Antepartum Hemorrhage - Before Baby Bleeds
APH: Vaginal bleeding >20-24 wks gestation, pre-labor.
Causes & Features:
- Placenta Previa: Placenta over/near os. Painless, bright red bleed; soft uterus.
- Types: Low-lying, Marginal, Partial, Complete (📌 LMPC).

- Types: Low-lying, Marginal, Partial, Complete (📌 LMPC).
- Abruptio Placentae: Premature placental separation. Painful, dark red bleed; tender, rigid uterus.
- Vasa Previa: Unprotected fetal vessels over os. Painless bleed with ROM; fetal distress.
Previa vs. Abruption:
| Feature | Placenta Previa | Abruptio Placentae |
|---|---|---|
| Bleeding | Bright red, no pain | Dark red, pain |
| Uterine Tone | Soft | Tense, rigid (woody) |
| Fetal Distress | Late / None | Early / Common |
- ABCs, maternal stabilization (IVs, fluids, blood).
- Fetal assessment (CTG, USG). ⚠️ No PV exam till USG excludes previa.
- Delivery: Based on stability, GA, APH type.
⭐ Painless, causeless, recurrent bright red 3rd trimester bleeding strongly suggests placenta previa.
Postpartum Hemorrhage - Aftershock Bleed
-
Definition: Loss of >500ml blood after SVD or >1000ml after CS.
- Primary PPH: Within 24 hours postpartum.
- Secondary PPH: From 24 hours up to 12 weeks postpartum.
-
Causes 📌 '4 T’s':
- Tone: Uterine atony (most common, ~70-80%).
- Trauma: Genital tract lacerations (cervical, vaginal, perineal), uterine rupture, uterine inversion.
- Tissue: Retained products of conception (placenta, membranes, clots).
- Thrombin: Coagulopathies (pre-existing or acquired e.g., DIC, HELLP).
-
Active Management of Third Stage of Labor (AMTSL) (Prophylaxis):
- Oxytocin $10 \text{ IU}$ IM/IV.
- Controlled cord traction.
- Uterine massage after placental delivery.
-
Management of PPH:
- Initial: Call for help (CODE RED/BLUE), ABCs (Airway, Breathing, Circulation), 2 large-bore IV lines, uterine massage.
- Uterotonics:
- Oxytocin: $20-40 \text{ IU}$ in 1L crystalloid IV infusion.
- Misoprostol: $800-1000 \text{ µg}$ per rectum/sublingual/oral.
- Ergometrine: $0.2-0.5 \text{ mg}$ IM or slow IV (Contraindicated: Hypertension, cardiac disease).
- Carboprost (PGF2α): $0.25 \text{ mg}$ IM, q15-90min, max 8 doses (Contraindicated: Asthma).
- Tranexamic Acid: $1 \text{g}$ IV over 10 min (give within 3 hours of onset).
- Escalation (if uterotonics fail):
- Bimanual uterine compression.
- Intrauterine balloon tamponade (e.g., Bakri balloon).
- Surgical (if conservative measures fail):
- Examination under anesthesia (EUA) to exclude trauma/retained tissue.
- Uterine artery embolization (if stable & available).
- Laparotomy: Compression sutures (e.g., B-Lynch), uterine/ovarian artery ligation, hysterectomy (last resort).
- Always identify & treat the specific 'T' cause.
⭐ Uterine atony accounts for approximately 70-80% of all PPH cases.
Hypertensive Emergencies - Pressure Peril
- Gestational HTN: BP ≥140/90 mmHg post-20wks; no proteinuria.
- Pre-eclampsia: BP ≥140/90 mmHg post-20wks + Proteinuria (≥0.3g/24h or ≥2+) OR end-organ damage.
- Severe features: BP ≥160/110 mmHg, ↓platelets (<100,000/µL), ↑LFTs, ↑Cr, pulm. edema, CNS/visual sx.
- Eclampsia: Pre-eclampsia + Seizures.
- HELLP Syndrome: 📌 Hemolysis (↑LDH), Elevated Liver enzymes, Low Platelets (<100,000/µL).
