SOAGs Intro - Not Just POAG!
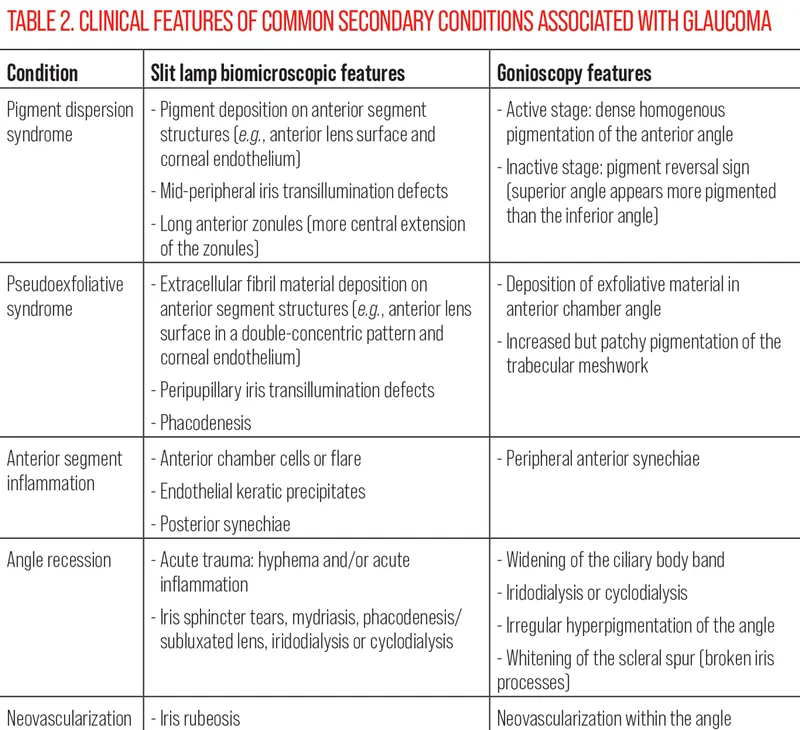
- Definition: SOAGs are glaucomas with ↑IOP from an identifiable secondary cause, despite an open, normal-appearing anterior chamber angle.
- SOAG vs. POAG:
- POAG: Idiopathic trabecular meshwork (TM) dysfunction.
- SOAG: Known cause for TM obstruction.
- Mechanisms of TM Obstruction:
- Pre-trabecular: Membrane/tissue over TM (e.g., neovascularization, ICE syndrome).
- Trabecular: Clogging within the TM itself.
- Cells: RBCs (ghost cell glaucoma), inflammatory cells (uveitic glaucoma).
- Material: Pigment (pigment dispersion), pseudoexfoliation (PXF) material, lens proteins (phacolytic).
- Steroid-induced: Altered TM matrix/cellularity.
⭐ Exam Favourite: Steroid-induced glaucoma is a classic SOAG; risk varies with steroid potency, duration, route of administration (topical > periocular > systemic > inhaled), and individual susceptibility (e.g., POAG patients, diabetics).
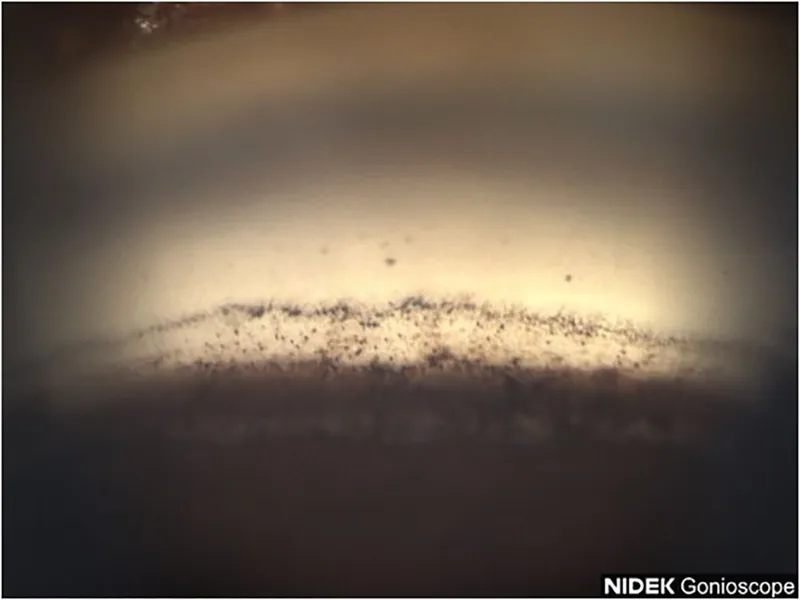
Exfoliation & Pigmentary - Debris Drama Duo
-
Common Theme: Trabecular meshwork (TM) obstruction by particulate debris leading to ↑IOP.
