Intro & Etiology - Cloudy Beginnings
- Definition: Lens opacity at birth or early infancy, obstructing visual axis, potentially causing amblyopia.
- Significance: Leading cause of treatable childhood blindness. Early intervention (first 2-3 months) crucial for visual development.
- Etiology:
- Genetic:
- Autosomal Dominant (AD) most common for isolated cataracts.
- AR, X-linked; syndromic (e.g., Down's, Lowe's).
- Metabolic:
- Galactosemia (""oil-droplet"" cataract).
- Hypoglycemia, Hypocalcemia.
- Intrauterine Infections:
- 📌 TORCH: Toxoplasmosis, Other (Syphilis, VZV), Rubella (classic), CMV, Herpes.
- Trauma: Rare (e.g., birth injury).
- Idiopathic: ~30-50% of cases.
- Genetic:
⭐ Most common inheritance for isolated congenital cataracts: Autosomal Dominant.
Morphology & Syndromes - Cataract Shapes & Links

| Type | Key Feature | Association(s) / Notes |
|---|---|---|
| Lamellar/Zonular | Disc-like opacity around clear nucleus; "riders" | Most common congenital |
| Polar (Ant/Post) | Opacity at anterior or posterior lens pole | Post: PHPV, Mittendorf dot |
| Nuclear | Central, dense opacity in embryonic nucleus | Hereditary, early visual impact |
| Cortical | Peripheral wedge/punctate opacities | Developmental, less common |
| Sutural (Y-shaped) | Opacity along Y-sutures | Usually minimal visual impact |
| Blue-dot/Punctate (C. Punctata Caerulea) | Multiple small, bluish dots in deep cortex/nucleus | Often non-progressive, AD |
| Membranous | Thickened capsule, absorbed lens matter | Post-trauma, inflammation |
| Total | Entire lens opaque, no red reflex | Severe, early visual loss |
| Oil-droplet | Central refractile opacity (retroillumination) | Galactosemia (reversible) |
- Associated Syndromes:
- Lowe's Syndrome: Cataract (~50%), posterior lenticonus
- Down's Syndrome (Trisomy 21): Flake-like, sutural, cerulean
- Hallermann-Streiff: Membranous, microphthalmia
- Congenital Rubella: Nuclear, total; "salt & pepper" fundus
- Galactosemia: Oil-droplet (reversible early), zonular
- Alport's Syndrome: Anterior lenticonus, PSC
- Wilson's Disease: Sunflower cataract (copper)
- Myotonic Dystrophy: Christmas tree (polychromatic), PSC
Clinical Features & Diagnosis - Spotting the Haze
- Symptoms (Parental/Pediatrician Concern):
- Leukocoria (white pupil) - hallmark sign!
- Poor visual fixation, nystagmus (involuntary eye movements), strabismus (misaligned eyes).
- Photophobia (light sensitivity).
- Absent or abnormal red reflex.
- Diagnostic Evaluation:
- Visual Acuity: Age-appropriate methods (e.g., fixation preference, Teller cards).
- Bruckner Test: Assesses symmetry of red reflexes.
- Ophthalmoscopy (Direct/Indirect): To view red reflex, lens, and fundus.
- Slit-lamp Examination: Detailed view of cataract morphology; opacity > 3mm or central is often visually significant.
- B-scan Ultrasonography: If dense cataract obscures fundus view, to rule out posterior pathology.
⭐ Leukocoria in a child is an ocular emergency requiring urgent evaluation to exclude retinoblastoma and congenital cataract.


Management & Complications - Clearing the View
- Surgical Timing (Critical Window):
- Bilateral significant cataracts: by 4-6 weeks of age.
- Unilateral significant cataracts: by 6-8 weeks of age.
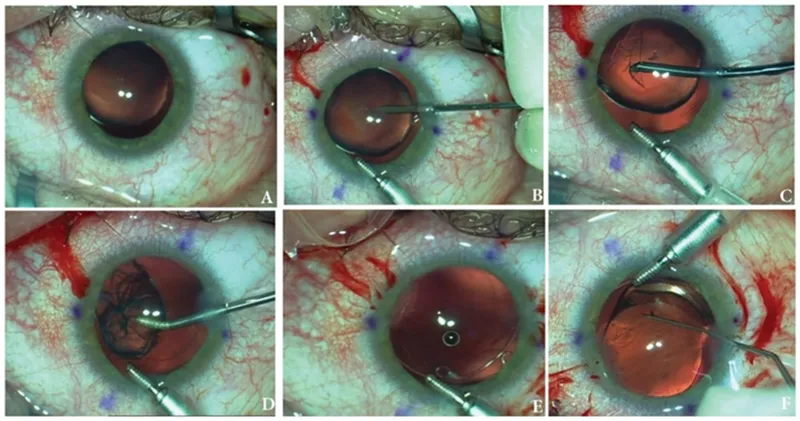
- Surgical Procedures:
- Lensectomy (lens removal).
- Anterior vitrectomy (common in infants, prevents PCO).
- Primary Posterior Capsulotomy (PPC).
- IOL Implantation:
- Primary (at surgery) vs. Secondary (later).
- Challenges: Power calculation (growing eye); target slight hypermetropia.
- Amblyopia Management (CRUCIAL):
- Aggressive patching of sound eye.
- Optical correction: Aphakic glasses, contact lenses, IOL.
- Complications:
- Glaucoma (most common serious long-term).
- Posterior Capsular Opacification (PCO).
- Retinal detachment, Strabismus, Nystagmus, Endophthalmitis.
⭐ The most common and serious long-term complication following congenital cataract surgery is secondary glaucoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Leukocoria (white reflex) is a critical sign; urgent referral is mandatory.
- Amblyopia is the major risk; early surgery (e.g., <2 months for dense bilateral) is crucial.
- Lamellar cataract is the most common type of developmental cataract.
- Maternal rubella (1st trimester) causes pearly nuclear cataracts & microphthalmos.
- Galactosemia presents with an "oil-droplet" cataract, reversible with early dietary restriction.
- Hereditary cataracts are most commonly autosomal dominant.
- Posterior polar cataracts: high risk of posterior capsular rupture during surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