Management:
- Antihypertensives (BP ≥160/110 mmHg): Labetalol, Nifedipine, Hydralazine.
- MgSO4: Load $4-6g$ IV; Maint $1-2g/hr$. (Therapeutic range: 4-7 mEq/L).
- Toxicity: 📌 BURP (↓BP, ↓Urine output, ↓Resp rate, ↓Patellar reflex). Antidote: Ca Gluconate $1g$ IV.
⭐ MgSO4: Drug of choice for seizure prophylaxis (severe pre-eclampsia) & control (eclampsia).
Obstructed Labor & Cord Events - Passage Problems
- Shoulder Dystocia: Anterior shoulder impaction post-head delivery.
- Risks: Macrosomia, GDM, obesity, prolonged 2nd stage.
- Comps: Maternal (PPH, tears); Fetal (brachial plexus injury, fracture, hypoxia).
- 📌 HELPERR: Help, Episiotomy, Legs (McRoberts), Pressure (suprapubic), Enter (Rubin II, Woodscrew), Remove posterior arm, Roll (Gaskin).
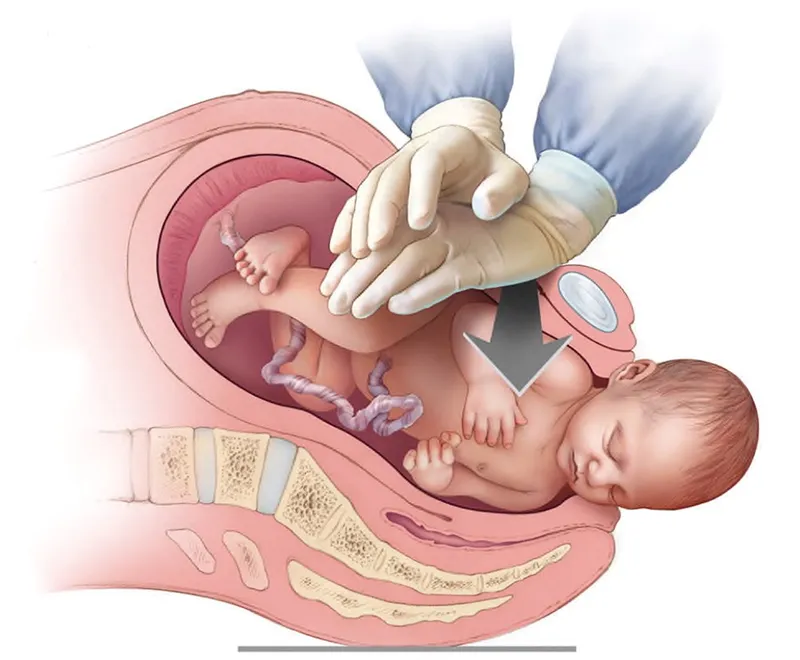
- Cord Prolapse: Cord below presenting part, membranes ruptured.
- Types: Overt, Occult, Funic.
- Risks: Malpresentation, AROM (unengaged head), polyhydramnios.
- Mgmt: Elevate part, knee-chest/Trendelenburg, O2, tocolysis (terbutaline 0.25mg SC), expedite delivery (C-section).

⭐ Cord prolapse: presenting part unengaged, cord slips past.
- Shoulder dystocia: Key maneuvers are McRoberts and suprapubic pressure; HELPERR mnemonic.
- PPH: Uterine atony is #1 cause; manage with uterotonics, then Bakri balloon or B-Lynch.
- Eclampsia: Magnesium sulfate (MgSO4) is vital for seizure prophylaxis and treatment.
- Cord Prolapse: Immediate C-section; elevate presenting part, knee-chest or Trendelenburg.
- Uterine Rupture: Sudden fetal bradycardia, loss of station; urgent laparotomy.
- Amniotic Fluid Embolism: Acute hypoxia, hypotension, coagulopathy; supportive care.
- Vasa Previa: Bleeding post-ROM with fetal distress; emergency C-section.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

