Morphology & Species - Fungal ID Parade
- Ubiquitous saprophytic molds.
- Key Species:
- Aspergillus fumigatus (most common)
- A. flavus (aflatoxin)
- A. niger (otomycosis, "salt & pepper")
- A. terreus (amphotericin B resistant)
- Microscopic Features:
- Septate hyphae.
- Acute angle (approx. 45°) dichotomous branching. 📌 A for Acute Angle.
- Conidiophore structure: foot cell → vesicle → phialides → chains of conidia.

⭐ Aspergillus fumigatus is the most common species causing human aspergillosis, known for its thermotolerance (can grow at >37°C).
Pathogenesis & Virulence - Spore Invasion Secrets
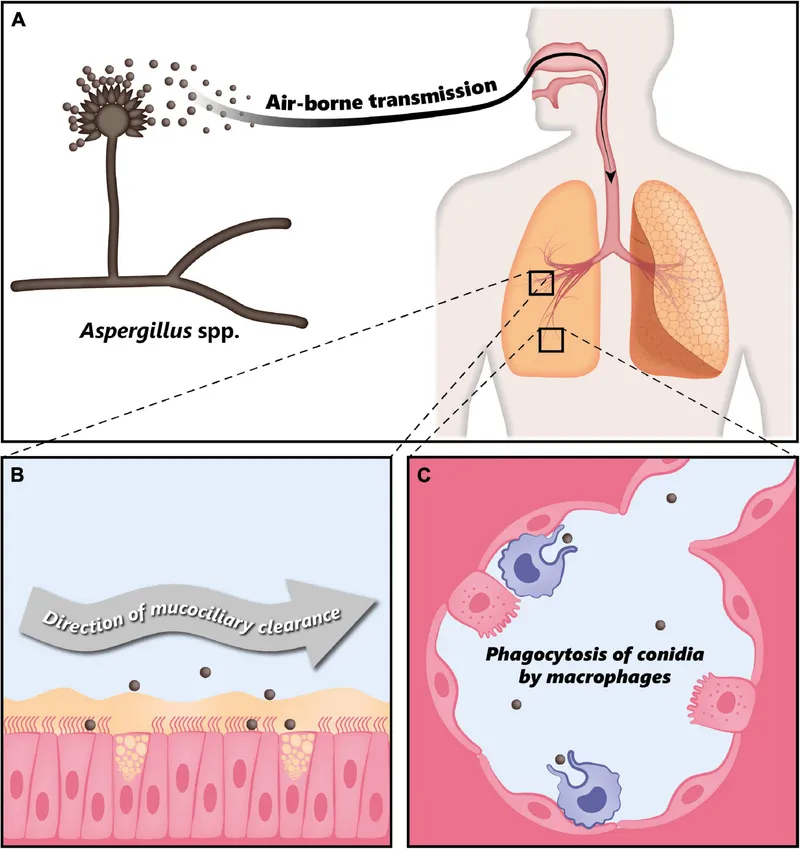
- Entry: Inhalation of Aspergillus conidia.
- Host Factors (↑ Susceptibility): Neutropenia (<500/μL), corticosteroid therapy, Chronic Granulomatous Disease (CGD), immunosuppression.
- Virulence Factors:
- Adhesion: Hydrophobins on conidia aid attachment.
- Survival: Thermotolerance (growth at 37°C); Catalase (resists oxidative stress); Melanin (protects from host defenses, ROS).
- Damage & Spread: Gliotoxin (immunosuppressive, pro-apoptotic); Proteases (elastase, collagenase for tissue invasion).
- Toxin: Aflatoxins (produced by A. flavus, carcinogenic).
⭐ Angioinvasion is a hallmark of Invasive Aspergillosis, leading to tissue infarction and necrosis.
Clinical Syndromes - Aspergillus' Disease Faces
| Syndrome | Host | Key Features | Diagnostic Clues |
|---|---|---|---|
| ABPA | Asthma, Cystic Fibrosis | Type I & III hypersensitivity, eosinophilia, fleeting pulmonary infiltrates | ↑ Total IgE (>1000 IU/mL), Aspergillus specific IgE/IgG, central bronchiectasis (CT) |
| Aspergilloma | Pre-existing lung cavity (e.g., TB, sarcoid) | Fungus ball (colonization), often asymptomatic; hemoptysis | Mobile intracavitary mass on imaging ("Monod sign") |
| Invasive (IA) | Severely Immunocompromised (neutropenia) | Angioinvasion, thrombosis, infarction, necrosis; fever, pneumonia, disseminated | Halo sign, air-crescent sign (CT chest); +ve galactomannan, β-D-glucan; biopsy for definitive diagnosis |
- Cutaneous Aspergillosis: Primary (direct inoculation at trauma sites) or secondary (hematogenous spread in IA) skin lesions (e.g., necrotic ulcers).

⭐ The 'halo sign' (ground-glass opacity surrounding a nodule) on CT chest is an early, albeit non-specific, sign of Invasive Aspergillosis in neutropenic patients.
Diagnosis - Unmasking the Culprit
-
Microscopy: Direct (KOH, Calcofluor); Histopathology (GMS, PAS) shows septate hyphae, acute-angle branching.
- Culture: Sabouraud Dextrose Agar (SDA) - rapid growth, species-specific colonies.
- Antigen Detection:
- Galactomannan (GM) assay (Serum/BAL): Crucial for Invasive Aspergillosis (IA). Index >0.5 often positive.
- (1→3)-β-D-Glucan (BDG): Panfungal.
- Antibody Detection: IgG/IgE (ABPA, CPA).
- Molecular: PCR for Aspergillus DNA.
- Imaging: CXR; CT (halo/air-crescent signs in IA; aspergilloma).
⭐ Detection of Galactomannan antigen in serum or bronchoalveolar lavage (BAL) fluid is a cornerstone in the early diagnosis of Invasive Aspergillosis.
Treatment - Mold Combat Plan
⭐ Voriconazole is the primary drug of choice for the treatment of Invasive Aspergillosis, demonstrating superior efficacy over Amphotericin B in pivotal trials.
High‑Yield Points - ⚡ Biggest Takeaways
- Aspergillus fumigatus is the most frequent species.
- Key morphology: Septate hyphae with acute angle (45°) dichotomous branching.
- Allergic Bronchopulmonary Aspergillosis (ABPA): Associated with asthma/CF, ↑IgE, eosinophilia.
- Aspergilloma: Fungus ball in pre-existing lung cavities (often post-TB).
- Invasive Aspergillosis: Seen in immunocompromised (especially neutropenia); characterized by angioinvasion.
- Diagnosis: Galactomannan antigen (serum/BAL) and β-D-glucan are important markers.
- Voriconazole is the first-line treatment for invasive aspergillosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

