Pathophysiology & Risks - Genesis of Graves' Gaze
- Autoimmune: Graves' disease; T-cell mediated.
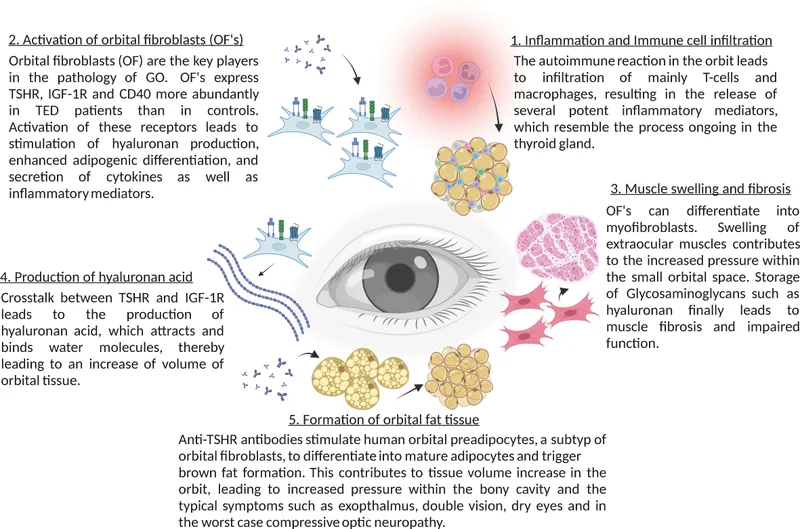
- Mechanism: TSH-Receptor Antibodies (TRAb) target TSH-R on orbital fibroblasts.
- Fibroblast activation: ↑ proliferation, differentiation.
- ↑ Glycosaminoglycan (GAG) production (hyaluronan) → edema.
- ↑ Adipogenesis (fat cell formation).
- Outcome: Orbital tissue expansion, muscle swelling, inflammation, fibrosis.
- Risk Factors:
- Smoking (strongest modifiable).
- Female sex.
- Genetics (HLA-DR3).
- Radioiodine therapy (can worsen).
⭐ Key pathogenic mechanism: autoantibodies against TSH receptor (TSH-R) on orbital fibroblasts, leading to glycosaminoglycan accumulation and adipogenesis.
Clinical Features - The Proptotic Profile
- Proptosis (Exophthalmos):
- Hallmark of TED; bilateral, often asymmetric.
- Hertel: Normal < 21mm (Caucasians), < 18mm (Asians); inter-eye > 2mm diff. significant.
- Severity: Mild (21-23mm), Mod. (24-27mm), Severe (>28mm).
- Key Eyelid Signs:
- Lid Retraction (Dalrymple's): Most common; sclera above limbus.
- Von Graefe's: Lid lag (downgaze).
- Stellwag's: Infrequent blinking.
- Soft Tissue:
- Eyelid/periorbital edema.
- Conjunctival injection (over recti), chemosis.
⭐ Exophthalmos (proptosis) is the hallmark of TED; lid retraction (Dalrymple's sign) is the most common ocular sign.
Classification - Staging the Stare
NOSPECS Classification (Severity) 📌
- Grades manifestations:
Class Finding 0 No signs/symptoms I Only signs (lid retraction) II Soft tissue III Proptosis (>22mm) IV EOM involvement V Corneal VI Sight loss (Optic Neuropathy)
Clinical Activity Score (CAS) (Activity)
- Active: ≥3/7 or ≥4/10. 1 point/sign.
Original CAS (7 signs) Expanded adds (3 signs) Pain (spontaneous/gaze) ↑ Proptosis ≥2mm Eyelid redness/swelling ↓ Motility ≥8° Conj. redness/chemosis ↓ VA ≥1 line Inflamed caruncle/plica
⭐ The Clinical Activity Score (CAS) is essential for determining active inflammation and guiding immunosuppressive therapy.
Investigations - Unmasking Orbitopathy
- Thyroid Function Tests (TFTs): TSH, fT3, fT4.
- Autoantibodies:
- TSH Receptor Antibodies (TRAb) - key diagnostic marker.
- Anti-Thyroid Peroxidase (Anti-TPO) Antibodies.
- Orbital Imaging:
⭐ CT or MRI of the orbits typically reveals fusiform enlargement of extraocular muscle bellies with sparing of the tendons.
- Assesses Extraocular Muscles (EOMs) (📌 IMSLO: Inferior > Medial > Superior > Lateral > Obliques), optic nerve.
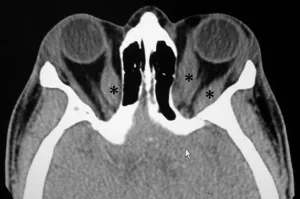
- Assesses Extraocular Muscles (EOMs) (📌 IMSLO: Inferior > Medial > Superior > Lateral > Obliques), optic nerve.
- Functional Tests: Visual fields, color vision (for optic neuropathy).
Management - Calming the Crisis
- Supportive: Smoking cessation, lubricants, selenium.
- Activity: CAS (Clinical Activity Score; active if ≥3/7).
- Severity: NOSPECS / EUGOGO. (📌 NO SPECS: No signs/symptoms, Only signs, Soft tissue, Proptosis, EOM involvement, Corneal, Sight loss).
⭐ Sight-threatening dysthyroid optic neuropathy (DON) is an ophthalmic emergency managed with urgent high-dose systemic corticosteroids (e.g., IV methylprednisolone).
High‑Yield Points - ⚡ Biggest Takeaways
- Thyroid Eye Disease (TED) is the most common cause of proptosis in adults, often bilateral.
- Strongest association with Graves' disease; mediated by TSH receptor antibodies.
- NOSPECS classification is used for severity; optic neuropathy is the most serious complication.
- Classic signs include lid retraction (Dalenrymple's) and lid lag (Von Graefe's).
- Inferior rectus is the most frequently affected extraocular muscle, then medial rectus.
- Treatment aims to manage activity and severity: steroids, radiotherapy, surgical decompression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