-
Exfoliation Syndrome (XFS) & Glaucoma (PXG):
- Debris: White "dandruff-like" pseudoexfoliative material (PXM) from abnormal basement membrane.
- Key Signs:
- PXM on pupil margin, anterior lens capsule ("bull's-eye" sign).
- Sampaolesi's line.
- Moth-eaten iris transillumination.
- Zonular weakness (↑cataract sx risk).
- Course: Often unilateral, aggressive.
-
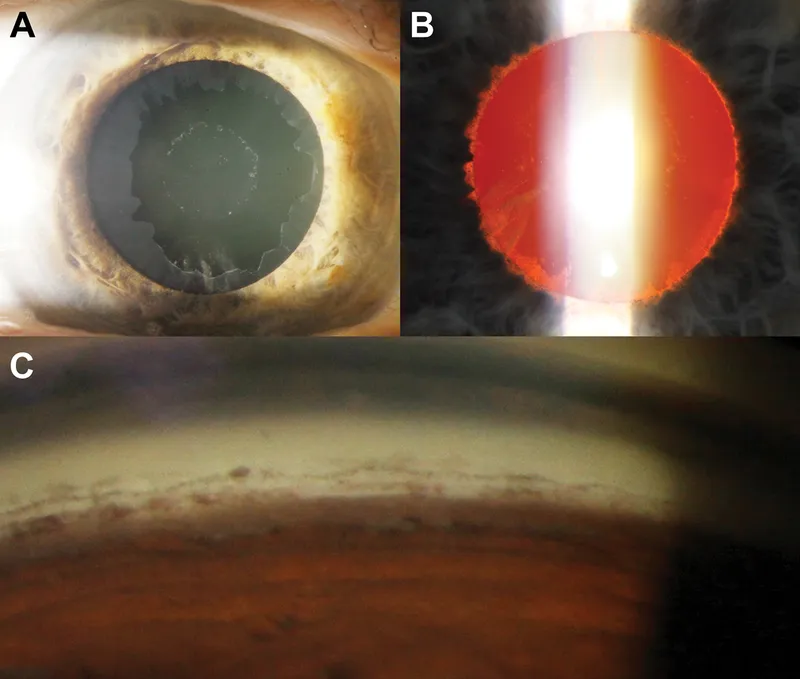
Pigment Dispersion Syndrome (PDS) & Glaucoma (PG):
- Debris: Iris pigment granules from posterior iris epithelium rubbing against lens zonules.
- Classic Triad:
- Krukenberg spindle (vertical pigment on corneal endothelium).
- Radial, mid-peripheral iris transillumination defects.
- Dense TM pigmentation (often 360°).
- Profile: Younger, myopic males.
- Course: Bilateral; exercise/mydriasis → pigment showers, IOP spikes.
⭐ Pigmentary glaucoma often shows greater IOP fluctuations than POAG, with spikes after exercise or mydriasis, and may "burn out" in later life as pigment liberation decreases.
Steroid & Uveitic - Pressure & Passion Plays
- Steroid-Induced Glaucoma:
- Patho: ↑Aqueous outflow resistance (Trabecular Meshwork - TM changes: ↑GAGs, ↓PGEs, altered ECM).
- Risk factors: Route (topical > periocular > systemic), potency, duration, family Hx of POAG.
- "Steroid responders": Genetically predisposed individuals.
- Rx: Discontinue/taper steroid. IOP-lowering drugs (avoid Prostaglandin Analogs initially). Surgery if refractory.
- Uveitic Glaucoma (Open Angle):
- Mechanism: TM inflammation/blockage by cells, fibrin, debris. Can be steroid-induced if steroids used for uveitis.
