hCG - Pregnancy's Herald
- Structure: Glycoprotein; α-subunit (common to LH, FSH, TSH), β-subunit (unique, confers specificity).
- Synthesis: Syncytiotrophoblast.
- Functions:
- Maintains corpus luteum → progesterone secretion. 📌 hCG 'Heralds Corpus luteum's Goodness'.
- Stimulates fetal testicular testosterone.
- Maternal thyroid stimulation (TSH-like activity).
- Levels:
- Detection: Serum 6-8 days, urine 10-14 days post-conception.
- Doubles: Every 48-72 hrs in early pregnancy.
- Peak: 8-10 weeks (approx. 100,000 mIU/mL).
- Nadir: ~20 weeks, then slight rise.
- Clinical Significance:
- Pregnancy tests (detects β-hCG).
- Ectopic pregnancy: Slower rise/plateau.
- Molar pregnancy (GTD): Very high levels (e.g., >100,000 mIU/mL beyond expected peak).
- Down syndrome screening: ↑ hCG in 2nd trimester.
⭐ β-hCG is highly specific for pregnancy and is used for its detection and monitoring trophoblastic diseases.
if possible to subtly indicate without cluttering main graph)
hPL - Fetal Fuel Manager
- A.k.a.: Human Chorionic Somatomammotropin (hCS). GH/Prolactin-like structure.
- Synthesis: Syncytiotrophoblast.
- Key Functions:
- Maternal: ↑ Lipolysis (↑ FFAs for maternal fuel); induces insulin resistance (diabetogenic, ensures fetal glucose supply).
- Fetal: Stimulates growth (indirectly via IGFs).
- Other: Angiogenesis; mammary gland development (lactogenic).
- Levels: Rise throughout pregnancy, proportional to placental mass.
- Clinical: Low levels may indicate IUGR/placental insufficiency (less used as a primary marker now).
⭐ hPL promotes maternal insulin resistance, shunting glucose to the fetus, and mobilizes free fatty acids for maternal energy use.
Estrogens - Uterine Growth Gurus
- Types: Estrone (E1), Estradiol (E2), Estriol (E3) (major placental estrogen).
- Synthesis: Feto-placental unit. Placenta lacks 17α-hydroxylase & 17,20-desmolase.
- Functions:
- Uterine growth (hypertrophy, hyperplasia)
- ↑ Uteroplacental blood flow
- Breast development (ductal growth)
- Cervical ripening
- ↑ Prostaglandin synthesis
- ↑ Myometrial contractility (late pregnancy)
- ↑ Clotting factors
- Levels: E3 levels ↑ progressively; reflects feto-placental health.
- Clinical Significance: Low maternal serum/urine E3 associated with:
- Fetal distress
- Anencephaly (no fetal pituitary/adrenals)
- Placental sulfatase deficiency
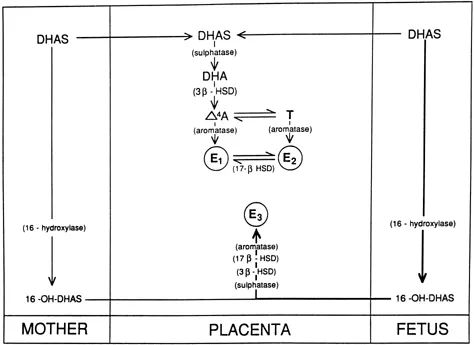
⭐ Estriol (E3) is the predominant estrogen in pregnancy, and its production uniquely depends on the fetal adrenal gland and liver, making it a marker of feto-placental well-being.
Progesterone - Quiescence Keeper
📌 Progesterone 'PROtects GESTation'
- Synthesis:
- Corpus luteum (<8-10 weeks), then placenta (syncytiotrophoblast; from maternal cholesterol).
- Placenta lacks 17α-hydroxylase.
- Functions:
- Maintains uterine quiescence (↓ myometrial excitability, ↓ gap junctions, ↓ PG synthesis).
- Endometrial decidualization.
- Inhibits maternal immune rejection of fetus.
- Breast development (lobuloalveolar).
- Substrate for fetal adrenal corticosteroid synthesis.
- Systemic smooth muscle relaxation.
- Levels: ↑ progressively throughout pregnancy.
- Clinical Significance:
- Luteal phase defect.
- Supplementation in threatened abortion/preterm labor (role debated but used).
⭐ Progesterone is essential for maintaining pregnancy by promoting uterine quiescence and immune tolerance.
Minor Hormones - Supporting Stars
- Relaxin
- Source: Corpus luteum, decidua, placenta.
- Functions: Cervical ripening, pubic symphysis relaxation, systemic vasodilation.
- Placental CRH (Corticotropin-Releasing Hormone)
- Rises late pregnancy.
- Functions: Implicated in parturition timing, fetal lung maturation (via fetal cortisol), uterine contractility.
⭐ Placental Corticotropin-Releasing Hormone (CRH) levels rise exponentially in late pregnancy and are thought to act as a 'placental clock' for parturition timing.
- Placental GH-V (Growth Hormone Variant)
- Functions: Maternal IGF-1 regulation, ↑ maternal insulin resistance, fetal growth.
- Inhibin A & Activin A
- Source: Placenta.
- Functions: Inhibin A used in aneuploidy screening (↑ in Down syndrome); FSH regulation, placental development.
- Kisspeptin
- Functions: Trophoblast invasion, placental development regulation.
High‑Yield Points - ⚡ Biggest Takeaways
- hCG (syncytiotrophoblast): Maintains corpus luteum, peaks 8-10 weeks. Basis of pregnancy tests.
- hPL (hCS): Anti-insulin action, ensures fetal glucose. Levels ↑ with placental size.
- Progesterone: Placenta takes over from ~8 weeks; maintains uterine quiescence.
- Estriol (E3): Major placental estrogen; reflects feto-placental unit health.
- Relaxin: Softens cervix and pelvic ligaments, aiding parturition.
- Inhibin A: Placental hormone, marker in quadruple screen.
- Placental CRH: Levels ↑, may time onset of labor.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more