Esophageal Motility Disorders - Choke & Spasm Tales
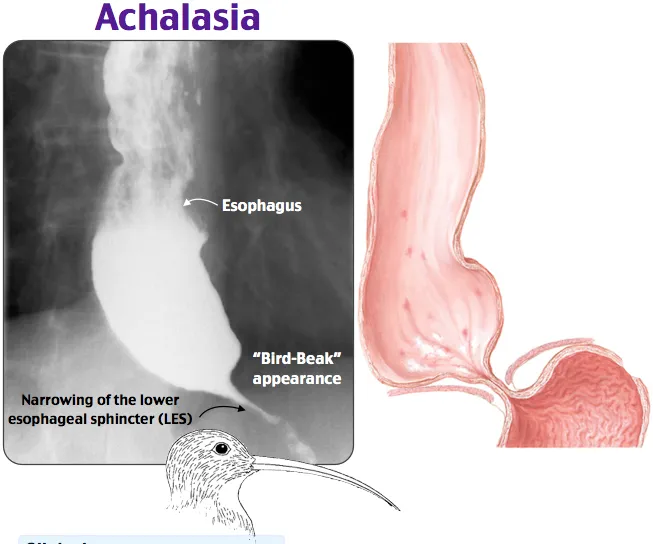
- Achalasia: Failure of LES relaxation & aperistalsis.
- Patho: Myenteric plexus ganglion cell loss.
- Sx: Dysphagia (solids & liquids), regurgitation, chest pain, weight loss.
- Dx: Barium (bird's beak), Manometry (gold: ↑LES pressure, incomplete relaxation, aperistalsis).
- Rx: Dilation, Myotomy, Botox, POEM.
- 📌 ABCDE: Achalasia, Bird's beak, Chest pain/Chagas, Dysphagia, ES (LES) non-relaxation.
- Diffuse Esophageal Spasm (DES): Uncoordinated, high-amplitude contractions.
- Sx: Intermittent dysphagia, chest pain (angina mimic).
- Dx: Manometry (simultaneous, non-peristaltic contractions), Barium (corkscrew).
- Nutcracker Esophagus (Hypertensive Peristalsis):
- Sx: Dysphagia, chest pain.
- Dx: Manometry (peristaltic contractions >180 mmHg).
- Hypertensive LES:
- Dx: Manometry (↑LES pressure >45 mmHg, normal relaxation/peristalsis).
- Ineffective Esophageal Motility (IEM):
- Dx: Manometry (distal amplitude <30 mmHg in ≥50% swallows).
⭐ Manometry is the gold standard for diagnosing esophageal motility disorders.
Gastric Motility Disorders - Stomach Standstills
- Gastroparesis: Delayed gastric emptying (GE) sans mechanical obstruction.
- Causes: Diabetes (commonest), post-surgical, idiopathic, meds (opioids, anticholinergics).
- Sx: Nausea, vomiting (undigested food), early satiety, bloating, abd. pain.
- Diagnosis:
- R/O obstruction (endoscopy/imaging).
- Gold Std: Gastric emptying scintigraphy (GES). Abnormal: >60% retention at 2h or >10% at 4h.
- Management:
- Diet: Small, frequent, low-fat/fiber meals; liquids if severe.
- Prokinetics: Metoclopramide (⚠️ tardive dyskinesia), Domperidone, Erythromycin (motilin agonist, tachyphylaxis).
- Antiemetics.
- Advanced: Botulinum toxin, G-POEM (Gastric Peroral Endoscopic Myotomy), gastric electrical stimulation.
⭐ Diabetic gastroparesis is a frequent complication of diabetes, often linked to autonomic neuropathy. oka
Intestinal Motility Disorders - Bowel Bedlam
-
Irritable Bowel Syndrome (IBS): Recurrent abdominal pain (≥1 day/week, last 3 months) + ≥2 of: related to defecation, change in stool frequency, change in stool form (Bristol Stool Chart). Subtypes: IBS-C, IBS-D, IBS-M. Management: Lifestyle, diet (low FODMAP), fiber, antispasmodics (e.g., dicyclomine), loperamide/lubiprostone, TCAs.
⭐ Rome IV criteria are key for IBS diagnosis.
-
Small Intestinal Bacterial Overgrowth (SIBO): Causes: Motility disorders, anatomical changes, ↓acid. Symptoms: Bloating, diarrhea, malabsorption (B12↓, fat-soluble vit↓). Diagnosis: Glucose/Lactulose breath test (H₂/CH₄ ↑). Gold std: Jejunal aspirate (>10^3 CFU/mL). Treatment: Rifaximin.
-
Chronic Intestinal Pseudo-obstruction (CIPO): Severe dysmotility mimicking obstruction; no mechanical block. Types: Neuropathic, Myopathic. Diagnosis: Manometry, biopsy. Management: Supportive, prokinetics.
GI Motility Diagnostics & General Rx - Test & Treat Tactics
- Key Diagnostics:
- Manometry (esophageal, anorectal): Assesses pressures, sphincter function.
- Transit Studies: Gastric Emptying Scintigraphy (GES), Wireless Motility Capsule (WMC), Sitz markers.
- Endoscopy/Biopsy: Rule out mechanical obstruction, mucosal disease.
- Breath Tests (e.g., H₂): Detect SIBO, malabsorption.
- General Rx Principles:
- Dietary: Small frequent meals, low FODMAP, fiber modulation.
- Pharmacotherapy:
- Prokinetics (e.g., metoclopramide, prucalopride).
- Antispasmodics (e.g., dicyclomine).
- Neuromodulators (e.g., TCAs, SSRIs) for pain/visceral hypersensitivity.
- Biofeedback: For pelvic floor dyssynergia.
- Empiric trials common.
⭐ Gastric Emptying Scintigraphy (GES) is the gold standard for diagnosing gastroparesis; solid meal retention >60% at 2 hours or >10% at 4 hours is diagnostic.
High‑Yield Points - ⚡ Biggest Takeaways
- Achalasia: Bird-beak sign, impaired LES relaxation, dysphagia to solids & liquids.
- GERD: Due to transient LES relaxations; PPIs are mainstay treatment.
- Gastroparesis: Delayed gastric emptying (no obstruction), common in diabetes; causes nausea, vomiting.
- IBS: Diagnosed by Rome criteria; abdominal pain linked to defecation, altered bowel habits.
- Ogilvie's syndrome: Acute colonic pseudo-obstruction with massive dilation, no mechanical block.
- Scleroderma esophagus: Features aperistalsis and patulous LES, leading to severe reflux.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