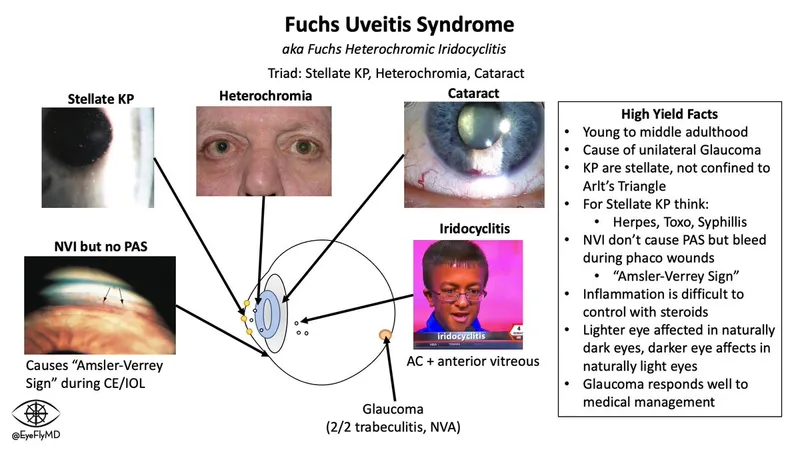
- Fuchs' Heterochromic Iridocyclitis (FHI): Chronic, low-grade inflammation; stellate keratic precipitates (KPs), iris heterochromia, cataract, glaucoma (often late, difficult to control).
- Posner-Schlossman Syndrome (PSS) / Glaucomatocyclitic Crisis: Recurrent, unilateral, acute ↑IOP; mild anterior chamber (AC) reaction, few KPs, open angle. 📌 "PSS - Painful, Seeing, Single eye".
- Rx: Control inflammation (topical steroids, mydriatics). IOP-lowering drugs (aqueous suppressants preferred; miotics contraindicated in active inflammation).
⭐ In Posner-Schlossman Syndrome, IOP can rise very high (e.g., 40-60 mmHg) with minimal cells in AC and an open angle on gonioscopy.
Lens & Trauma - Crystal Clear Damage
- Lens-Induced Glaucomas (SOAG):
- Phacolytic Glaucoma:
- Hypermature cataract leaks lens proteins.
- Macrophages engulf proteins, obstruct Trabecular Meshwork (TM).
- Acute: ↑IOP, pain, cells/flare.
- Tx: Medical, then cataract extraction.
- Lens Particle Glaucoma:
- Lens matter (post-trauma/surgery) obstructs TM.
- Tx: Medical, surgical removal.
- Phacolytic Glaucoma:
- Traumatic Glaucomas (SOAG):
- Angle Recession Glaucoma:
- Blunt trauma → ciliary body tear, TM damage/scarring.
- Develops years later; gonioscopy: widened ciliary body band.
- Risk: ~10% if >180° recession.
- Tx: Medical, trabeculectomy.
- Ghost Cell Glaucoma: 📌 "Old ghosts (RBCs) haunt the TM"
- Degenerated RBCs (ghost cells) from vitreous hemorrhage block TM.
- Khaki-colored cells in AC.
- Tx: Medical, AC washout.
⭐ Ghost cell glaucoma typically occurs 2-3 weeks after vitreous hemorrhage, presenting with elevated IOP and khaki-colored cells.
- Angle Recession Glaucoma:
High‑Yield Points - ⚡ Biggest Takeaways
- Pseudoexfoliation syndrome: Most common identifiable cause; white flaky deposits on anterior lens capsule, angle.
- Pigment dispersion syndrome: Features Krukenberg spindle, iris transillumination defects; common in young myopes.
- Lens-induced glaucoma: Includes phacolytic (leaked proteins from hypermature cataract) and lens particle types.
- Steroid-induced glaucoma: Results from prolonged steroid use, impairing trabecular meshwork outflow.
- Uveitic glaucoma: Arises from TM blockage by inflammatory cells/debris or trabeculitis.
- Traumatic glaucoma: Often due to angle recession or ghost cells post-vitreous hemorrhage.
- Glaucomatocyclitic crisis (Posner-Schlossman): Recurrent, unilateral ↑IOP with mild anterior uveitis; open angles maintained during attacks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

