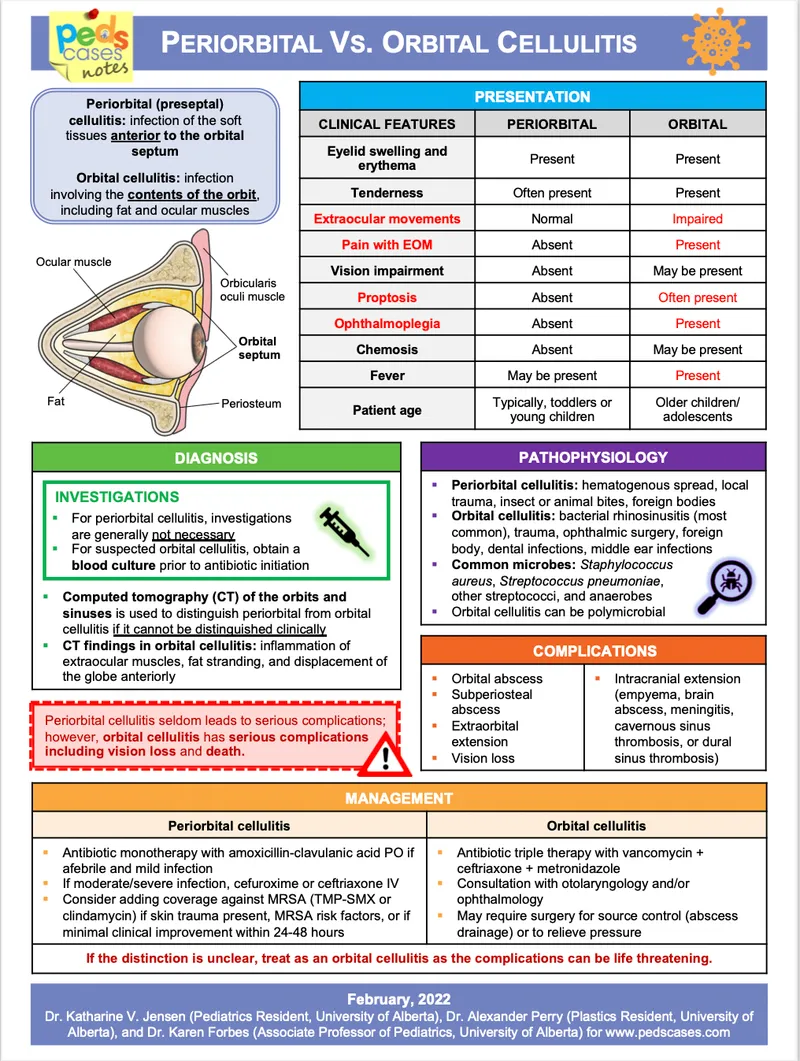
Orbital Anatomy & Overview - Stage for Infection
- Orbital Septum: Key fibrous membrane; acts as anterior orbital boundary.
⭐ The orbital septum is the key anatomical barrier differentiating preseptal (anterior) from orbital (postseptal) cellulitis.
- Paranasal Sinuses: Close proximity; common primary infection sources.
- Ethmoid sinus (most common), maxillary sinus.
- Venous Drainage: Valveless veins (e.g., superior/inferior ophthalmic) allow bidirectional flow.
- Risk of intracranial spread to cavernous sinus.
- Key Spaces: Defined by orbital septum.
- Preseptal space: Anterior to orbital septum; involves eyelids.
- Postseptal (Orbital) space: Posterior to septum; involves orbit proper (globe, muscles, optic nerve).
Preseptal Cellulitis - Eyelid's Red Alert
- Definition: Infection of eyelid & surrounding soft tissues anterior to the orbital septum.
- Etiology:
- Skin trauma (lacerations, abrasions).
- Insect/spider bites.
- Spread from hordeolum, chalazion, dacryocystitis.
- Extension from sinusitis (less common than for orbital cellulitis).
- Common Organisms: Staphylococcus aureus, Streptococcus pyogenes.
- Clinical Features:
- Eyelid: Edema, erythema, warmth, tenderness.
- Key Negatives: NO proptosis, NO ophthalmoplegia, NO pain on eye movements.
- Vision: NORMAL visual acuity, NORMAL pupillary reflexes.
⭐ In preseptal cellulitis, visual acuity, pupillary reactions, proptosis, and ocular motility are characteristically NORMAL.
- Diagnosis: Primarily clinical. CT scan if orbital cellulitis is suspected or if there's no improvement with initial treatment.
