Diagnostic Tests - Numbers Game
- Basis: 2x2 table (Disease vs. Test: TP, FP, FN, TN).
- Sensitivity (Sn): $TP / (TP+FN)$. Detects disease.
- 📌 SNOUT: Sensitive test, Negative result, rules OUT.
- Specificity (Sp): $TN / (TN+FP)$. Confirms absence.
- 📌 SPIN: Specific test, Positive result, rules IN.
- PPV (Positive Predictive Value): $TP / (TP+FP)$. Prob. disease if test +ve. Varies with prevalence.
- NPV (Negative Predictive Value): $TN / (TN+FN)$. Prob. no disease if test -ve. Varies with prevalence.
- Likelihood Ratios (LR): Link pre- to post-test probability.
- LR+: $Sn / (1-Sp)$. >10 strong for disease.
- LR-: $(1-Sn) / Sp$. <0.1 strong against disease.

⭐ Prevalence ↑ → PPV ↑, NPV ↓.
Decision Thresholds - Choice Points
- Critical probability points guiding decisions: withhold action, test, or treat.
- Test Threshold ($T_{test}$):
- If P(Disease) < $T_{test}$: No further testing or treatment. Disease considered ruled out.
- Treatment Threshold ($T_{treat}$):
- If P(Disease) > $T_{treat}$: Initiate treatment empirically. Disease considered ruled in.
- Test-Treat Zone:
- If $T_{test}$ ≤ P(Disease) ≤ $T_{treat}$: Optimal to perform diagnostic testing.
- Influencing factors:
- Disease: Prevalence, severity.
- Test: Accuracy (Sn, Sp), risks, cost.
- Treatment: Efficacy, risks, benefits, cost.
⭐ The treatment threshold ($T_{treat}$) is lowered by ↑disease severity, ↑treatment efficacy, or ↓treatment risk.

Clinical Scores & EBM - Evidence Edge
- Clinical Scores: Objectify risk/diagnosis (e.g., Wells' for DVT/PE, CURB-65 for pneumonia severity).
- Metrics: Sensitivity $TP/(TP+FN)$, Specificity $TN/(TN+FP)$.
- PPV $TP/(TP+FP)$, NPV $TN/(TN+FN)$.
- Likelihood Ratios: $LR+ = Sens/(1-Spec)$; $LR- = (1-Sens)/Spec$.
- EBM: Integrates best evidence, clinical expertise, patient values.
- PICO: Patient, Intervention, Comparison, Outcome.
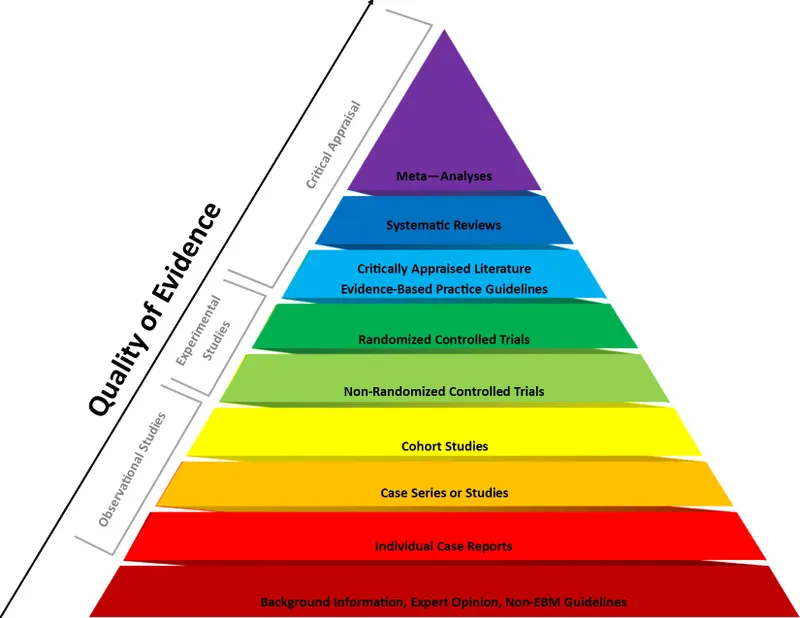
- Hierarchy (Top to Bottom): Meta-analysis/Systematic Review → RCT → Cohort → Case-Control → Case Series → Expert Opinion.
- Key EBM stat: Number Needed to Treat (NNT) = $1/ARR$.
- 📌 FINER criteria (Research Q): Feasible, Interesting, Novel, Ethical, Relevant.
⭐ Odds Ratio (OR) is used in case-control studies; Relative Risk (RR) in cohort studies. For rare diseases ($prevalence < 10%$), $OR \approx RR$
Cognitive Biases & SDM - Mind Matters
- Cognitive Biases: Systematic thinking errors impairing clinical judgment.
- Anchoring: Over-relying on initial info.
- Availability: Overestimating based on easily recalled examples.
- Confirmation: Seeking info confirming existing beliefs.
- Premature Closure: Accepting diagnosis early, missing alternatives.
- Framing Effect: Decisions influenced by info presentation.
- Mitigation: Metacognition, checklists, second opinions.
- Shared Decision Making (SDM): Clinicians and patients collaboratively make healthcare decisions.
- Involves discussing options, evidence, benefits/risks.
- Aligns care with patient values and preferences.
- Improves satisfaction and adherence. 📌 Remember "BRAN": Benefits, Risks, Alternatives, Nothing.
⭐ SDM is not just an option but an ethical imperative in patient-centered care.
High‑Yield Points - ⚡ Biggest Takeaways
- Bayes' Theorem is crucial for post-test probability calculation using likelihood ratios.
- Understand Sensitivity (Sn), Specificity (Sp), PPV, and NPV for test interpretation.
- ROC curves help compare diagnostic tests; Area Under Curve (AUC) quantifies overall accuracy.
- Decision analysis often employs decision trees to model choices and potential outcomes.
- The threshold model (test/treat thresholds) guides diagnostic and therapeutic actions.
- Recognize common cognitive biases (e.g., anchoring, availability) that can affect clinical judgment.
- Apply Evidence-Based Medicine (EBM) principles, respecting the hierarchy of evidence for decisions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

