Liver Injury & Jaundice Basics - Yellow Peril Primer
- Liver Injury Markers:
- Hepatocellular: ↑ALT (📌 Alanine Transaminase - more Liver specific), ↑AST. De Ritis ratio ($AST/ALT$) >2 suggests alcoholic liver disease.
- Cholestatic: ↑ALP, ↑GGT, ↑Conjugated Bilirubin.
- Jaundice: Yellow hue (sclera, skin) if serum bilirubin >2.5-3 mg/dL.
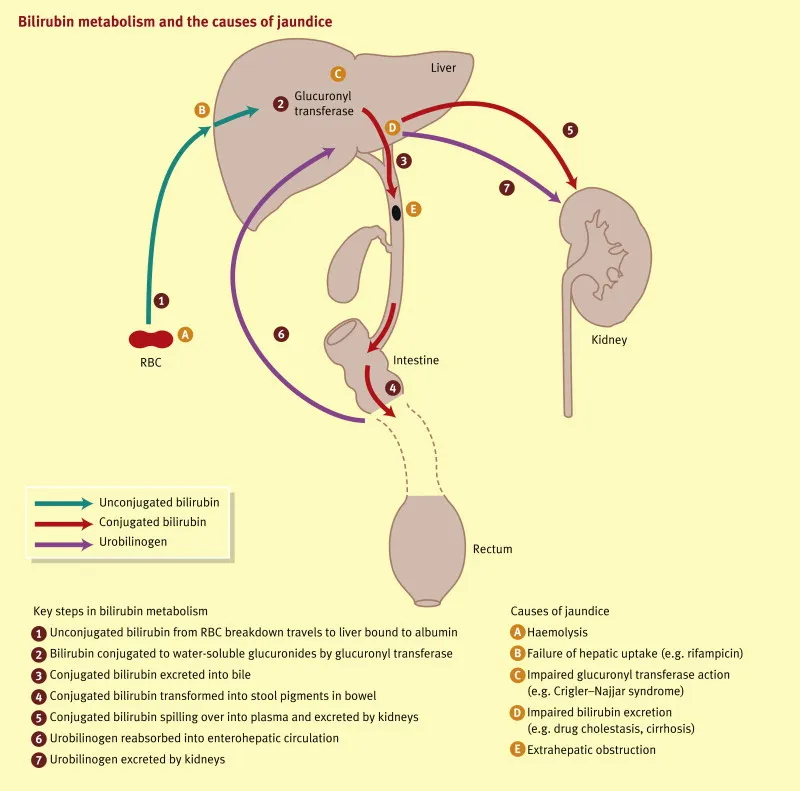
- Approach to Jaundice:
⭐ Gilbert's syndrome: Common, benign; mild unconjugated hyperbilirubinemia due to ↓ UDP-glucuronyltransferase activity, often provoked by fasting/illness.
Cirrhosis Path & Problems - Scarred Liver Saga
- Pathophysiology: Irreversible fibrosis, nodule formation. Stellate cell activation → collagen deposition.
- Etiologies (India Focus):
- 📌 VWHAPPENS: Viral (HBV, HCV), Wilson's/ Hemochromatosis, Autoimmune hepatitis, PSC/PBC, NASH/NAFLD, Ethanol, Something else (e.g., drugs, Budd-Chiari).
- Severity Scoring:
- Child-Pugh Score: Components (Bilirubin, Albumin, INR, Ascites, Encephalopathy - 📌 BEA AI). Score: 5-6 (Class A), 7-9 (Class B), 10-15 (Class C).
- MELD Score: $3.78 \times \ln(\text{Bilirubin mg/dL}) + 11.2 \times \ln(\text{INR}) + 9.57 \times \ln(\text{Creatinine mg/dL}) + 6.43$. Predicts 3-month mortality.
- Key Problems: Portal hypertension (varices, ascites, SBP), hepatic encephalopathy, hepatorenal syndrome, HCC.
