Emotional Rollercoaster - Initial Reactions
- Common initial emotional responses:
- Shock, Denial
- Anger, Resentment
- Anxiety, Fear
- Depression, Sadness
- Grief Process (adapted Kübler-Ross 📌 DABDA):
- Shock / Denial
- Anger / Resentment
- Bargaining
- Depression / Despair
- Acceptance / Adaptation
⭐ Depression is the most common psychiatric comorbidity in individuals with visual impairment, affecting up to 30-40% of older adults with vision loss.
Mind Over Matter - Coping & Adjustment
- Stages of Adjustment:
- Crisis: Shock, denial.
- Stabilization: Emotional turmoil, realization.
- Resolution/Reintegration: Acceptance, adaptation.
- Coping Strategies:
- Adaptive (Positive):
- Problem-focused (e.g., new skills).
- Emotion-focused (e.g., managing distress).
- Seeking support (social, professional).
- Positive reframing.
- Maladaptive (Negative):
- Avoidance, denial (prolonged).
- Substance abuse.
- Social withdrawal.
- Adaptive (Positive):
- Key Factors:
- Resilience: Ability to bounce back.
- Locus of Control: Internal (empowerment) vs. External.
⭐ An internal locus of control and strong social support are significant predictors of successful psychosocial adjustment to vision loss.
- Self-Efficacy: Belief in one's capabilities. 📌 PAUSE: Positive Adaptive Unfaltering Self-Efficacy.
Support Systems - Interventions & Help
- Psychological Counseling: Crucial for emotional adjustment and coping with vision loss.
- Cognitive Behavioral Therapy (CBT): Targets negative thought patterns, enhances coping skills.
⭐ Cognitive Behavioral Therapy (CBT) is effective in reducing symptoms of depression and anxiety and improving coping skills in patients with low vision.
- Supportive Therapy: Provides emotional validation and empathetic listening.
- Problem-Solving Therapy: Focuses on developing practical solutions to daily challenges.
- Cognitive Behavioral Therapy (CBT): Targets negative thought patterns, enhances coping skills.
- Support Networks: Vital for reducing isolation and fostering resilience.
- Peer Support Groups: Offer shared experiences, mutual encouragement, and practical advice.
- Family Therapy & Education: Engages family members, improving understanding and support.
- Social Support Networks: Broader community, friends, and resources providing assistance.
- Multidisciplinary Team (MDT) Approach: Ensures comprehensive, patient-centered care.
- Core Team: Ophthalmologist, Optometrist, Low Vision Rehabilitation Specialist, Psychologist, Social Worker.
Quality of Life - Beyond Sight
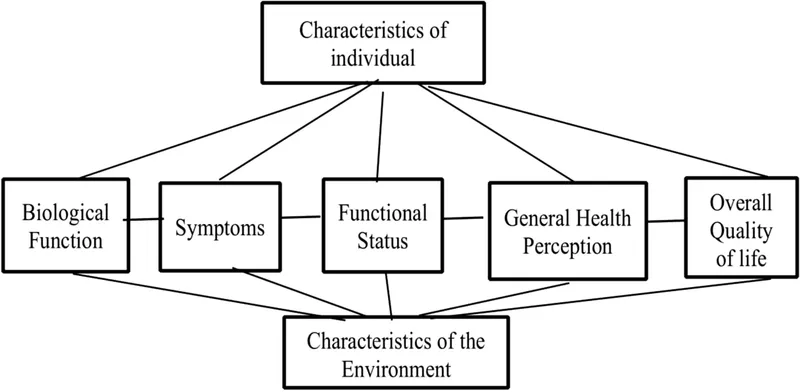
- Visual impairment significantly impacts QoL:
- Difficulty with Activities of Daily Living (ADLs) & Instrumental ADLs (IADLs).
- Reduced independence & social participation.
- Affects body image & self-esteem.
- Strategies to improve QoL: Maximize residual vision, adaptive aids, counseling, support groups.
Charles Bonnet Syndrome (CBS)
| Feature | Description |
|---|---|
| Prevalence | ~10-40% in low vision. |
| Hallucinations | Complex, formed visual (non-psychiatric); insight preserved. |
| 📌 Mnemonic | Complex Benign Sightings (Visual, Vivid, Silent) |
| Management | Reassurance, education, ↑lighting, visual search techniques, manage anxiety. |
High‑Yield Points - ⚡ Biggest Takeaways
- Visual impairment commonly triggers depression, anxiety, and grief reactions.
- Kubler-Ross model (DABDA) often describes the stages of emotional adjustment.
- Charles Bonnet Syndrome: formed visual hallucinations with clear sensorium and insight.
- Expect significant ↓ in Quality of Life (QoL) and functional independence.
- Psychological counseling and support groups are key to successful rehabilitation.
- Social isolation is a frequent and debilitating consequence.
- Early psychiatric referral for severe cases improves outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

