover test, motility exam
- Ocular exam (media, fundus) to rule out organic pathology.
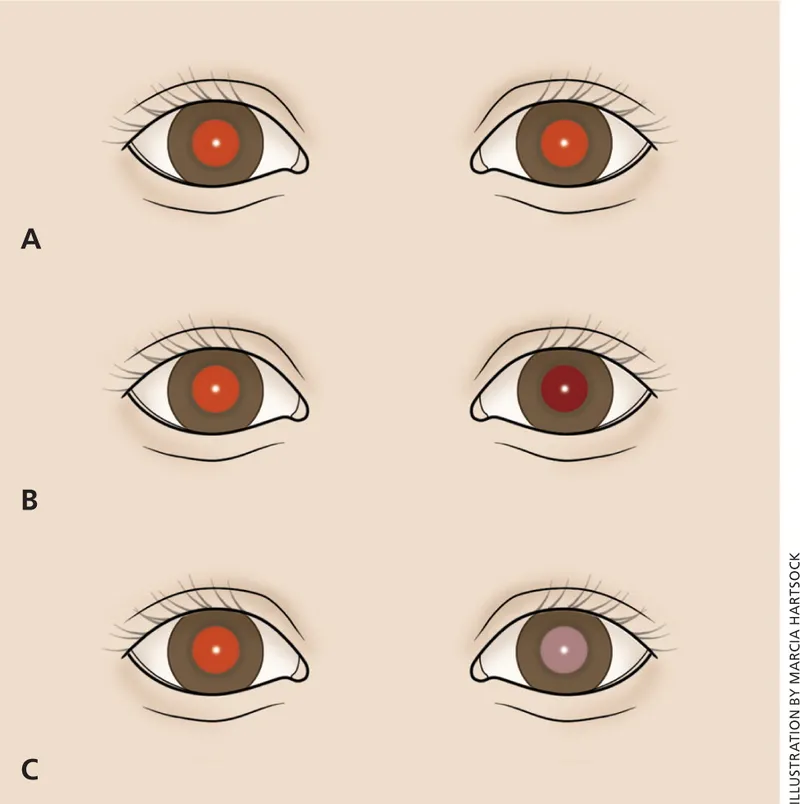
⭐ Amblyopia: diagnosis of exclusion (rule out organic causes). Key: ≥2 line VA difference between eyes.
Amblyopia: Management & Prognosis - Waking Up Vision
- Goal: Ensure clear retinal image; stimulate amblyopic eye use.
- Management Protocol:
-
- Optimal Refractive Correction: Spectacles first. Re-evaluate VA in 6-8 weeks.
-
- Amblyopia Therapy (if VA remains subnormal):
- Occlusion Therapy: Patch good eye. Moderate (20/40-20/80): 2 hours/day. Severe (<20/80): 6 hours/day.
- Pharmacological Penalization: Atropine 1% in non-amblyopic eye (e.g., 2 days/week). Alternative to patching.
- Optical Penalization: Fogging lens over good eye.
- Active Vision Therapy: Binocular treatments, perceptual learning (adjunctive).
-
- Prognosis Factors:
- Age: Best outcome if treated before 7-8 years (critical period). Treatment effective up to 17 years, but response diminishes.
- Type: Strabismic & Anisometropic amblyopia respond better than Deprivation amblyopia.

⭐ Treatment is typically continued until visual acuity shows no further improvement over 2-3 consecutive visits or plateaus.
High‑Yield Points - ⚡ Biggest Takeaways
- Amblyopia: Unilateral/bilateral reduced BCVA (not solely organic), critical period up to ~8 years.
- Most common types: Strabismic, then Anisometropic. Stimulus deprivation is most severe.
- Key sign: Crowding phenomenon (difficulty reading letters in a row).
- Treatment: Correct underlying cause (glasses, surgery), then occlusion therapy (patching) or atropine.
- Early vision screening and treatment initiation are vital for prognosis.
- Untreated amblyopia can lead to permanent vision loss.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more