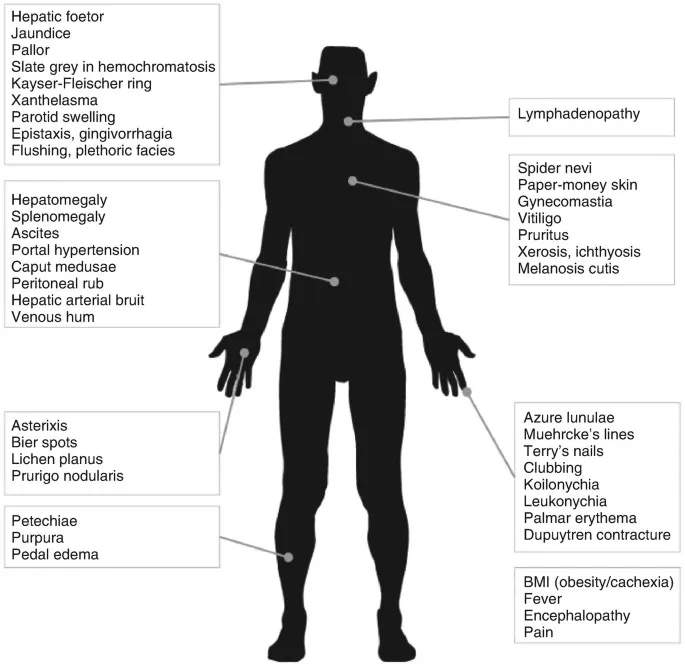
⭐ Most common causes of cirrhosis in India: Alcohol, Viral Hepatitis (HBV, HCV), and NAFLD (Non-Alcoholic Fatty Liver Disease).
Cirrhosis Complications Pt 1 - Pressure Cooker Effects
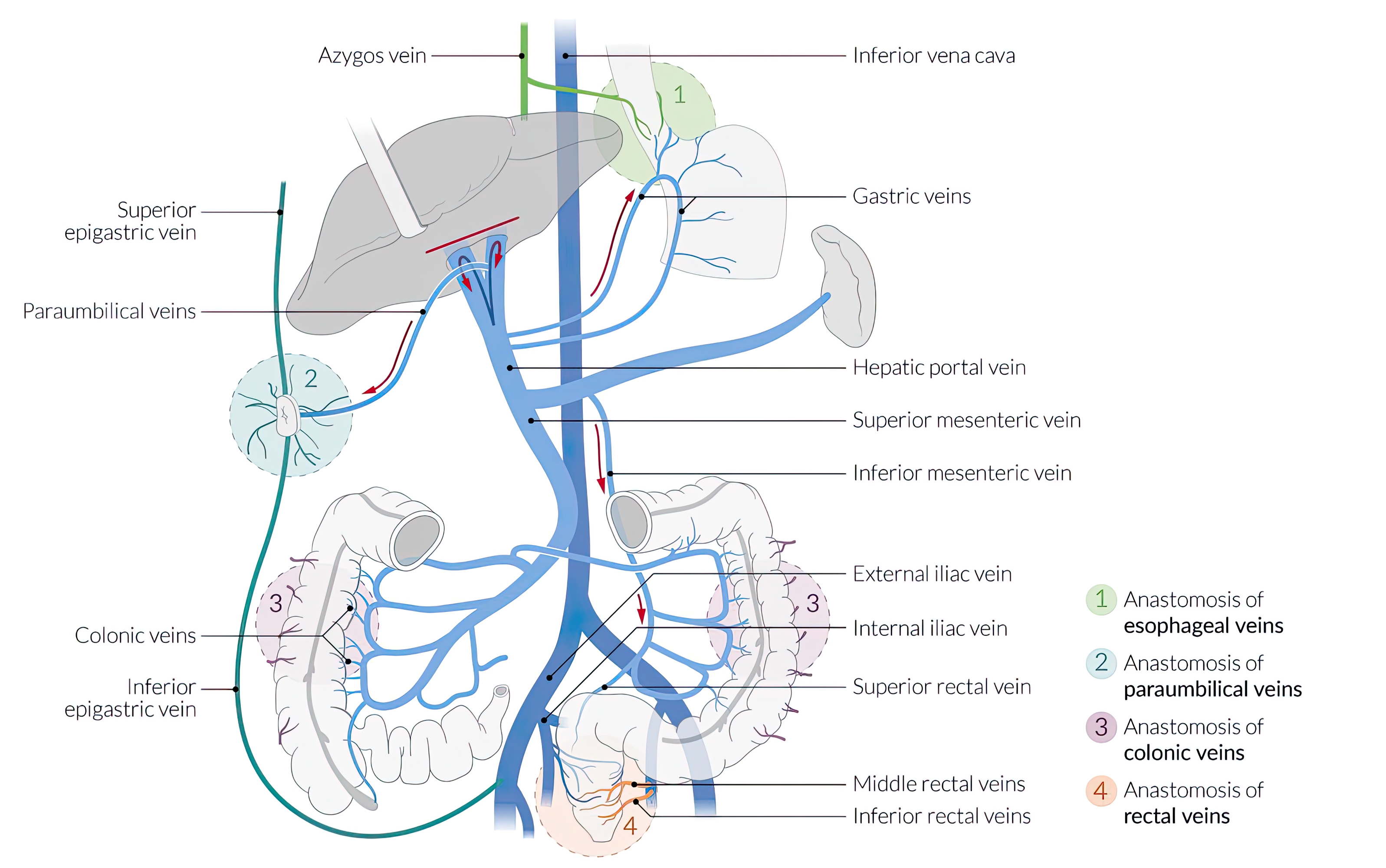
- Portal Hypertension (PHT): HVPG > 5 mmHg (clinically significant > 10 mmHg). Effects:
- Varices: Esophageal (most common), gastric. Bleed risk: size, red signs, Child C.
