Febrile Neutropenia - Fever Pitch Peril
- Definition: Fever (single oral T ≥ 38.3°C or T ≥ 38.0°C sustained ≥1 hr) + Neutropenia (ANC < 500/mm³ or ANC < 1000/mm³ with predicted fall to < 500/mm³).
- Risk Stratification: MASCC score (Multinational Association for Supportive Care in Cancer); score ≥21 indicates low risk, consider outpatient management.
- Common Pathogens: Gram-negative bacilli (Pseudomonas aeruginosa, E. coli), Gram-positive cocci (Staphylococcus aureus, Streptococcus spp.).
- Management: Initiate empiric broad-spectrum antibiotics within 60 minutes.
⭐ The "golden hour": Administer empiric broad-spectrum antibiotics within 60 minutes of presentation to significantly reduce mortality risk in febrile neutropenia patients.
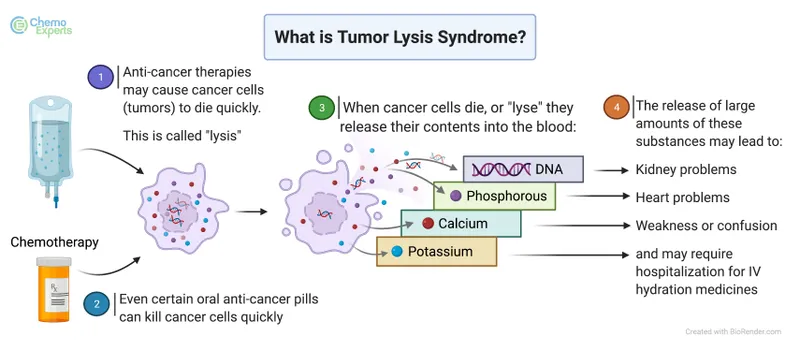
Tumor Lysis Syndrome - Cell Chaos Crisis
Rapid cell lysis releases intracellular contents. High risk: Burkitt, ALL/AML, bulky tumors post-chemo. 📌 Mnemonic: K-PUNCH (K⁺↑, Phosphate↑, Uric acid↑, Nucleotides↑, Ca²⁺↓, Hydration).
- Lab TLS (Cairo-Bishop):
- Uric acid >8 mg/dL
- K⁺ >6 mEq/L
- PO₄³⁻ >4.5 mg/dL
- Ca²⁺ <7 mg/dL
- Clinical TLS: Lab TLS + AKI (Cr >1.5x ULN), arrhythmia, seizure.
- Management:
- Aggressive IV hydration (2-3 L/m²/day).
- Allopurinol; Rasburicase (0.2 mg/kg) if high-risk/uric acid ↑↑.
- Correct electrolytes; dialysis if needed.
⭐ Rasburicase is contraindicated in G6PD deficiency due to risk of severe hemolysis.
Spinal Cord Compression - Nerve Wreckage
Oncologic emergency from tumor pressure on spinal cord/cauda equina.
- Etiology: Lung, breast, prostate cancer; myeloma, lymphoma.
- Clinical:
- Back pain (>90%): Earliest, worse supine/night, radicular.
- Motor weakness, sensory deficits (progressive).
- Autonomic dysfunction (late): Bladder/bowel.
- Diagnosis: MRI whole spine (gold standard).
- Management:
- Steroids: Dexamethasone (e.g., **10 mg** IV bolus, then **4-6 mg** q6h or higher doses like **16-96 mg/day**).
- Definitive: RT, surgery, or chemo based on tumor/stability.
⭐ Back pain is the earliest symptom (>90%), often preceding neurological deficits by weeks. Prompt MRI is crucial.

Hypercalcemia of Malignancy - Calcium Calamity
- Serum Ca > 10.5 mg/dL (ionized > 1.3 mmol/L). Severe: > 14 mg/dL.
- Pathophys: PTHrP (80%, squamous cell Ca), local osteolysis (breast Ca, myeloma), ↑Vit D (lymphoma).
- Sx: 📌 "Stones, bones, groans, thrones, psychiatric overtones". ECG: Short QT.
- Rx:
- Initial: IVF (NS 3-6L/24h). Furosemide post-IVF.
- Specific: Bisphosphonates (Zoledronate 4mg IV). Calcitonin (rapid ↓Ca). Denosumab (refractory).
⭐ Bisphosphonates (e.g., Zoledronic acid) are cornerstone; onset 2-4 days, nadir 4-7 days.
Superior Vena Cava Syndrome - Vascular Vexation
Obstruction of SVC blood flow, often by external compression or internal thrombosis.
- Etiology:
- Malignancy (~90%): Lung cancer (esp. SCLC), lymphoma, metastases.
- Benign: Catheter-related thrombosis, fibrosing mediastinitis.
- Features: 📌 "3 D's": Dyspnea, Distended neck/chest veins, Disfigurement (facial/arm edema, plethora). Pemberton's sign.

- Diagnosis: CT chest with contrast. Histopathology essential.
- Management:
- Supportive: Head elevation, O2, corticosteroids (e.g., dexamethasone).
- Definitive: RT, chemotherapy, SVC stenting for rapid relief.
⭐ SCLC is a frequent malignant cause of SVCS.
High‑Yield Points - ⚡ Biggest Takeaways
- Febrile neutropenia: ANC < 500/µL + fever. Immediate broad-spectrum antibiotics are crucial.
- Tumor Lysis Syndrome (TLS): Key features: hyperkalemia, hyperuricemia, hyperphosphatemia, hypocalcemia. Prophylaxis/treatment: hydration, allopurinol/rasburicase.
- SVC Syndrome: Facial/arm swelling, dyspnea. Common with lung cancer. Treat with steroids, radiotherapy.
- Spinal Cord Compression: Back pain, weakness. MRI is diagnostic. Immediate steroids, radiotherapy/surgery.
- Hypercalcemia of Malignancy: Most common paraneoplastic. Treat with hydration, bisphosphonates, calcitonin.
- SIADH: Euvolemic hyponatremia, often with SCLC. Management: fluid restriction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