- Management:
- Oral antibiotics (e.g., amoxicillin-clavulanate, cephalexin).
- Warm compresses.
Orbital Cellulitis - Deep Trouble Eye
- Definition: Infection posterior to orbital septum.
- Etiology: Sinusitis (esp. ethmoiditis), dacryocystitis, dental infection, trauma.
- Organisms: Strep. pneumoniae, Staph. aureus, H. influenzae, anaerobes.
- Clinical Features: Proptosis, painful ophthalmoplegia, ↓ visual acuity, chemosis, APD, fever.
- Key Differentiators (vs. Preseptal): Proptosis, ophthalmoplegia, ↓VA.
- 📌 Mnemonic (Red Flags - ROPES): Restricted/Painful eye movements, Ophthalmoplegia, Proptosis, Edema/Elevated IOP, Significant vision loss.
- Chandler's: I-Preseptal, II-Orbital, III-Subperiosteal Abscess, IV-Orbital Abscess, V-CST.
- Diagnosis: Urgent CT (orbit & sinuses + contrast). Blood cultures.
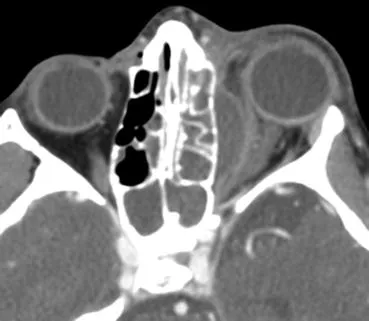
- Management:
- Hospitalize; IV broad-spectrum Abx (Ceftriaxone + Vancomycin; consider anaerobes).
- Surgery if: abscess, ↓VA, or no improvement in 24-48h.
⭐ The most common cause of orbital cellulitis is extension of infection from adjacent paranasal sinuses, particularly the ethmoid sinus.
Complications & Nasties - When Bugs Go Rogue
- Subperiosteal Abscess (SPA):
- Collection: bone & periosteum. Location: medial/superior orbit.
- Drainage: if large, vision threat, or no IV Abx response.
- Orbital Abscess:
- Pus in orbital fat. ↑ risk vision loss.
- Management: Usually drainage.
- Cavernous Sinus Thrombosis (CST):
- Spread: valveless veins.
- Features: Bilateral signs, CN palsies (III-VI, V1/V2), severe headache, sepsis.
- Mortality: High. Rx: IV Abx; anticoagulation controversial.
- Fungal Orbital Infections (e.g., Mucormycosis):
- Form: Rhino-orbital-cerebral.
- Risk: DKA, immunosuppression, iron overload, post-COVID (India).
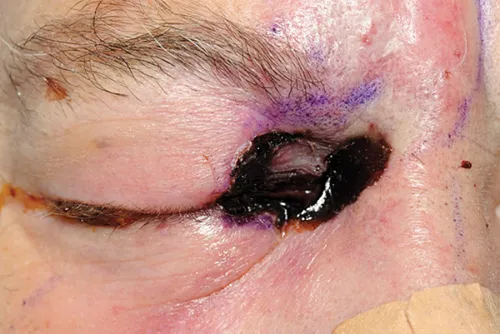
- Features: Black necrotic eschar (nose/palate), rapid progression, multiple CN palsies.
- Dx: Biopsy (broad, non-septate hyphae, right-angle branching).
- Rx: Urgent surgical debridement + IV Ampho B.
⭐ Rhino-orbital mucormycosis is a life-threatening emergency characterized by black necrotic eschar and requires immediate aggressive surgical debridement and systemic antifungal therapy (Amphotericin B).
High‑Yield Points - ⚡ Biggest Takeaways
- Preseptal cellulitis: Eyelid inflammation, NO proptosis, NO ophthalmoplegia, normal vision.
- Orbital cellulitis: Proptosis, painful ophthalmoplegia, ↓ vision; often from ethmoid sinusitis.
- Common organisms: Staphylococcus aureus, Streptococcus pneumoniae, H. influenzae (in unvaccinated).
- Cavernous Sinus Thrombosis: Critical complication, look for bilateral signs, cranial nerve palsies.
- Management: IV antibiotics (broad-spectrum); surgical drainage for abscess or no improvement.
- Rhino-orbital-cerebral mucormycosis: Aggressive fungal infection in diabetics (DKA); black necrotic eschar.
- Chandler's classification stages orbital complications of sinusitis from preseptal to cavernous sinus thrombosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

