HLA & Graft Basics - Body's ID Check
- HLA (Human Leukocyte Antigen): Body's ID system. Encoded by Major Histocompatibility Complex (MHC) genes on Chromosome 6. Highly polymorphic.
- Class I (HLA-A, B, C): On all nucleated cells. Presents endogenous antigens to CD8+ T cells.
- Class II (HLA-DR, DQ, DP): On Antigen-Presenting Cells (APCs) e.g., macrophages, B-cells, dendritic cells. Presents exogenous antigens to CD4+ T cells.
- Graft Types & Rejection Risk:
- Autograft (self) & Isograft (identical twin): No rejection.
- Allograft (human-to-human, non-identical): Rejection risk. Most common type.
- Xenograft (animal-to-human): High rejection risk.
- HLA matching (especially A, B, DR) is crucial for allograft survival.
⭐ HLA-DR matching has the most significant impact on graft survival for kidney transplants.
Allorecognition Pathways - Immune System's War
Recipient immune system recognizes donor alloantigens (MHCs) as foreign, initiating rejection. Two pathways:
- Direct Allorecognition:
- Recipient T-cells engage intact MHCs on donor APCs.
- Migratory donor APCs (e.g., dendritic cells) reach recipient lymphoid organs.
- Activates CD8+ T-cells (target donor cells via MHC I) & CD4+ T-cells (help via MHC II).
- Dominant in early acute rejection.
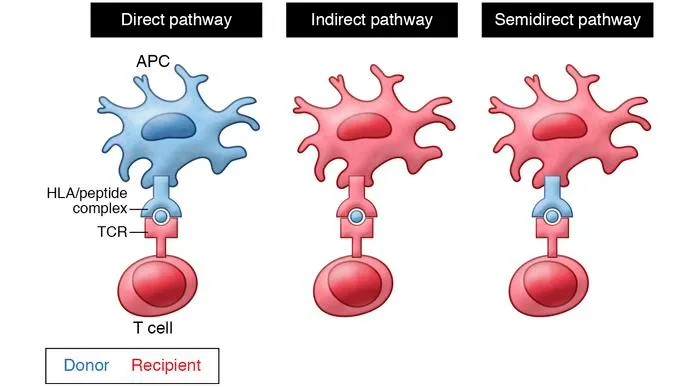
- Indirect Allorecognition:
- Recipient APCs process & present peptides from donor MHC/minor histocompatibility antigens.
- Presented on recipient MHC II to recipient CD4+ T-cells.
- Like conventional antigen presentation.
⭐ Indirect allorecognition, mediated by recipient APCs presenting donor peptides, is key in chronic rejection.
Rejection & GVHD - When Transplants Rebel
Graft Rejection: Host immune system attacks donor organ.
- Hyperacute:
- Mins-hrs; pre-formed anti-donor Abs (ABO, HLA).
- Type II HSR; widespread thrombosis, ischemic necrosis.
- Acute:
- Days-weeks (typically < 6 months).
- Cellular (T-cell, Type IV HSR): Lymphocytic infiltrate.
- Humoral (Ab-mediated, Type II HSR): Vasculitis, C4d.
⭐ C4d deposition in peritubular capillaries is a diagnostic marker for antibody-mediated acute rejection.
- Chronic:
- Months-years; mixed Type III & IV HSR.
- Progressive fibrosis, arteriosclerosis (e.g., Bronchiolitis obliterans - lung).
Graft-versus-Host Disease (GVHD): Donor T-cells attack recipient tissues.
- Common in Bone Marrow/Stem Cell Transplants.
- Key sites: Skin (rash), GIT (diarrhea), Liver (jaundice).
- Acute GVHD: < 100 days post-transplant.
- Chronic GVHD: > 100 days post-transplant.
Immunosuppression - Calling a Truce
- Goal: Prevent host-vs-graft (rejection) & graft-vs-host disease (GVHD).
- Phases & Typical Regimens:
- Induction: Peri-op, potent agents (e.g., Anti-thymocyte Globulin (ATG), Basiliximab).
- Maintenance: Long-term (e.g., Calcineurin Inhibitor (CNI) + Antimetabolite ± Steroids).
- Anti-rejection: High-dose steroids, biologics for acute episodes.
- Core Drug Classes (Mechanism of Action):
- Calcineurin Inhibitors (CNIs): Tacrolimus, Cyclosporine (↓IL-2 synthesis).
- Antiproliferatives: Mycophenolate Mofetil (MMF), Azathioprine (↓lymphocyte proliferation).
- mTOR Inhibitors: Sirolimus, Everolimus (↓IL-2 signaling).
- Corticosteroids: Prednisone (Broad anti-inflammatory effects).
- Biologics (Antibodies): Basiliximab (IL-2R Ab), Rituximab (CD20 Ab for AMR).
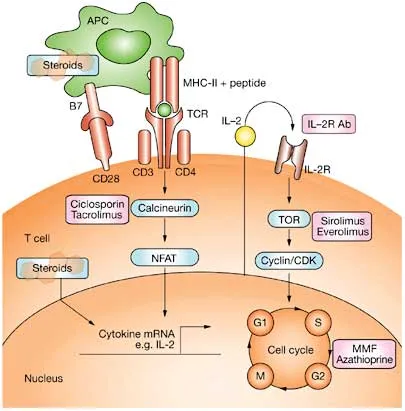
⭐ Tacrolimus and Mycophenolate Mofetil form a common cornerstone of maintenance immunosuppression in solid organ transplantation.
High‑Yield Points - ⚡ Biggest Takeaways
- MHC (HLA) compatibility, especially HLA-DR, is key for graft survival.
- Hyperacute rejection: Minutes to hours; pre-formed anti-donor antibodies (ABO, HLA).
- Acute rejection: Days to weeks; primarily T-cell mediated (Type IV HSR); also antibody-mediated.
- Chronic rejection: Months to years; fibrosis, vascular issues; mixed cellular/humoral.
- GVHD: Donor T-cells attack recipient; common in bone marrow transplants.
- Immunosuppressants (calcineurin inhibitors, steroids) prevent rejection.
- Crossmatching detects pre-formed anti-donor antibodies against donor antigens.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

