HPO Axis Regulation - Brainy Ovary Chat
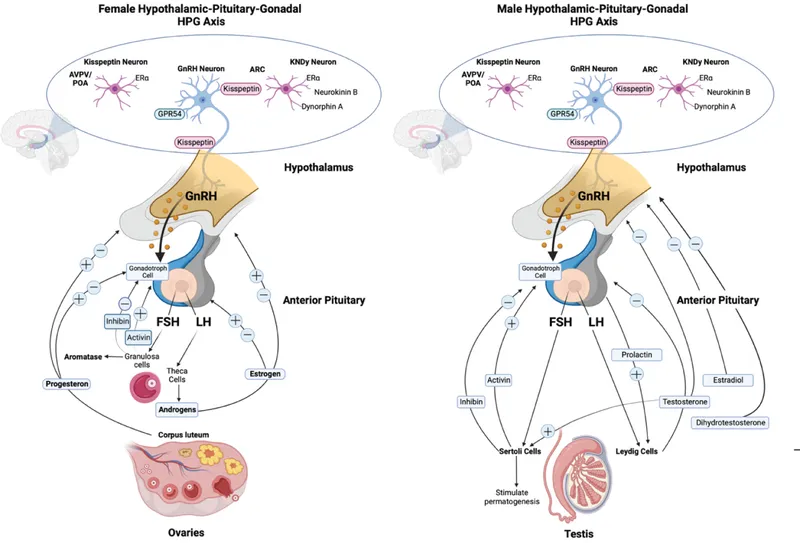
- Hypothalamus: Secretes GnRH in critical pulses; Kisspeptin is a key modulator.
- Anterior Pituitary: GnRH stimulates gonadotrophs to release FSH and LH.
- Ovary:
- FSH: Drives follicular maturation; granulosa cells produce estrogen & inhibin.
- LH: Theca cells (androgens); mid-cycle surge → ovulation; corpus luteum → progesterone.
- Feedback Control:
- Negative: Estrogen, progesterone, inhibin (↓FSH) suppress hypothalamus & pituitary.
- Positive: Sustained high estrogen (mid-cycle) induces pituitary LH surge → ovulation.
- Flowchart:
- Exam Highlight:
⭐ Pulsatile GnRH is essential. Continuous GnRH (agonists) causes pituitary desensitization, ↓FSH/LH. Used for endometriosis, fibroids, precocious puberty.
Hypothalamic Disorders - Stress & Scent Woes
- Functional Hypothalamic Amenorrhea (FHA): Reversible ↓GnRH pulsatility.
- Causes: Stress (psychological, intense exercise), nutritional deficits (low body weight, eating disorders).
- Pathophysiology: ↓GnRH pulsatility → ↓LH, ↓FSH → ↓$E_2$ → anovulation, amenorrhea.
- Diagnosis: Low/normal FSH & LH, low $E_2$. Negative progestin challenge (no withdrawal bleed).
- Management: Address underlying cause, HRT for bone protection if prolonged.
- Kallmann Syndrome: Genetic disorder; failed migration of GnRH & olfactory neurons.
- Features: Hypogonadotropic hypogonadism (delayed/absent puberty) + Anosmia or Hyposmia.
- 📌 Mnemonic: KALlmann = Kills Aroma (anosmia) & Lowers Life (gonads).
- Diagnosis: ↓FSH, ↓LH, ↓sex steroids; MRI (olfactory bulb aplasia/hypoplasia).
- Management: Pulsatile GnRH for fertility; HRT for secondary sexual characteristics.
⭐ Kallmann Syndrome: congenital GnRH deficiency with anosmia/hyposmia, often X-linked (KAL1 gene).
Pituitary Gland Disorders - Gland Gone Wild

- Hyperprolactinemia: Prolactin >25 ng/mL. Commonest pituitary hyperfunction.
- Causes: Prolactinoma (PRL often >200 ng/mL), drugs (antipsychotics, metoclopramide), hypothyroidism, stalk compression.
- Sx: Galactorrhea, amenorrhea, infertility.
- Rx: Dopamine agonists (cabergoline, bromocriptine). Pituitary MRI for diagnosis.
⭐ Prolactinomas are the most common hormone-secreting pituitary adenomas.
- Sheehan's Syndrome: Postpartum pituitary necrosis from severe obstetric hemorrhage.
- Leads to panhypopituitarism.
- Sx: Agalactia (earliest), amenorrhea, fatigue.
- Rx: Hormone replacement therapy.
- Pituitary Apoplexy: Sudden hemorrhage into a pituitary adenoma.
- Sx: Severe headache, visual loss, ophthalmoplegia. ⚠️ Neurological emergency!
- Rx: Steroids, ?surgery.
- Empty Sella Syndrome: CSF fills sella. Often incidental; can cause hypopituitarism.
Systemic Influences & Dx - Hormone Harmony Hunt
- Systemic Disruptors:
- Thyroid: ↑/↓ TSH → anovulation.
- Adrenal: ↑ Cortisol/Androgens (Cushing's, CAH) → cycle disruption.
- Pituitary: ↑ Prolactin (Prolactinoma) → amenorrhea, galactorrhea.
- Metabolic: PCOS, obesity → insulin resistance.
- Stress, eating disorders, chronic illness.
- Diagnostic "Hormone Hunt":
- History & Exam (menstrual, virilization signs, galactorrhea).
- Labs:
- Initial: FSH, LH, Estradiol, Prolactin, TSH.
- Specific: Testosterone, DHEAS, 17-OHP.
- Imaging: Pelvic USG, Pituitary MRI (if indicated).
- 📌 Prolactin, Androgens, Thyroid, HPO axis - PATH to Dx.
⭐ Prolactin levels > 100 ng/mL strongly suggest prolactinoma; levels 20-100 ng/mL can be due to drugs, stress, or pituitary stalk compression (non-pathological hyperprolactinemia).
High‑Yield Points - ⚡ Biggest Takeaways
- Hypothalamic amenorrhea: Due to stress, weight loss, or excessive exercise; results in low GnRH, FSH, LH, and estrogen.
- Kallmann syndrome: Features anosmia & hypogonadotropic hypogonadism from defective GnRH neuron migration.
- Sheehan's syndrome: Postpartum pituitary necrosis causing panhypopituitarism; lactation failure is a key early sign.
- Hyperprolactinemia: A common cause of amenorrhea & infertility; prolactin inhibits GnRH. Often due to prolactinomas or drugs (e.g., antipsychotics).
- PCOS: Neuroendocrine aspects include ↑LH/FSH ratio, androgen excess, and insulin resistance, disrupting ovulation.
- Empty Sella Syndrome: CSF fills sella turcica, potentially compressing the pituitary; may cause hypopituitarism or be asymptomatic.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

