Definitions & Types - Gasping for Definitions
- Respiratory Failure (RF): PaO2 < 60 mmHg (hypoxemic) OR PaCO2 > 50 mmHg (hypercapnic) on room air.
| Type | PaO2 | PaCO2 | A-a Grad. | Examples |
|---|---|---|---|---|
| I | ↓ <60 mmHg | Normal / ↓ | ↑ | ARDS, Pneumonia, PE |
| II | Normal / ↓ | ↑ >50 mmHg | Normal | COPD, NMD, Opioids |
| III | ↓ | Variable | ↑ | Atelectasis (Post-op) |
| IV | ↓ | Variable | Variable | Shock (Cardio/Septic) |
⭐ Normal A-a gradient in Type II RF = pure hypoventilation.
Pathophysiology - Why Lungs Stumble
Mechanisms of Impaired Gas Exchange:
- V/Q Mismatch: Most common. Ventilation/perfusion imbalance. Responds to O2.
- Causes: Pneumonia, PE, Asthma, COPD. (📌 P-P-A-C)
- Shunt: Extreme V/Q mismatch; blood bypasses alveoli. Refractory to O2.
- Causes: ARDS, severe pneumonia, cardiac shunts.
- Hypoventilation: ↓Alveolar ventilation → ↑PaCO2, ↓PaO2. Normal A-a gradient.
- Causes: CNS depression, neuromuscular weakness.
- Diffusion Impairment: Thickened alveolar-capillary membrane. Exercise-induced hypoxemia.
- Causes: ILD, emphysema.
- Low Inspired O2: e.g., high altitude. ↓PaO2, normal A-a gradient.
- Alveolar Gas Equation: $P_A O_2 = F_i O_2 (P_B - P_{H_2O}) - P_a CO_2 / R$
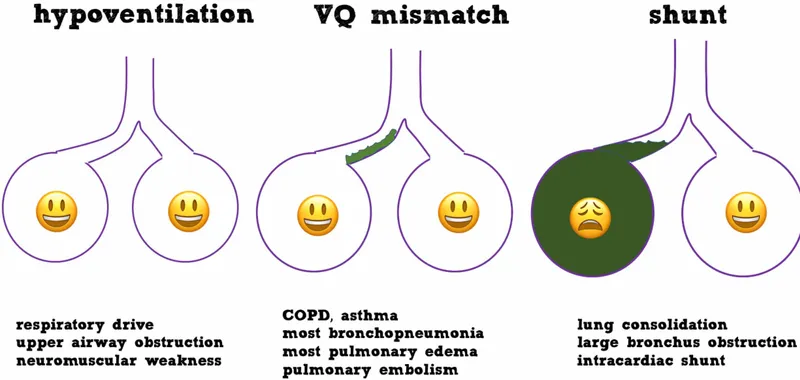
⭐ Normal A-a gradient in hypoxemia suggests hypoventilation or low inspired FiO2.
Clinical Features & Diagnosis - Symptom Sleuthing
- Symptoms: Dyspnea, tachypnea, cyanosis. Altered sensorium (agitation, confusion).
- Type I (Hypoxemic): Restlessness.
- Type II (Hypercapnic): Headache, asterixis.
- A-a Gradient: $P_A O_2 - P_a O_2$. Normal: <15 mmHg.
- ↑ A-a causes: 📌 VSD (V/Q mismatch, Shunt, Diffusion impairment).
- ABG Interpretation:
| Feature | Type I (Hypoxemic) | Type II (Hypercapnic) Acute | Type II (Hypercapnic) Chronic |
|---|---|---|---|
| PaO₂ (mmHg) | ↓↓ (<60) | ↓ / Normal | ↓ / Normal |
| PaCO₂ (mmHg) | Normal / ↓ | ↑↑ (>45) | ↑↑ (>45) |
| pH | Normal / ↑ | ↓↓ | ↓ (near normal) |
| HCO₃⁻ (mEq/L) | Normal | Normal | ↑↑ (Compensated) |
| A-a Gradient | ↑ | Normal / ↑ | Normal / ↑ |
| BE (mEq/L) | Normal | Approx. 0 | ↑↑ |
Management Principles - Airway Allies
- Oxygen Therapy:
- Goal: $PaO_2$ >60 mmHg, SpO2 >90%.
- COPD: Target SpO2 88-92%.
- Devices:
- Nasal Cannula (NC): Low flow, FiO2 24-44%.

- Venturi Mask: Precise FiO2 (24-60%).

- Non-Rebreather Mask (NRBM): High FiO2 (up to 90%).
- Nasal Cannula (NC): Low flow, FiO2 24-44%.
- Non-Invasive Ventilation (NIV):
- Indications: 📌 COPD (pH <7.35, $PaCO_2$ >45 mmHg), ACPE, Immunosuppressed, Post-extubation.
- Contra: Resp arrest, unstable, no airway protection, facial trauma, ↑secretions.
- Mechanical Ventilation (MV):
- Indications: NIV failure/contra, severe hypoxemia ($PaO_2/FiO_2$ <150), resp arrest, airway protection, ↓GCS.
⭐ ARDS: Lung-protective ventilation (LPV) with low tidal volumes (4-6 mL/kg PBW) & $P_{plat}$ <30 $cmH_2O$ improves survival.
Spotlight Cases - ARDS & COPD Alarms
- ARDS (Acute Respiratory Distress Syndrome)
- 📌 BERLIN criteria: Acute onset, bilateral opacities (non-cardiac edema), P/F ratio $\le \textbf{300}$ mmHg with PEEP $\ge \textbf{5}$ cmH2O.
- Severity (P/F mmHg): Mild ($\textbf{201-300}$), Mod ($\textbf{101-200}$), Sev ($\le\textbf{100}$).
- Mgmt: Lung Protective Ventilation (LPV), optimal PEEP, prone positioning.

- COPD Exacerbation with Respiratory Failure
- Triggers: Infections (viral/bacterial), pollutants, non-compliance.
- Mgmt: Controlled O2 (target SpO2 88-92%), nebulized SABA/SAMA, systemic corticosteroids, antibiotics (if indicated). Consider NIV (BiPAP) for RF.
⭐ COPD + Hypercapnic RF: NIV is 1st line ventilation (reduces intubation/mortality).
High‑Yield Points - ⚡ Biggest Takeaways
- Respiratory Failure: PaO₂ < 60 mmHg (Hypoxemic) or PaCO₂ > 50 mmHg (Hypercapnic).
- Type I (Hypoxemic): V/Q mismatch (e.g., Pneumonia, PE); ↑ A-a gradient.
- Type II (Hypercapnic): Alveolar hypoventilation (e.g., COPD, Myasthenia); normal A-a gradient.
- ARDS: Acute onset, bilateral opacities, P/F ratio ≤ 300 mmHg, non-cardiogenic origin.
- Management: O₂ therapy (cautious in Type II), treat underlying cause, mechanical ventilation.
- P/F ratio (PaO₂/FiO₂) assesses hypoxemia severity, crucial in ARDS diagnosis and management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