- Acute Bleed Management:
- Varices: Esophageal (most common), gastric. Bleed risk: size, red signs, Child C.
- **Ascites**: Pathophys: PHT → splanchnic vasodilation → RAAS activation → Na+/water retention.
+ Diagnosis: SAAG > **1.1 g/dL**.
+ Management: Na+ restriction (<**2g/d**), Diuretics (Spironolactone ± Furosemide).
- **Spontaneous Bacterial Peritonitis (SBP)**: Infection of ascitic fluid.
+ Diagnosis: Ascitic PMN > **250 cells/mm³** (+ culture).
+ Treatment: IV Cefotaxime.
> ⭐ SBP Prophylaxis (Norfloxacin): High-risk (prior SBP; or ascites protein < **1.5 g/dL** + severe liver/renal dysfunction).
Cirrhosis Complications Pt 2 & Management - Brain Fog & Beyond
-
Hepatic Encephalopathy (HE): Neuropsychiatric; ↑ammonia.
- Grades 0-4 (West-Haven).
- 📌 Precipitating factors (HIDALGO): Hypokalemia, Infection, Dehydration, Azotemia, Lactulose non-compliance, GI bleed, Other sedatives.
- Management:
- Lactulose 30-45ml TID (target 2-3 soft stools/day).
- Rifaximin 550mg BID (add-on/recurrent).
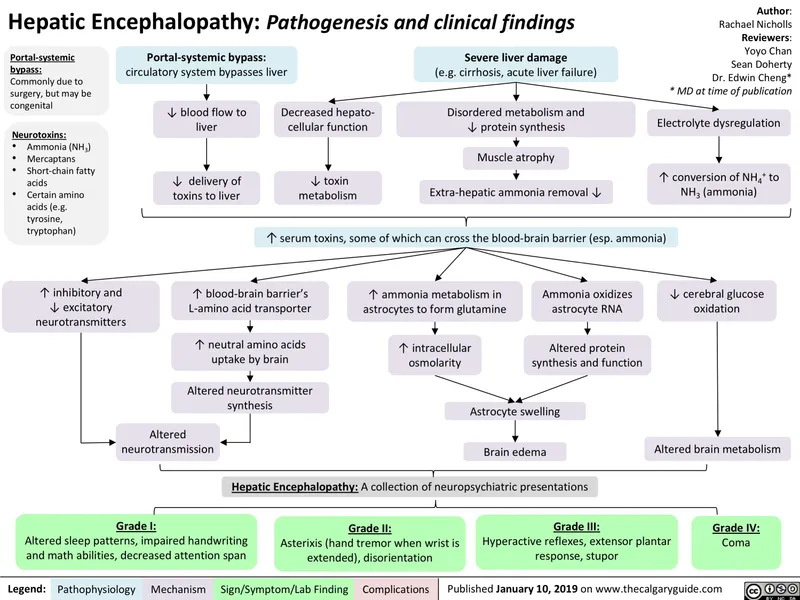
- HE Management:
-
Hepatorenal Syndrome (HRS): Functional renal failure.
- Type 1: Rapid (sCr >2.5 mg/dL in <2wks).
- Type 2: Slower, refractory ascites.
- Management: Albumin + Vasoconstrictors (Terlipressin/Noradrenaline).
-
Hepatopulmonary Syndrome (HPS): Intrapulmonary vascular dilatations + hypoxemia.
-
Portopulmonary Hypertension (POPH): PAH with portal HTN.
⭐ HCC Screening: Ultrasound +/- AFP every 6 months in cirrhotic patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Child-Pugh & MELD scores assess cirrhosis severity and prognosis.
- SBP diagnosis: ascitic fluid PMN > 250/mm³; treat with cefotaxime.
- Hepatic encephalopathy precipitated by infections/GI bleed; manage with lactulose/rifaximin.
- Interpret Hepatitis B serology (HBsAg, anti-HBs, anti-HBc) accurately.
- Screen for HCC in cirrhotics with ultrasound +/- AFP every 6 months.
- Manage acute variceal bleeding with vasoactive drugs and endoscopic therapy.
- Paracetamol and ATT drugs are common causes of DILI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

