Demyelinating Diseases: Overview - Myelin Under Siege

- Definition: Pathological process causing loss or damage to myelin, the protective sheath around nerve fibers.
- Impact: Disrupts nerve impulse conduction → neurological deficits.
- Sites & Cells:
- Central Nervous System (CNS): Oligodendrocytes targeted.
- Peripheral Nervous System (PNS): Schwann cells affected.
- Types:
- Primary: Myelin or myelin-forming cells are direct targets (e.g., MS).
- Secondary: Axonal damage leads to myelin loss.
- Mechanisms: Often immune-mediated; also viral, ischemic, metabolic, toxic.
⭐ Multiple Sclerosis (MS) is the most common demyelinating disease of the CNS, primarily affecting young adults, especially women (F:M ≈ 2-3:1).
Multiple Sclerosis (MS) - The Great Masquerader
- Autoimmune CNS demyelination & axonal damage. Peak 20-40 yrs, F>M.
- Presentation: Symptoms disseminated in time & space.
- Optic neuritis (painful vision loss, Uhthoff's phenomenon), Internuclear ophthalmoplegia (INO).
- Lhermitte's sign (electric shock on neck flexion), sensory loss, motor weakness, spasticity.
- Cerebellar ataxia, fatigue, bladder/bowel issues.
- Diagnosis: McDonald Criteria (clinical + MRI).
- MRI: Periventricular (Dawson's fingers), juxtacortical, infratentorial, spinal lesions. Gadolinium+ = active.

- CSF: Oligoclonal bands (OCBs), ↑IgG index.
- MRI: Periventricular (Dawson's fingers), juxtacortical, infratentorial, spinal lesions. Gadolinium+ = active.
- Management:
- Acute relapse: IV Methylprednisolone.
- Disease-Modifying Therapies (DMTs): Interferons, Glatiramer acetate, Fingolimod, Natalizumab, Ocrelizumab.
- Symptomatic: Spasticity (Baclofen), Fatigue (Amantadine).
- 📌 McDonald Criteria: Dissemination In Time and Space (DITS).
⭐ Oligoclonal bands in CSF are present in >95% of MS patients but are not specific.
NMOSD & ADEM - MS Mimics & More
Key MS mimics; distinct antibodies, features, and management.

| Feature | NMOSD (Neuromyelitis Optica Spectrum Disorder) | ADEM (Acute Disseminated Encephalomyelitis) |
|---|---|---|
| Antibodies | AQP4-IgG (+), MOG-IgG | None (post-infectious/vaccinial) |
| Course | Relapsing | Monophasic; encephalopathy common |
| Key Sites | Optic nerves (severe, bilateral), Spinal cord (LETM >3 seg), Area postrema | Brain (widespread, large WM lesions; deep grey matter), Spinal cord |
| CSF OCBs | Usually negative | Usually negative |
| MRI Brain | Periependymal, area postrema; often normal early | Multiple, large (>1-2 cm), asymmetric WM lesions; basal ganglia/thalami |
| Rx (Acute) | Steroids, PLEX | Steroids; IVIG/PLEX (severe) |
| Rx (Chronic) | Immunosuppression (Rituximab) | Usually not needed |
- 📌 NMO: Not MS, Optic nerve & cord focus.
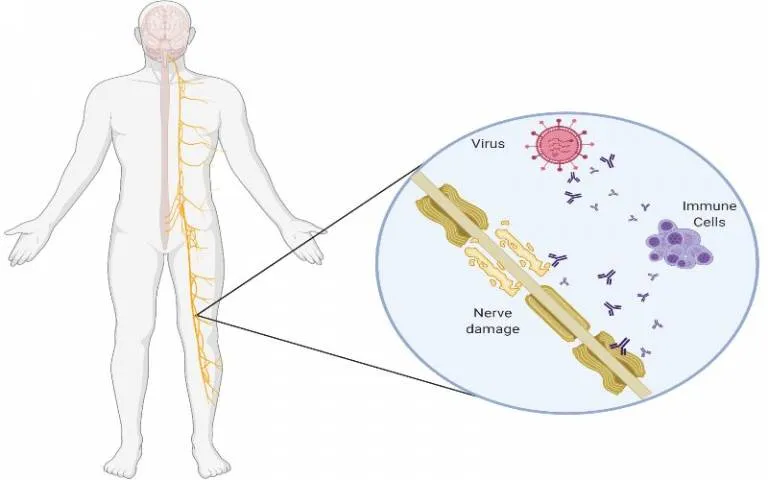
Guillain-Barré Syndrome (GBS) - Nerve Strippers
- Acute immune-mediated polyradiculoneuropathy, often post-Campylobacter jejuni infection.
- Pathophys: Molecular mimicry; antibodies (anti-GM1, anti-GD1a) target peripheral nerve myelin/axons.
- Key Features: Rapidly progressive, symmetrical ascending weakness/paralysis; areflexia/hyporeflexia.
- Sensory symptoms (paresthesia, pain).
- Autonomic dysfunction (tachycardia, BP changes).
- Cranial nerve involvement (e.g., facial palsy); respiratory failure risk (monitor FVC).
- Variants:
- Miller Fisher Syndrome (MFS): Ophthalmoplegia, ataxia, areflexia (anti-GQ1b Ab).
- Diagnosis:
- CSF: Albuminocytologic dissociation (↑ protein, normal cells) - typically after 1 week.
- NCS/EMG: Demyelinating features (↓ conduction velocity).
⭐ Albuminocytologic dissociation in CSF (↑ protein, normal cells) is a classic diagnostic hallmark, usually appearing 1-2 weeks post-symptom onset.
- Treatment: IVIG or Plasma Exchange (PLEX). Supportive care crucial. Steroids NOT effective. 📌 Gradual Bilateral Symmetrical weakness.
High-Yield Points - ⚡ Biggest Takeaways
- Multiple Sclerosis (MS): Oligoclonal bands (CSF), periventricular plaques (MRI). Key signs: Uhthoff's, Lhermitte's.
- Optic Neuritis: Common MS onset; painful monocular vision loss, Marcus Gunn pupil.
- Neuromyelitis Optica (NMO): AQP4-IgG+; severe optic neuritis & longitudinal transverse myelitis (LETM).
- Acute Disseminated Encephalomyelitis (ADEM): Monophasic, post-infectious/vaccinial (children); diffuse white matter lesions.
- Guillain-Barré Syndrome (GBS): Ascending paralysis, areflexia; CSF: albuminocytologic dissociation (↑protein, normal cells).
- Progressive Multifocal Leukoencephalopathy (PML): JC virus in immunocompromised; non-enhancing white matter lesions on MRI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

